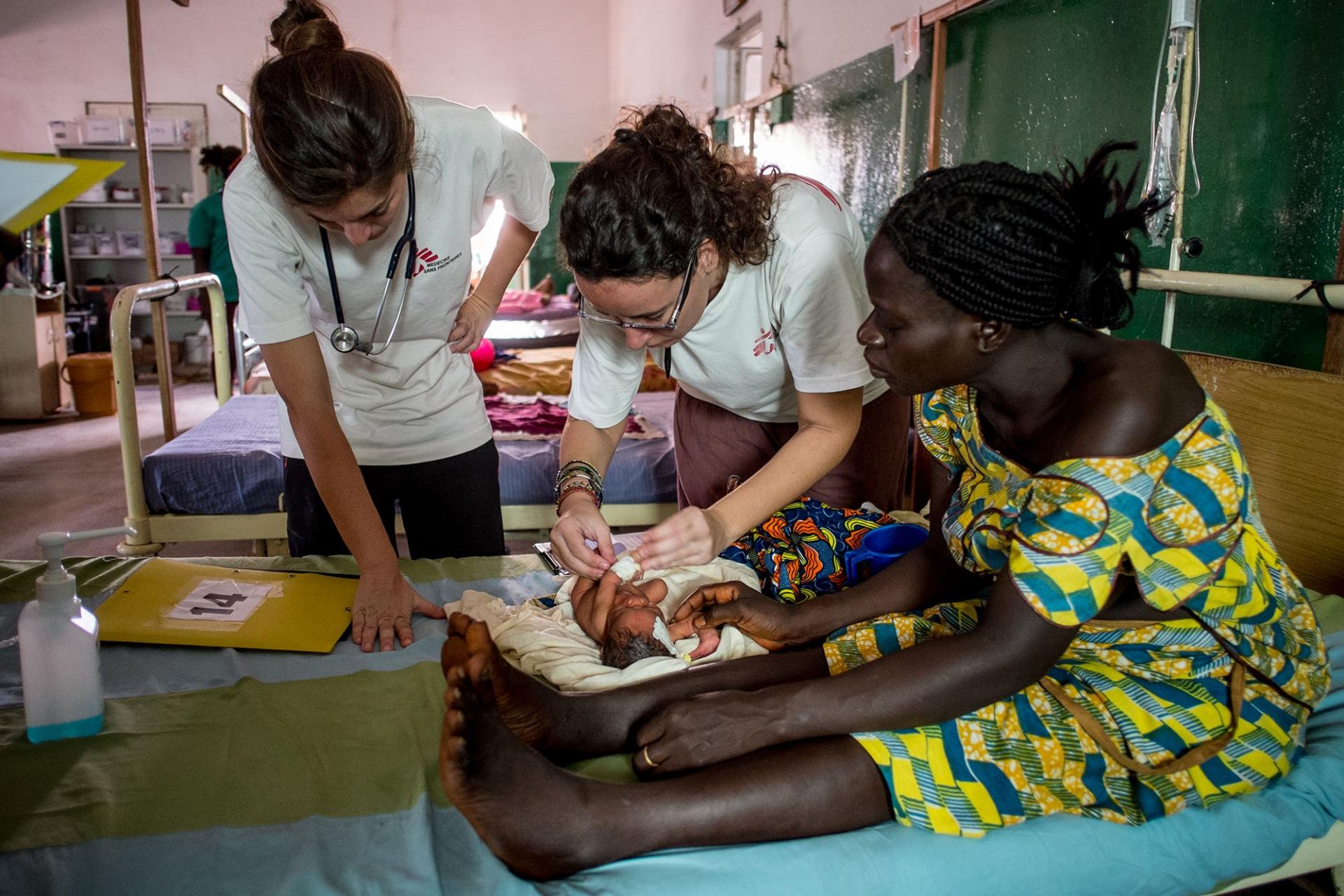
In November 2014, Doctors Without Borders (MSF) launched a pediatric project in the region of Bafatá in central Guinea-Bissau. With an infant mortality rate of 116 per 1,000 children, Guinea-Bissau is among the 10 countries with the worst maternal and child health indicators in the world. Here, Isabel Grovas, the MSF medical coordinator in charge of opening the project, discusses the situation.
Why a paediatric health project in Guinea-Bissau?
Firstly, because the infant mortality figures are alarming, not to mention the fact that many deaths are not registered because many children do not even reach health centres, but die in their own homes.
In addition, Guinea-Bissau’s health system has some major deficiencies: you have to pay a high price for health services, there are often no medicines and there is also a lack of qualified medical personnel.
Just to get an idea, when the first MSF paediatrician arrived, we were only aware of one other in the country.
We now know that there are a few more but they are still very few to cover the needs. In this context, with a very fragile health system, any free, quality medical activity we offer has a great impact on the health of mothers and their children.
What health scenario have you found in the country?
The country suffered a coup in 2012 which considerably worsened the health status of the population. Although there has now been a legitimate government since May 2014, these have been difficult years in which health centres, having already endured a very precarious situation, ran out of resources.
It has been months since many health workers have received any wages, which has affected their motivation and the care they provide.
To this, we must add the lack of international aid, as the major donors ceased their financial contributions due to political instability. In addition to this, the poor harvests of the past two years have forced people to sell what they grow at much lower prices than in previous years.
Much of the population ceased to have sufficient financial resources, and in a context where you have to pay for access to healthcare, no money means no health.
What are the main needs of the child population in Guinea-Bissau?
Many mothers do not go to health centres when their children are sick. In the context of such a weak health system, any sick child faces major difficulties no matter how simple their illness might be to treat: long distances to get to the nearest health centre, the absence of skilled health personnel, lack of medicines, uncertain diagnosis and the high cost of medical consultations.
This means that a simple diarrhoea can become a deadly disease for a child in Guinea-Bissau.
How is MSF working in Guinea-Bissau?
To provide efficient and effective care to the child population, we must consider several aspects. First, we are doing intensive work with the community, the families and mothers, to encourage them to trust in the public health system and bring their children to paediatric visits.
We offer free, quality medical services and this is a big change for them.
We also ensure that mothers are taught to identify severe cases in time and take their children to health centres. Then there are the families who live in areas far from health centres.
A very important figure here is the community health agent, who takes medical care to children’s homes. We are training more than 200 community agents who will travel to the areas furthest from the capital, Bafata.
Moreover, we are strengthening technical support to the primary healthcare system, with medical equipment and training for professionals to improve diagnostic capacity and treatment.
We also give specific support at the secondary level, i.e. in the hospital’s paediatric unit, so that the most serious cases can be transferred to the hospital and treated properly. All this while ensuring free care and a functioning referral system.
How has the threat of the Ebola epidemic affected Guinea-Bissau?
During the opening of the project, with the Ebola epidemic devastating several countries in the region, much of our work focused on working together with the country’s technical committee to manage the preparedness and prevention of the epidemic.
The lack of knowledge about Ebola in the region and, above all, the limited capacity of the country’s health system meant that early detection of the first cases would not have been possible. Fortunately, the country has not had any cases of Ebola so far.
What reaction have you received from the local authorities and the population?
The acceptance of MSF by the population and health authorities has been very positive. We are providing free quality healthcare; this is totally new to them and they are reacting very well.
Word has spread quickly in the area where we are working and more and more mothers are bringing their children in for paediatric consultations.
To get an idea of the progress made, only 10 children came for paediatric consultations in Bafata in February 2014, while for the same month in 2015 the number children rose to 100.
Doctors Without Borders (MSF) has worked intermittently in Guinea-Bissau over the past two decades. Since its first appearance in 1998, MSF has carried out several interventions to respond to epidemics of cholera, meningitis and measles, and to serve victims of violence and internally displaced people.
In November 2014, MSF began working in the paediatric unit of the regional hospital of Bafata and in the health centres in Tantan Cossé and Contuboel.
Find out more about MSF's work in Guinea-Bissau.