Between 130,000 and 150,000 Rohingya refugees live in Nayapara camp/makeshift settlement and more than 22,000 in Unchiprang.
The settlements are located south of the largest Rohingya refugee camp, Kutupalong-Balukhali mega-cap, near the southern tip of the Cox’s Bazar peninsula – a narrow strip of land along the Naf river, which divides Bangladesh and Myanmar.
The rapid influx of refugees from August 2017 dramatically increased the need for medical services in this area.
Primary Health Care
MSF runs one primary health centre (PHC) in Nayapara and one in Unchiprang. The PHCs focus on primary healthcare and standard outpatient services.
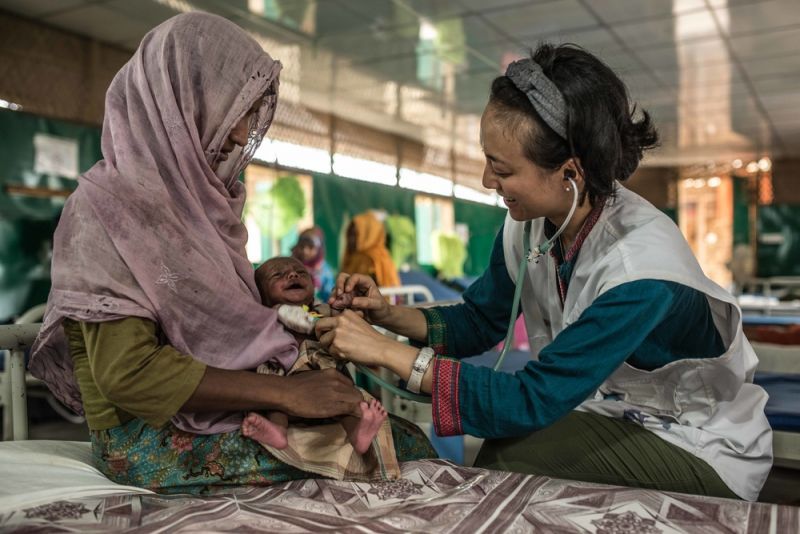
Patients can see a doctor or bring children for vaccinations and wound dressing is provided. Services for women who are pregnant or have recently delivered are available.
Every day, Unchiprang PHC provides around 200 consultations and Nayapara PHC, around 250. Patients come from both the host communities and the refugee camps.
In addition to primary healthcare, the PHCs provide mental health services and medical and psychosocial services for survivors of sexual violence. They also provide 24-hour emergency care, stabilisation and ambulance referral.
24 Hour Emergency Services
In Unchiprang camp, the MSF health centre is the only health facility that provides services around the clock.
“Here in my camp,” said nurse supervisor, Tanjima Chowdhury, “only MSF has 24-hour shift [as well as] regular primary health services. There is no other medical support for 24 hours. No-one.”
Patients come to the health centre at night with emergency or very serious health problems, Chowdhury explains: “They come with severe respiratory distress, in labour, with severe bleeding and sometimes with accidental injuries.”
“The Rohingya refugees don’t actually have an option,” she continues. “They’re not allowed to leave the camp. Only MSF can refer the patient to another facility. If MSF had no 24-hour service, it would be difficult for them.”
Catarina Branco, nursing activity manager at Nayapara health centre, agrees:
“We have the observation room and the emergency room, where we receive cases from the street, the community and the camps… At night, patients come mostly in the evening and in the early morning after the first prayer of the day. We have a lot. Sometimes when we arrive in the morning, we have a full house already.”
Referral
Branco explains that the teams need to identify which patients can be treated at the health centre, where they can be stabilised and observed for up to 24 hours, and which need to be referred:
“For example if we have a surgical case, we will always refer because we don’t have surgical capacity here. But imagine a child who is four years old with respiratory distress who needs nebulization and needs to be observed for a time… we just keep him here with his mother or someone from the family, and we observe and wait till the patient gets better and then send him home.”
Sometimes patients struggle to understand referral. A team of Rohingya volunteer health promoters help to explain.
“Sometimes patients are unable to understand why this is not here, why this is another place,” says Chowdhury, “Sometimes it’s confusing. They help us explain why the referral is needed.”

Continued Activity
More than a year after the current crisis began, both Unchiprang and Nayapara PHCs continue to adapt and expand their activities. Construction has started at the Nayapara PHC on a maternity facility and a new mobile clinic is planned.
Unchiprang PHC will also be expanded to provide more space for the waiting and consultation areas, mental health counselling and health promotion activities.
“We’re always trying to improve our facilities and increasing our activities according to the situation, according to the patient needs,” says Chowdhury
Find out more of MSF's work in Bangladesh.
