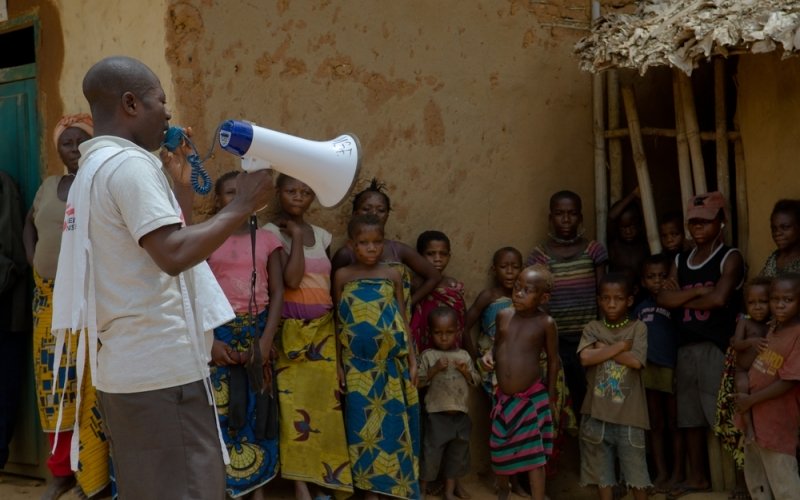In response to high levels of sexual violence in the Ituri region of eastern Democratic Republic of Congo (DRC), Doctors Without Borders (MSF) has launched a project in Mambasa to provide medical and psychological care to survivors.
Driving along the red mud road, the MSF Land Cruiser passes through a cloud of white, yellow, and orange butterflies. On either side of the road is thick forest. The trees are packed so closely together that visibility is limited to a couple of feet.
It is not far from the Okapi Wildlife Reserve, and among the trees are animals on the brink of extinction, elephants, and villages inhabited of pygmy people who are the original inhabitants of this region. The trees also hide gold and diamond mines, both official and unofficial; smugglers of hardwood; poachers; armed Mai-Mai militiamen; and many other men carrying weapons.
The MSF staff in the vehicle represent one of three medical teams circulating between the towns of Mambasa, Nia-Nia, Bella, and PK51. At each stop, they provide care for victims of sexual violence and people suffering from sexually transmitted diseases.
Their work is part of a project launched this past February. They have already been very busy. "In March alone, our teams took care of 123 victims of sexual violence and treated 907 people for sexually transmitted diseases," said Mame Anna Sane, MSF medical team leader.
"These are very big numbers. That is almost four people raped per day—and that is just the ones coming to health facilities. Rape is so taboo that many people don’t come for help, so the real numbers are likely much higher."
Each of the three MSF teams is made up of a nurse, a psychologist, and a health promoter. Together, they provide support to nine health facilities in the region by training local staff members in the provision of medical and psychological care for survivors of sexual violence.
The MSF teams also supply the necessary medicines and work with local communities to raise awareness about sexual violence, encouraging victims to seek medical care promptly. Rape survivors need to come for help within 72 hours of an assault for treatment to be effective. MSF teams also educate people about the symptoms of sexually transmitted infections so that people recognize them and come for treatment.
Taking Care of the Survivors
The work with local communities is showing results, and there is evidence that rape survivors are coming forward more promptly.
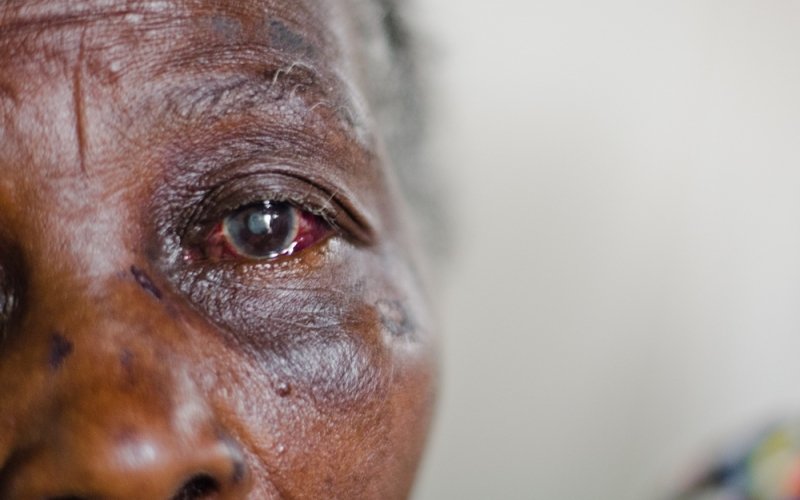
When an MSF team is visiting the Biakato health center, a 70-year-old woman who survived a gang rape is brought in by a group of relatives and neighbors. Two days earlier, she was asleep at home when three armed men broke down her door. They dragged her out of the house and into the forest, where they beat her and then raped her one by one.
They left her in the forest, naked and unconscious. At the health center, she will receive psychological support and treatment for HIV and other sexually transmitted diseases. Her daughter is with her—but not all patients have family members to support them.
Marie, 37, is in the maternity ward at Biakato health center. She has just given birth to a baby boy and she is alone. Almost two years ago, as she went to sell drinks in a mine near her home, Marie was kidnapped by a Mai-Mai group. They kept her prisoner for more than a year and raped her repeatedly.
She only managed to escape when the Congolese army attacked the camp where she was being held. She returned to her husband, but he rejected her because she was four months pregnant from one of the rapes.
A Medical Emergency
"Our work involves changing mentalities to get rid of the taboo around [reporting] sexual violence, and to be able to offer proper care to every victim. [This mean working on] the mentality of the local population, but also of the authorities," Sane said. "Of course there is a criminal and legal aspect to sexual violence, but for us, it’s first of all a medical emergency."
MSF’s project in Mambasa will last six months and then be reassessed. It is already clear, however, that the need for medical and psychological care for survivors of sexual violence in the Ituri region are far greater than expected.