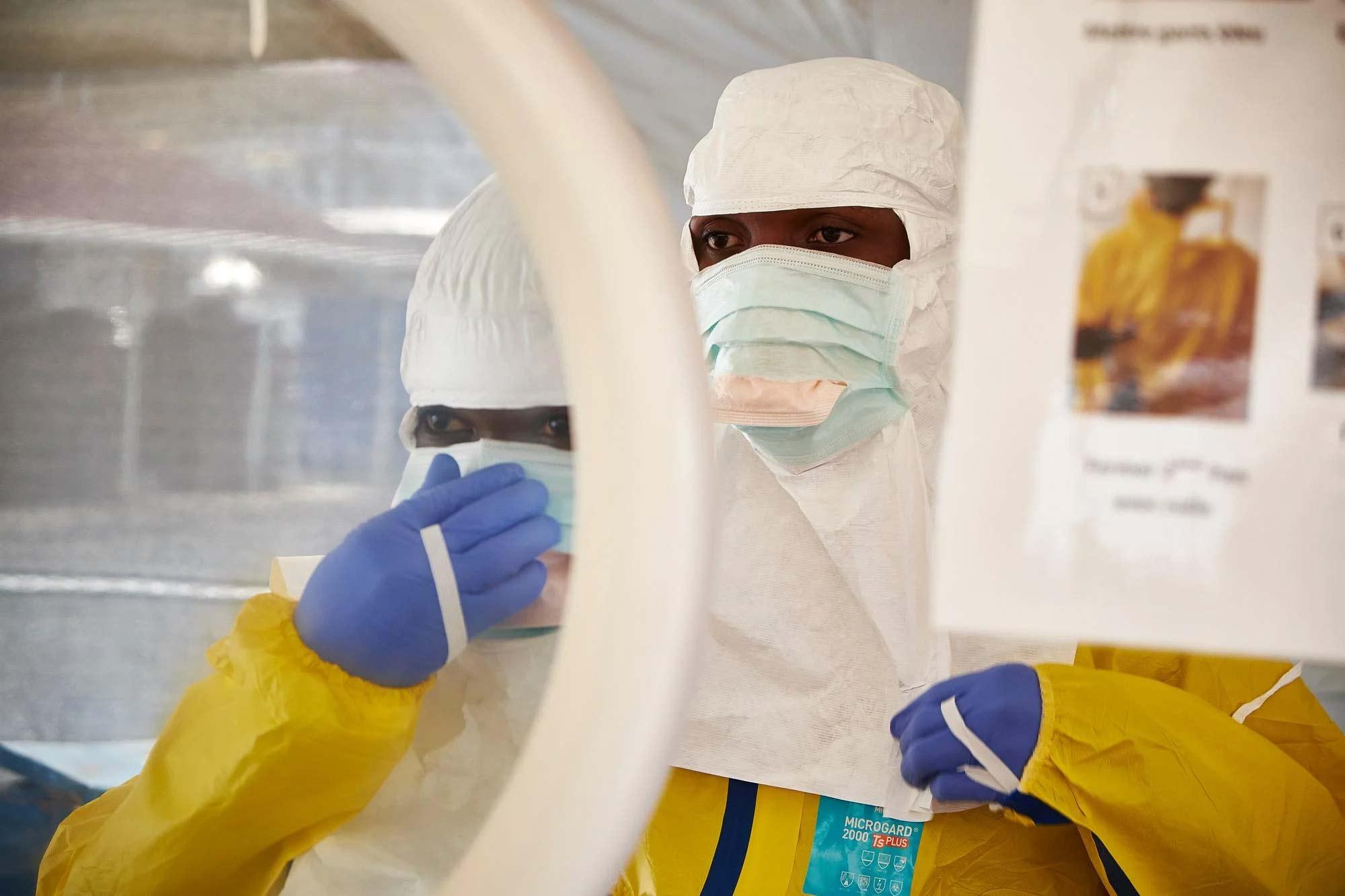
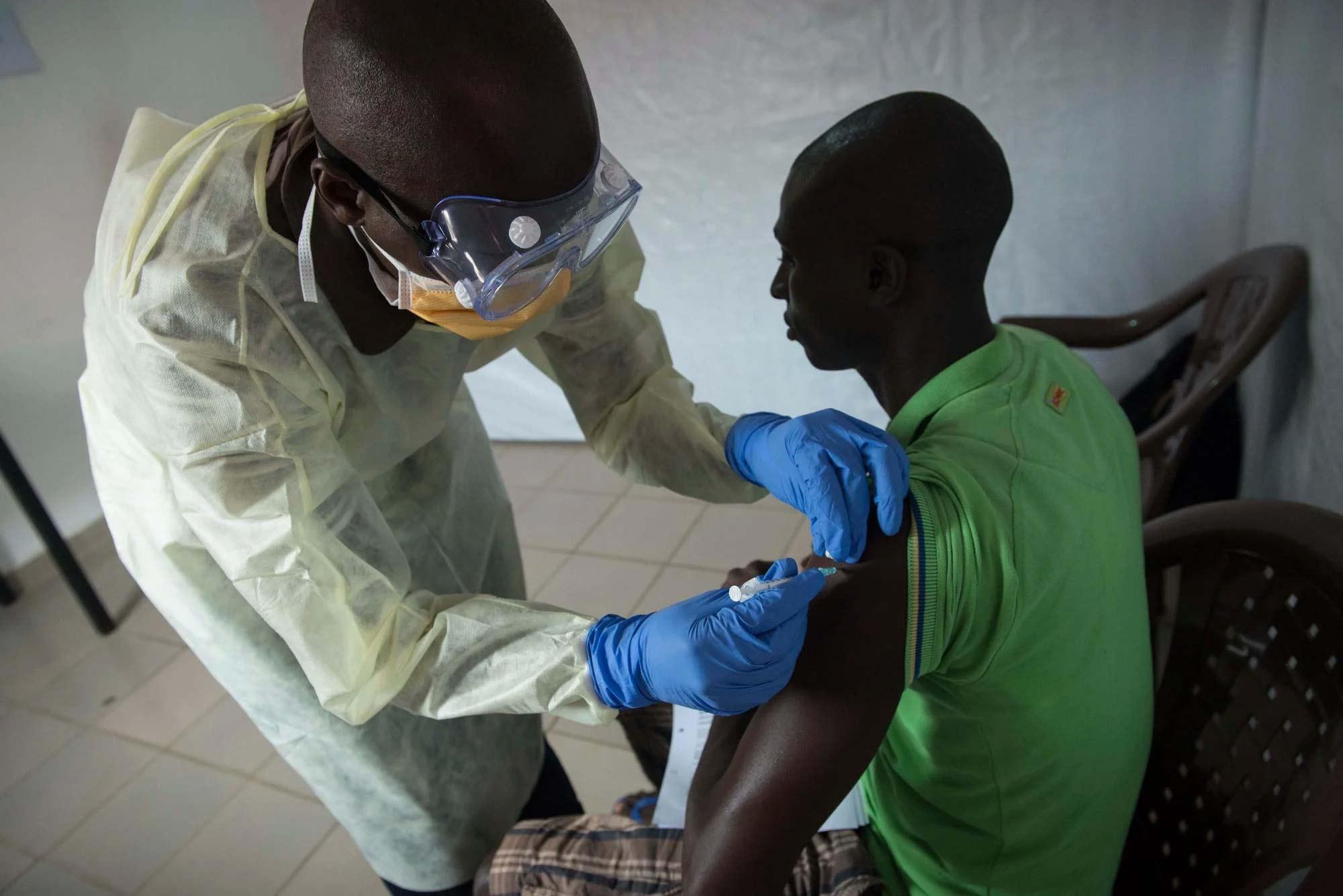
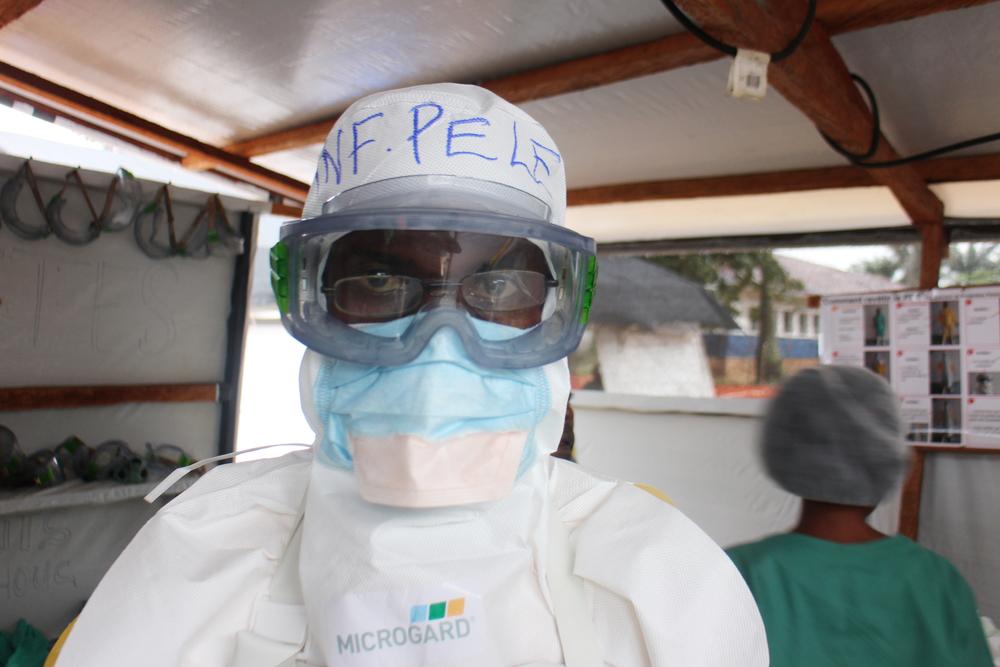
Once a case of Marburg or Ebola is confirmed, a swift response is vital. The needs of patients and affected communities must remain at the heart of the response, which can be defined by six main pillars: care and isolation of patients; tracing and follow-up of patient contacts; raising community awareness of the disease, such as how to prevent it and where to seek care; conducting safe burials; proactively detecting new cases, and supporting existing health structures.