

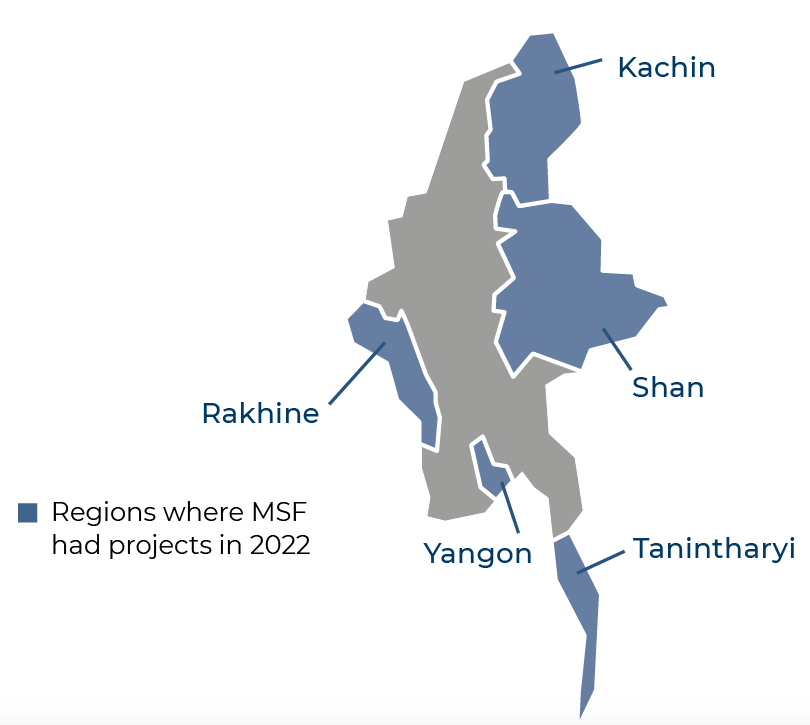
Myanmar
MSF teams continue to care for HIV, tuberculosis and hepatitis C patients, provide basic healthcare and reproductive and sexual healthcare services, and to respond to medical emergencies.
We pioneered HIV treatment in Myanmar – at one point becoming the largest provider of antiretrovirals in the country – and steadily grew a large patient cohort. In 2015, we began working with the Ministry of Health to transfer patients to the decentralised National AIDS Programme, so people can receive care closer to home. This has been suspended since the military seized power, and we are now seeing those patients return to us in greater numbers at our clinics in Shan, Kachin and Tanintharyi.
Despite restrictions on humanitarian access to conflict-affected areas, we have mobile teams based in Sittwe and Maungdaw in Rakhine state, who offer basic healthcare. They also arrange emergency referrals for patients from all communities, including those forcibly detained in camps.
Our Activities in 2022 in Myanmar
Data and information from the International Activity Report 2022.
1,340
1,34
€16.5 M
16.5M
1992
1992
In 2022, public health services continued to deteriorate after thousands of doctors and nurses left their jobs to join the civil disobedience movement. Meanwhile, growing insecurity and administrative barriers hampered humanitarian access, further limiting the availability of healthcare.
In response to the drastic reduction in tuberculosis (TB) services across Myanmar, MSF scaled up activities at Aung San TB hospital in the country’s largest city, Yangon, where 50 per cent of the country’s patients with drug-resistant TB go to receive treatment. As well as providing hands-on care, we helped to detect new cases through community outreach activities.
In mid-2022, we resumed the handover of some of our HIV patients to the Ministry of Health. In 2015, we began working with the ministry to transfer patients to the national AIDS programme. This was postponed when the military seized power in 2021.
In early 2022, as COVID-19 cases declined, we closed the three dedicated centres we had set up in Yangon, Hpakant and Myitkyina.
Following an escalation in conflict in Rakhine state in August, the military imposed restrictions on movements of people and goods, including medications. This meant that we were unable to run our mobile clinics for four months, which further curtailed access to healthcare for people living in vulnerable circumstances. Only emergency referrals were allowed during this period. In December, we resumed services in some locations; however, not at full scale.
In Kachin and Shan states, we responded to people fleeing violence by providing medical assistance and distributing relief items such as hygiene and cooking kits.
IN 2022

190,700
190,7
7,760
7,76
2,470
2,47
33
33


Out of Fear: Rohingya youth trapped in violence and despair

After 10 years in camps in Myanmar, Rohingya mental health continues to suffer
Myanmar: MSF implores all parties to ensure unimpeded access to healthcare

MSF's Yangon office becomes makeshift clinic amid Myanmar's collapsing health system
