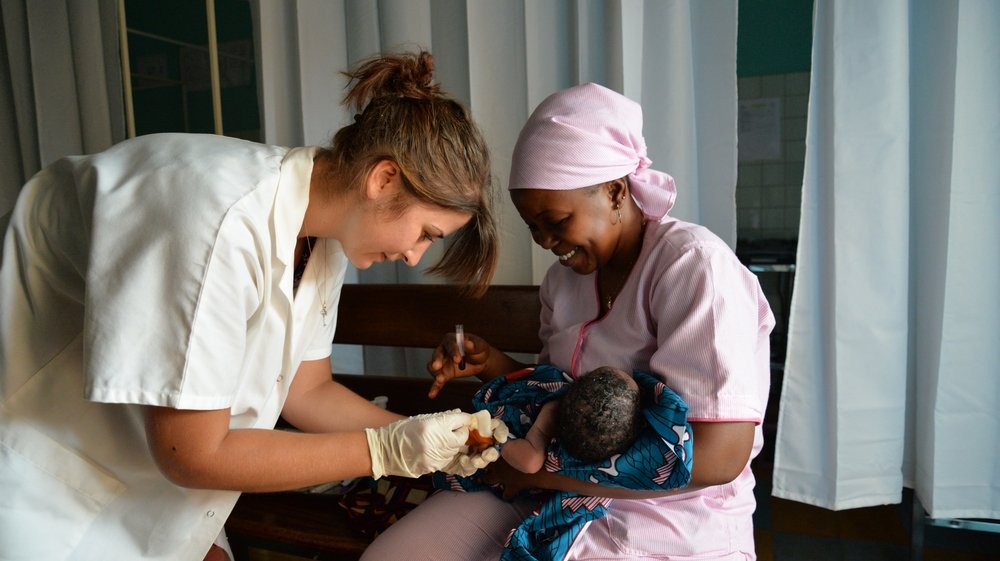
Years of instability have severely undermined Côte d’Ivoire’s health service, which now lacks facilities and trained staff, and the shortage of medical treatment available to expectant mothers and their babies has resulted in particularly high levels of maternal mortality.
In July 2014, Doctors Without Borders (MSF)—already present in maternity units in Duékoué and Abobo—opened a programme of care for pregnant women and new-borns at Katiola Regional Hospital Centre (RHC), north of Bouaké. The programme is run in partnership with Côte d’Ivoire’s Ministry of Health and the Fight against AIDS.
Madeleine and her medical team at Katiola hospital have spent a long and anxious night, but she can relax now. Madeleine was designated a ‘red code’ emergency surgery case because of suspected umbilical cord prolapse, which could have resulted in her baby being asphyxiated.
But, in fact, the cord was wrapped around the baby’s neck. Luckily, the Franco-Ivorian surgical team were able to perform a caesarean section in the brand new operating room re-opened only a few days earlier, at the end of April.
“This region has a really high infant mortality rate. Over 600 women in 100,000 births die, compared to less than 10 in France,” explains Dr Olivier Dro, deputy manager of MSF programmes in Côte d’Ivoire.
“These numbers testify to the lack of obstetric and preventive care and treatment of complications that can occur during pregnancy, delivery and postpartum. While close to 6 deliveries in 10 are assisted by qualified health staff, due to the shortage of medical facilities and an uneven distribution of healthcare personnel, medical assistance is still not only insufficient but also unevenly spread over the country.”
An exemplary cooperation
Nurse and medical coordinator Cécile Brucker spells out the priorities: “To enable women in the region to give birth in complete safety—mothers and babies alike—, we deliver emergency gynaecological, obstetric and neonatal care.
A major renovation programme that included constructing buildings and equipping specialist departments was implemented along with support and training for the hospital’s staff.”
Obstetric and neonatal emergencies can now be treated in the neonatal unit, which will open in July 2015, whereas previously, patients able to afford transport and drugs were referred to the University Hospital in Bouaké.
“We took the time to work with our associates from the Ministry of Health and the Katiola RHC to build a common project that truly addresses mother and child health, which is a public health emergency in the region,” adds Cécile.
Jean-Yves Bailly, the hospital’s administrator, welcomed this cooperation. “We liked MSF’s approach because it was innovative. We participated fully in the decision-making process and our procedures were taken into account.
This project has come at just the right time, as Katiola recently became referral hospital for the Hambol region. It has given us the opportunity to improve still further the quality of our technical platform, from construction and equipment through to staff training.”
A large-scale programme of renovation and training
The programme included completely renovating and re-equipping the operating rooms and sterilisation unit.
The medical test laboratory and blood bank, so essential to responding to surgical emergencies and haemorrhages, have also been refurbished.
“ The rest of the work—upgrading the electrical installation, setting up a system for recycling and hospital-waste treatment, drilling, storage, waste-water treatment and supply—will be finished this summer,” adds Beatrice Wibaux, construction project coordinator.
“The final phase of the construction work and refurbishment involves fitting out the laundry, biomedical logistics/maintenance department, kitchen and visitors’ washing area and renovating the maternity department which will have a neonatal kangaroo care unit and a 20-bed hospital for postpartum mothers.”
Years of crises have undermined the health service, resulting in an uneven distribution of health workers and an aging technical platform.
Muriel Durand, the nurse in charge of training, explains, “In Katiola, staff already have basic training and often some experience working as care assistants, nurses or mid-wives. My role is to refresh certain routine practices, like hygiene, and address essential issues such as early identification of at-risk babies. When there are complications, every minute counts.”
Next step: Providing support to peripheral health centres
The last step after upgrading the technical platform at Katiola hospital was the launch in May of a programme of support for a network of peripheral health centres.
The aim of this programme is to decentralise access to quality medical care for mothers and infants. “Centres will receive support with renovating infrastructure, medical equipment and staff training.
This support is both strategic and complementary to enhancing capacities at the Katiola HRC so as to decentralise access to healthcare and reduce maternal and infant mortality.
Around half of babies continue to be born at home in this region of Côte d’Ivoire and, when there are complications, the distance to health facilities poses a real problem for the health of both mother and baby,” says midwife Cécile Chesneau, who is charge of the “health centres” project.
Key figures
Maternal and infant mortality: a public health emergency in Côte d’Ivoire
Maternal mortality: 614 women in every 100,000 die after giving birth, compared to around 10 in 100,000 in France.
Infant mortality: out of 1,000 births, 68 children do not reach the age of five years, compared to 4 in 1,000 in France.
5 nurses/midwives for 10,000 inhabitants, compared to almost 90 for 10,000 in France.
Source: Ministry of Health and the Fight against AIDS and WHO, 2011
Katiola
An average of 300 births per month during the first three months of 2015.
Approximately 10% were caesarean deliveries.
Find out more about MSF's work in Côte d’Ivoire.