What causes malnutrition?
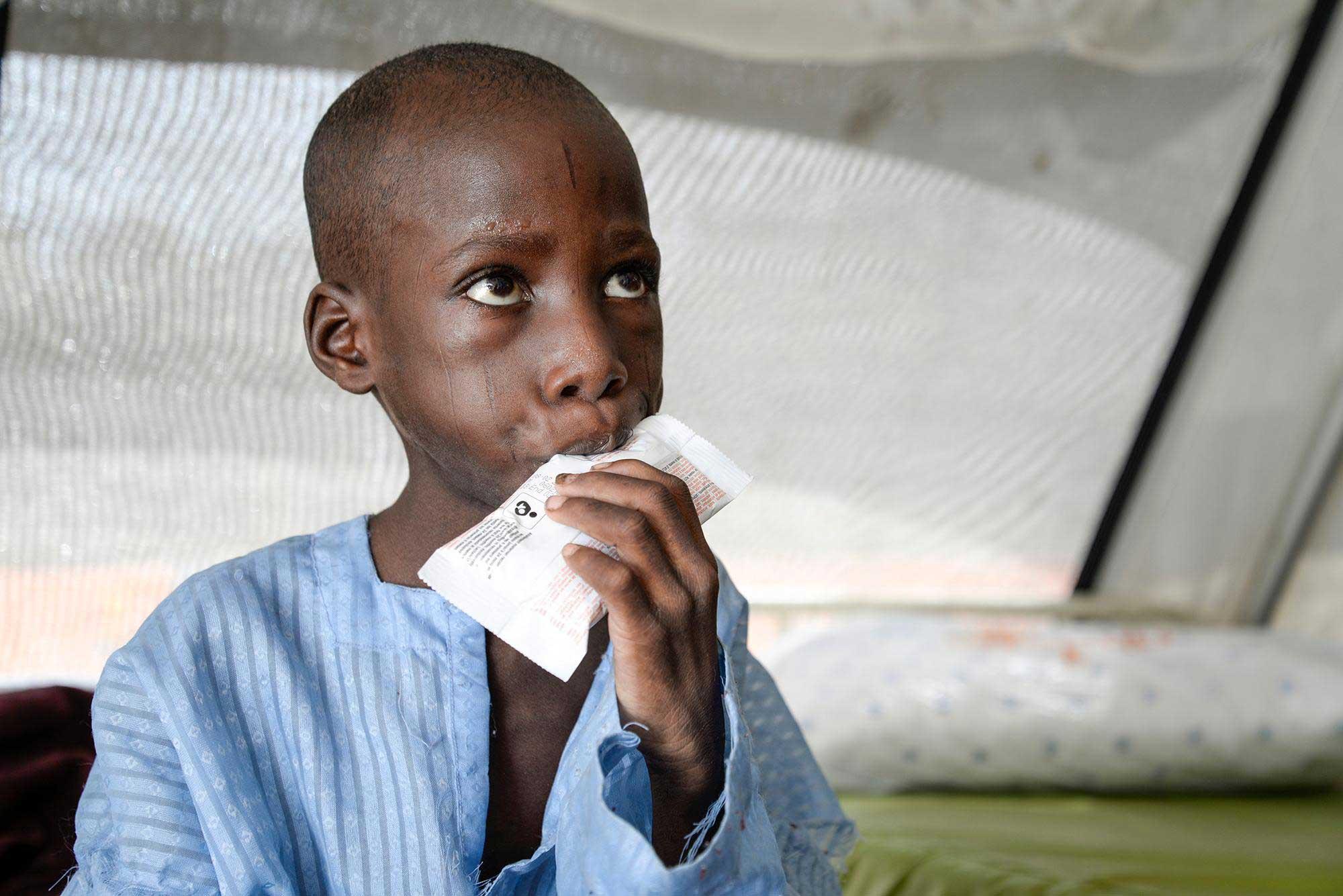
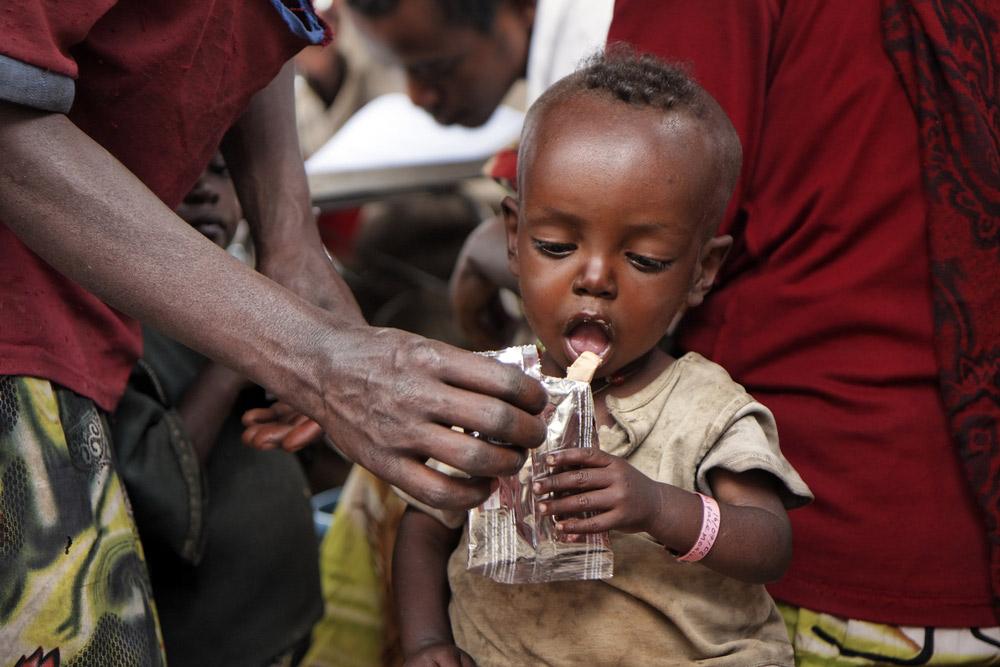
In the first six months of life, breast milk is the only food a child needs—but beyond this point, breastfeeding alone is not sufficient. Diets at this stage must provide the right blend of high-quality protein, essential fats and carbohydrates, vitamins, and minerals. In the Sahel, the Horn of Africa, and parts of South Asia, highly nutritious foods such as milk, meats, and fish are severely lacking.
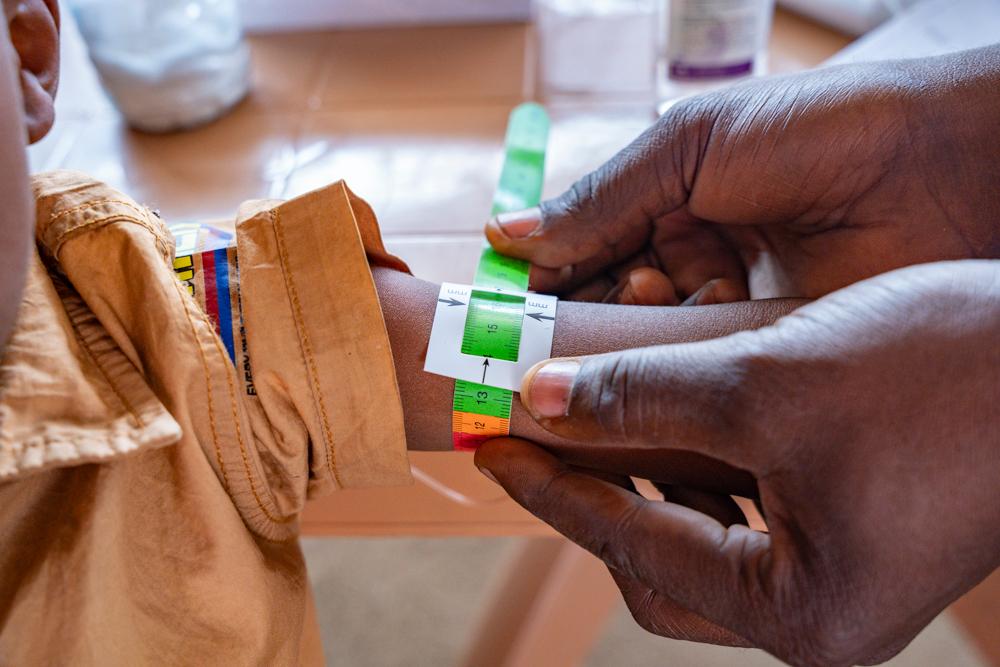
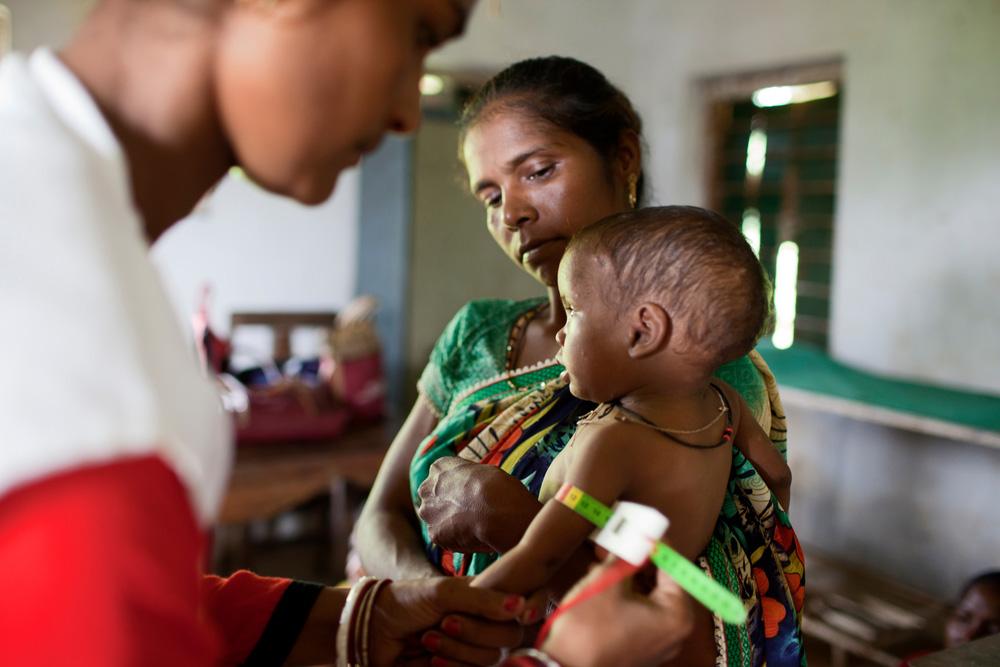
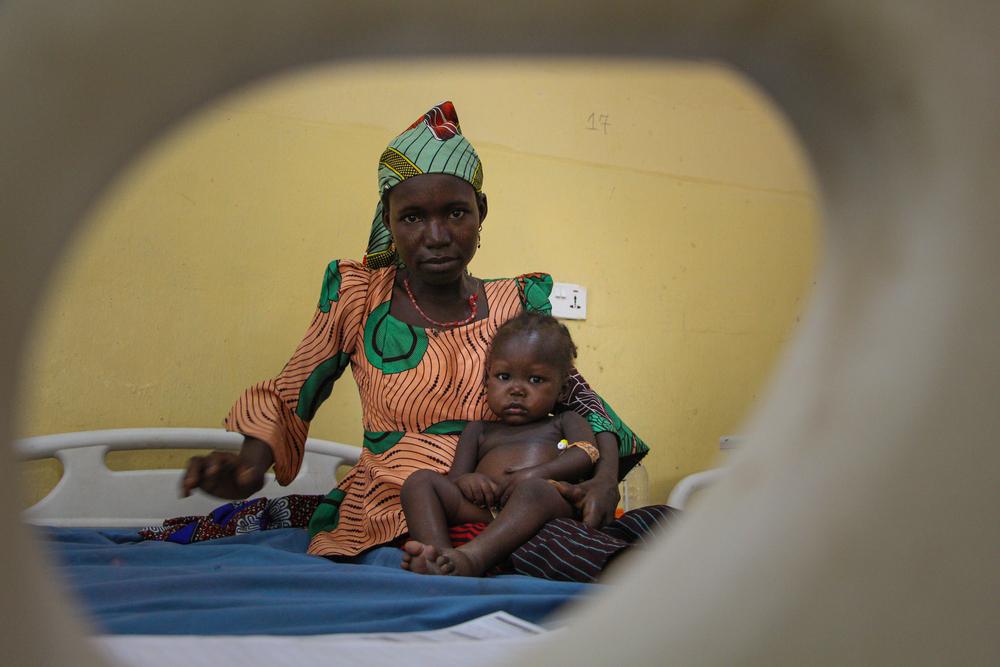
The critical age for malnutrition is from six months—when mothers generally start supplementing breast milk—to 24 months old. However, children under five, adolescents, pregnant or breastfeeding women, the elderly, and the chronically ill are also vulnerable.
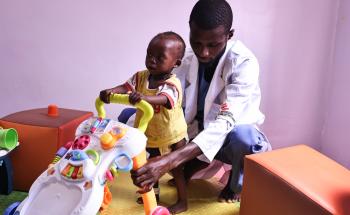
For a child under the age of two, their diet will have a profound impact on their physical and mental development. Malnourished children under the age of five have severely weakened immune systems and are less resistant to common childhood diseases. This is why a common cold or a bout of diarrhea can kill a malnourished child.