Yemen
In 2024, regional armed escalations following Israel’s war on Gaza directly impacted the country. The lack of healthcare in large areas of the country, and the worsening economic landscape had severe repercussions on people’s health and living conditions.
As a consequence of the armed escalations in the Middle East and the Red Sea crisis, key infrastructure, such as Hodeidah port, Sana’a airport, as well as power stations and storage structures vital for delivering much-needed humanitarian aid, had been badly damaged by airstrikes.
Our activities in Yemen in 2024
Data and information from the International Activity Report 2024.
2,334
2,334
€116.1 M
116.1M
1986
1986
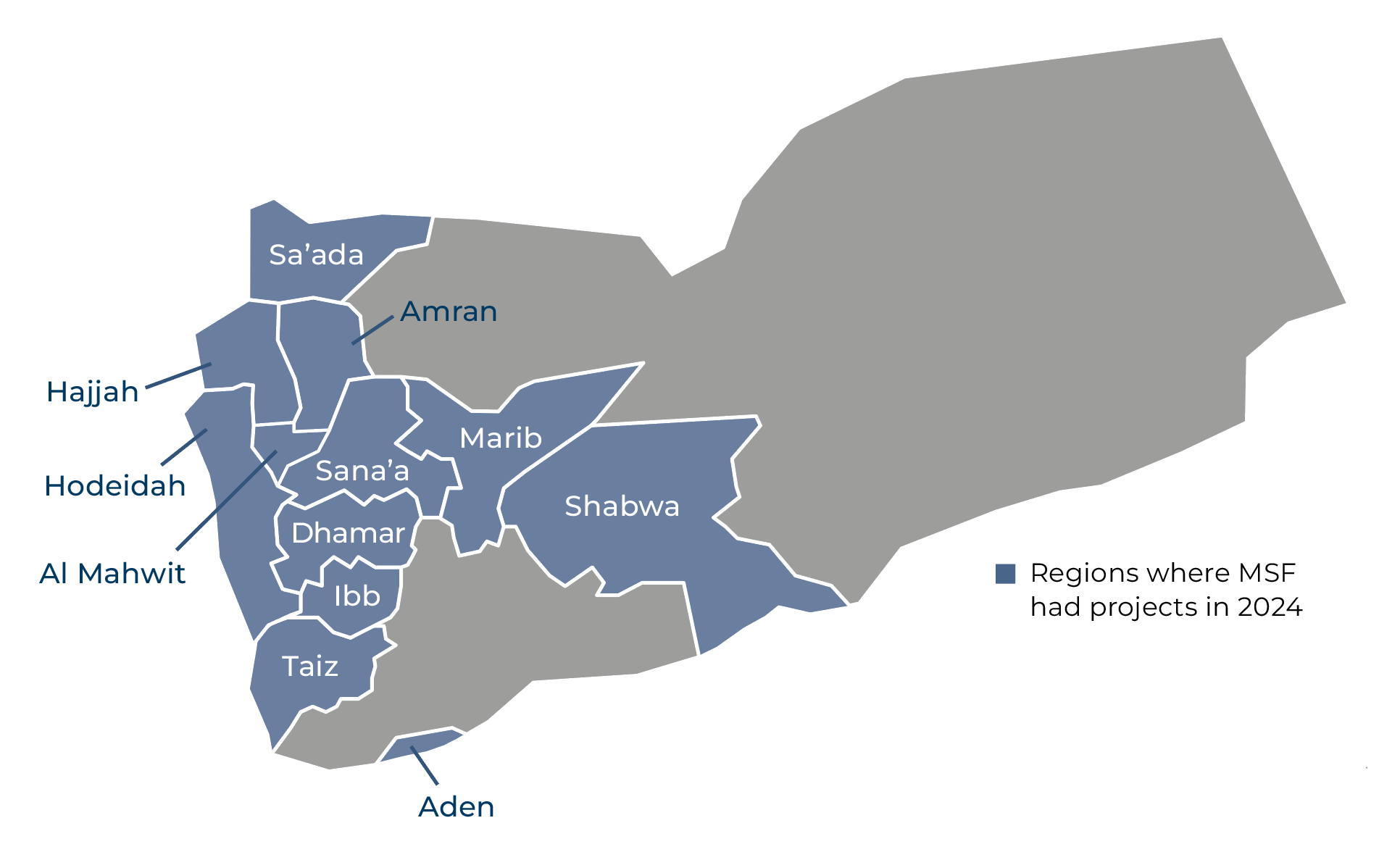
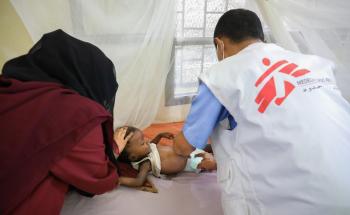
In 2024, MSF worked in 17 hospitals across 12 governorates, providing medical services such as emergency, maternal, and paediatric care, nutrition support, and specialised surgery. To facilitate access to basic healthcare at community level and reduce the strain on hospitals, MSF supported more than 10 basic healthcare centres with staff training and incentives, donations of medications and medical supplies, and rehabilitation works.
In addition, we provided emergency healthcare and donations of blankets and hygiene kits in Mahweet and Marib governorates during flash floods in the second half of the year.
Malnutrition
In recent years, our staff have seen worsening trends in malnutrition, especially among children, as many Yemeni families have lost their sources of livelihood during the last decade of political and economic instability and conflict. To date, the international humanitarian response to the crisis in Yemen has been insufficient to meet people’s immense needs.
In 2024, MSF offered acute and intensive therapeutic nutrition care in seven governorates, both as part of our regular activities, and as stand-alone emergency responses. These included outpatient and inpatient paediatric therapeutic feeding centres in the towns of Ad-Dahi, Az-Zaydiyah, and Al-Qanawes, in Hodeidah; an inpatient therapeutic feeding centre in Abs mother and child hospital, in Hajjah; an inpatient therapeutic feeding centre in Al-Salam hospital in Khamir, Amran governorate; an outpatient therapeutic feeding centre in the Hygiene Fund healthcare centre, in Marib; and Al-Jomhouri hospital and the mother and child hospital in Taiz. In Sa’ada and Amran, MSF maintained a regular contingency plan to start treating malnourished patients in case of a rapid surge in numbers.
Vaccine-preventable diseases
There has been a marked increase in outbreaks of vaccine-preventable diseases in Yemen in recent years, due in part to falling vaccination coverage. As the country’s healthcare system has continued to deteriorate, many people, in particular children, have missed out on routine vaccinations, leaving them vulnerable to diseases such as cholera, acute watery diarrhoea, measles, and diphtheria.
In 2024, MSF launched emergency responses in nine governorates to tackle outbreaks of cholera, acute watery diarrhoea, measles, and diphtheria. As well as treating patients for cholera and acute watery diarrhoea in our regular facilities, in collaboration with the health authorities, we managed or supported treatment units or centres across Aden, Marib, Taiz, Shabwa, Amran, Dhamar, Hodeidah, Hajjah, and Sa’ada. Our teams also responded to outbreaks of measles in Amran, Hajjah, Hodeidah, and Sa’ada, and diphtheria in Dhamar.
In addition, in Marib and Taiz, MSF delivered logistics support to the Ministry of Health for a mass catch-up routine vaccination campaign for children and pregnant women.
Maternal and child healthcare
Maternal and child healthcare continued to be a core element of our activities in Yemen. In 2024, we ran a range of specialised maternal, neonatal, and paediatric services, comprising ante- and postnatal consultations, assistance with deliveries, including caesarean sections, and both inpatient and outpatient care. In Hajjah, MSF supported the maternity, neonatal, and paediatric wards at Abs general hospital. In Taiz, our teams assisted women during deliveries, and provided obstetric surgery, and inpatient neonatal and paediatric care in Taiz Houban and Taiz city. We also supported Mocha general hospital’s inpatient paediatric department.
Since 2022, we have been partnering with Ataq’s mother and child hospital in Shabwa to offer paediatric and maternal healthcare, while in Marib we support maternity services at the Hygiene Fund healthcare centre. In Hodeidah, we ran specialist maternity and neonatal services at Al-Qanawes mother and child hospital. We also provided paediatric and neonatal care for rural communities in Ad-Dahi district, in Hodeidah, and in Dhi As-Sufal, Ibb. In Haydan, Sa’ada governorate, MSF supported the Ministry of Health hospital with vital maternity services, including antenatal care programmes that ensure safe pregnancy and childbirth for mothers, as well as paediatric care, and physiotherapy for malnourished children. In Khamir, Amran governorate, our teams also supported the Ministry of Health with maternity, paediatric, and neonatal care.
In Sana’a, MSF supported the emergency room at Al-Kuwait hospital, and continued to provide treatment for children with visceral leishmaniasis, a neglected disease that is also known as kala azar. In addition, we assisted the central lab in Sana’a, supporting the microbiology department to help identify pathogens that cause infection, especially in neonatal sepsis.
Emergency healthcare and surgery
Our teams provided emergency care at the Aden trauma centre in Aden, as well as at Taiz Houban hospital, in Taiz; Dhi As-Sufal general hospital, in Ibb; Ad-Dahi rural hospital, in Hodeidah; and Abs mother and child hospital, in Hajjah. Since the truce in April 2022, there has been a reduction in fighting inside Yemen, and as a result, fewer war-wounded patients. While this has enabled us to scale down our emergency surgical activities, we continue to run an operating theatre in Al-Qaida general hospital, in Dhi As-Sufal. MSF also donated trauma kits for mass-casualty events to Al-Thawra and Al-Gamhori hospitals in Sana’a governate.
Mental health
Years of conflict, economic hardship, and diminishing access to basic services have taken a severe mental toll on the people of Yemen. In response, we integrated basic mental health care into all our activities in Hodeidah, Marib, and Taiz governorates. In Hajjah, at Abs hospital and our mental health clinic in Hajjah city, our teams provided psychiatric care, individual and group counselling sessions, and psychotherapy. In Hajjah city, we ran a day centre, offering psychological care, and a rehabilitation programme for patients with chronic mental health conditions.
IN 2024

476,600
476,6
100,400
100,4
232,800
232,8

65,600
65,6
38,700
38,7
17,200
17,2
11,500
11,5

11,400
11,4
6,100
6,1


A Lifeline for Mothers-to-be on Yemen’s West Coast

Combating Antibiotic Resistant Bacteria in Low Income Countries
Grave health crisis as measles cases surge in Yemen

Delivering twins in Yemen’s Taiz Houban hospital