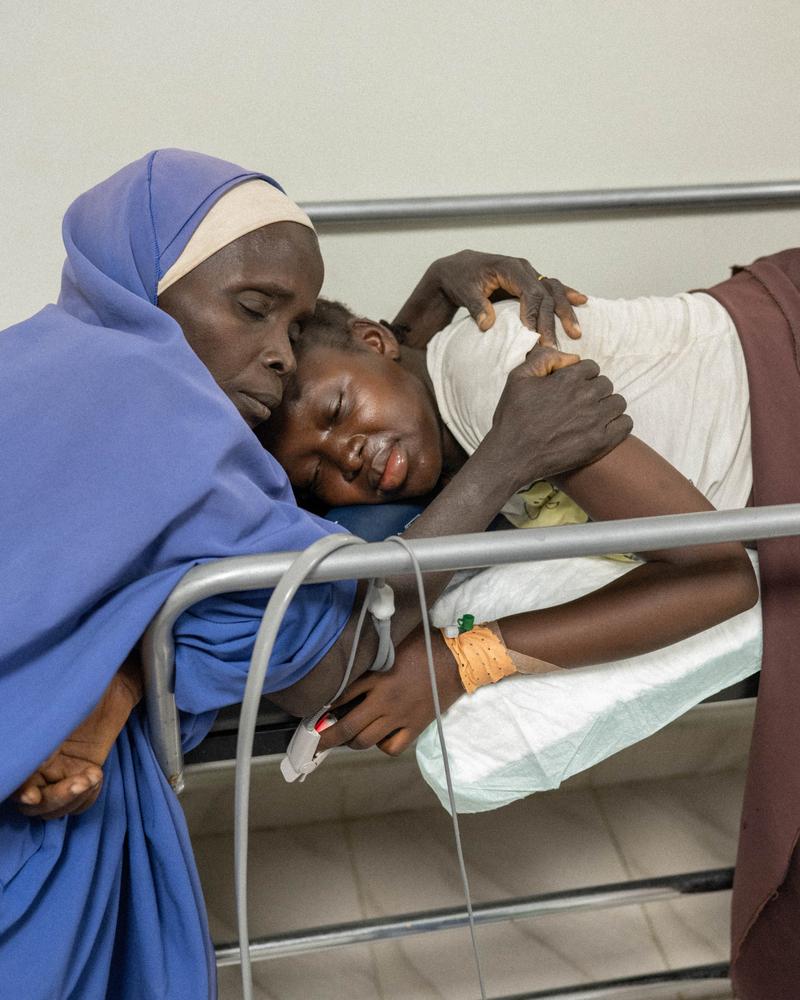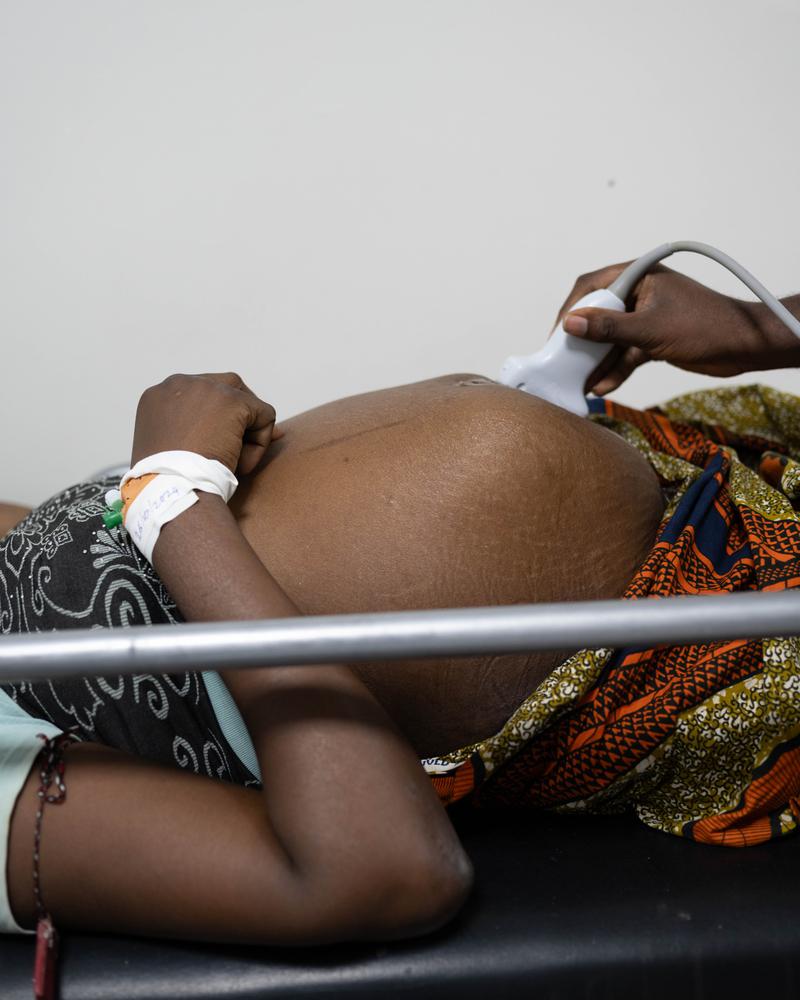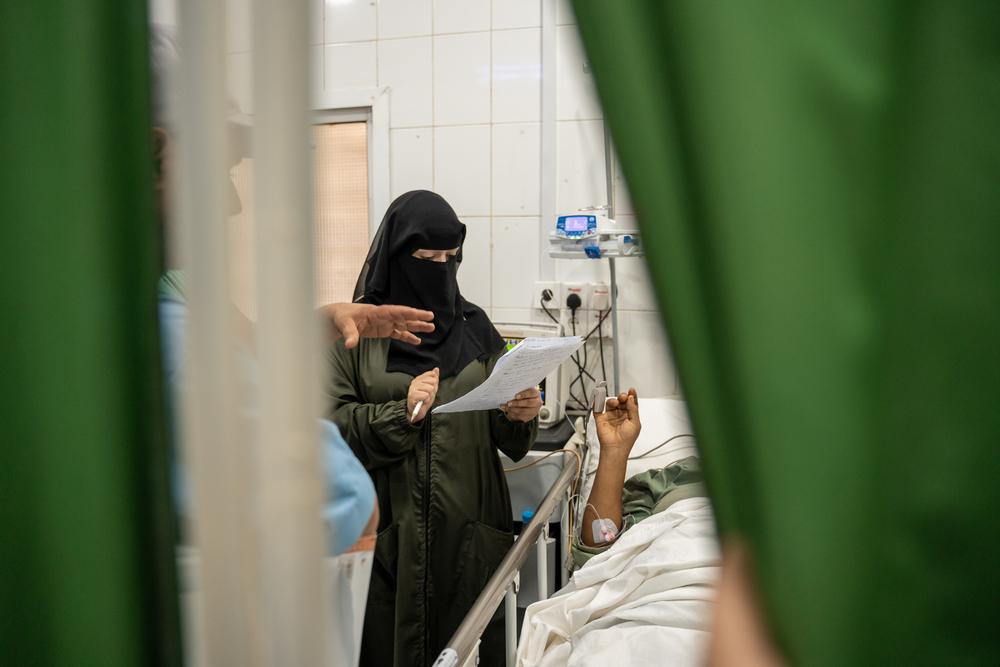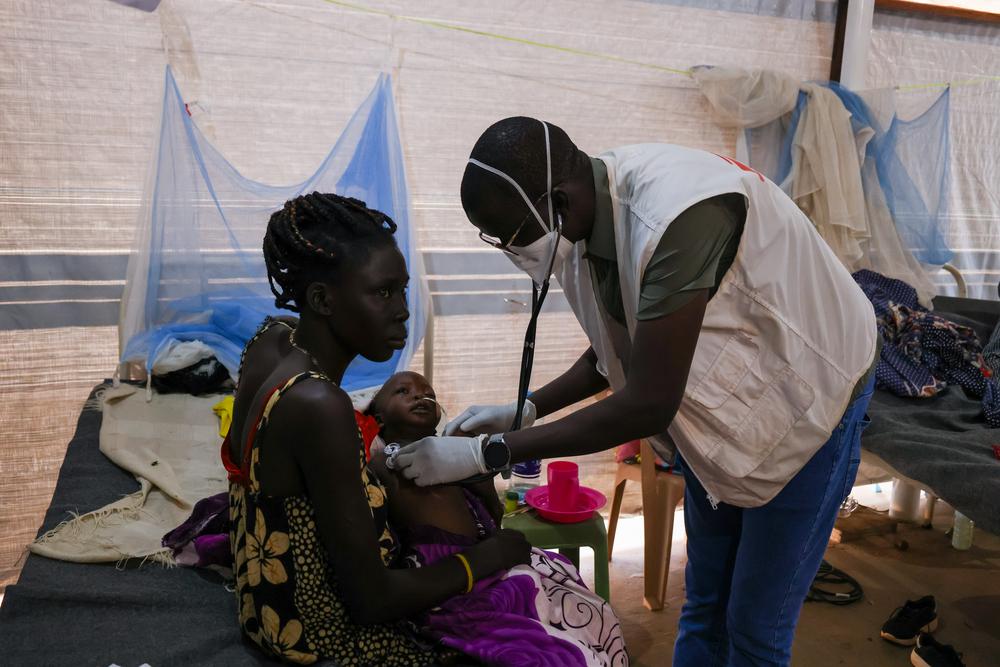
Hemorrhage, or excessive bleeding, can happen after a complicated birth. Often it results from failure of the uterus to contract after delivery. Normally, these contractions stop the bleeding that occurs once the placenta separates from the uterine wall. But complications or incomplete placental separation can lead to continued bleeding, and without rapid medical intervention, a woman can quickly bleed to death.
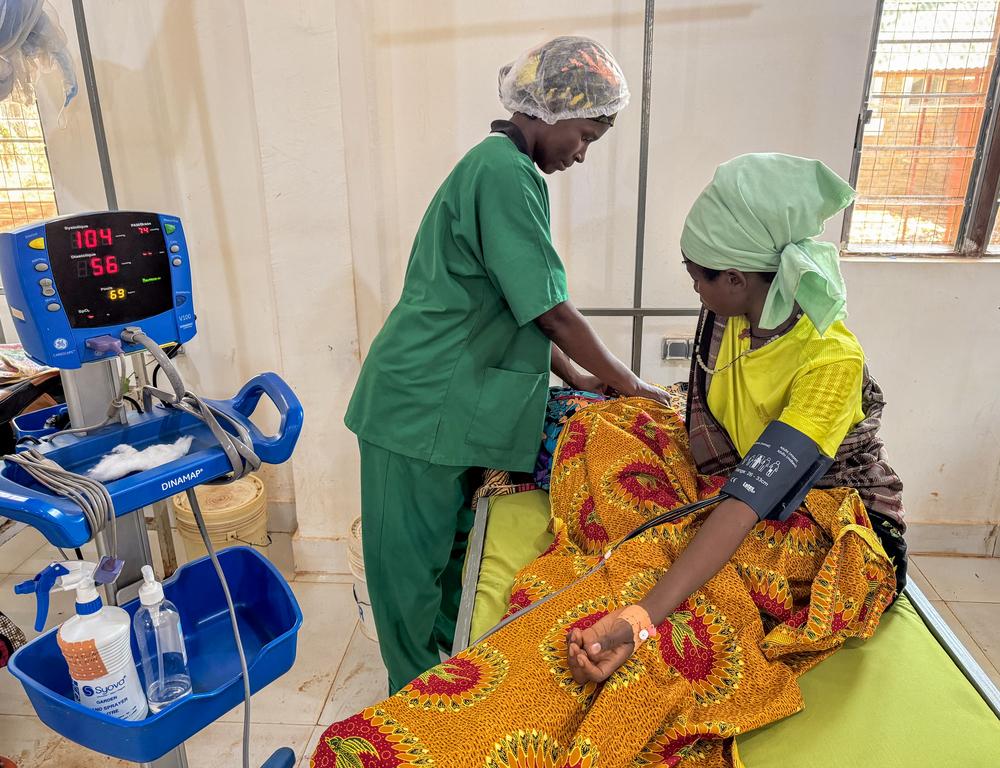
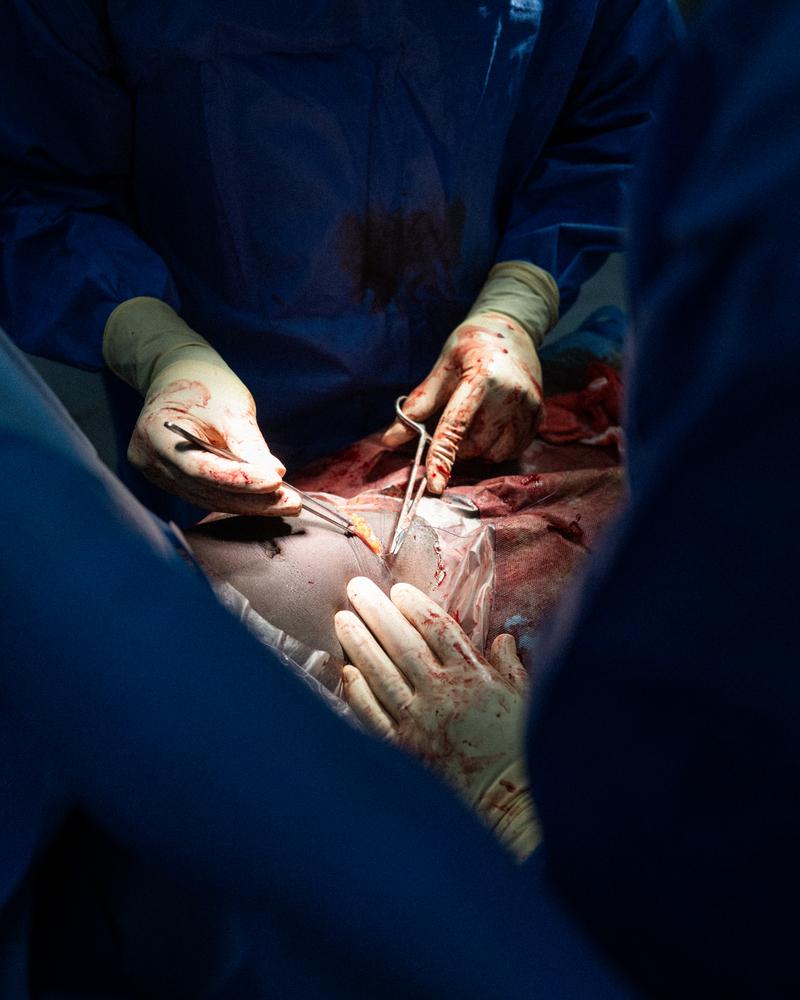
When skilled birth attendants are present, oxytocin can be given to prevent bleeding. If severe bleeding does occur, the mother is resuscitated and attendants apply methods ranging from further medication and manual pressure to stop the bleeding through to emergency surgery.