
Mental health in MSF
Mental Health in our projects
For decades, Doctors Without Borders/MSF teams have provided comprehensive mental health care support to people around the world. From psychological first aid in an emergency setting, to mental health services alongside care for pre-existing conditions, to standalone psychosocial and psychiatric care, here are some of the ways our teams are responding.
This year our teams on the are ground witnessing a dramatic deterioration in the mental health in the project where we work. Here's how they respond to mental health in the projects where we work.
South Africa
msf.org.zaIn our Tshwane Migrant Project, which supports migrants and asylum seekers to access primary healthcare, mental health services and social work assistance our teams have seen how mental health needs have increased in the communities we serve during COVID-19. For our mental healthcare teams, COVID-19 might have affected the way they work but not the work itself. Since the onset of the pandemic, our teams across South Africa have had to adapt how they treat and serve patients. Technology has had to fill in several gaps where face-to-face contact is not possible in order to avoid increasing risk for those we assist.

Kenya
msf.org.zaMSF is witnessing a dramatic deterioration in the mental health of camp residents in Dagahaley, Kenya. The number of attempted suicides is rising, and psychosocial consultations have jumped by more than 50% from last year, over the same time period until September – from 505 to 766. In the last two months, five people have reportedly attempted suicide in the camp, two with fatal results.
“COVID-19 has ended what little chance refugees had of escaping their degrading lives in the camps, compounding the mental distress for many who had nothing left but hope to cling to,” says MSF project coordinator for Dadaab, Jeroen Matthys. “We are seeing a groundswell of desperation in the camp.”

Central African Republic
msf.org.zaOlga, MSF mental health counsellor, facilitates discussion groups at Bossangoa hospital, helping people through stress management, family planning and coping with bad and sad thoughts. “Most of the participants are women: they come to the groups to talk about their conditions... Many of them come from very far away, and they have left their other children at home. They’re worried, and with no vision for their future. Many of them are victims of domestic violence, but they don’t dare to talk about it within their community. Nobody asks these women how they feel, and what would make them feel better."

Greece
blogs.msf.orgSince March 2020, thousands of migrants and asylum seekers have been locked down in overcrowded camps on the Greek islands due to restrictions imposed by COVID-19. MSF has warned about the precarious and inhumane conditions on Lesvos for years. In September 2020, a fire in Moria forced more than 12,000 people to be evacuated from the camp, interrupting medical services available for the refugees and asylum seekers, including services at the MSF paediatric clinic.

Lebanon
msf.org.zaNearly two thirds of patients consulting with MSF’s mental health team in Beirut are showing symptoms related to anxiety and depression. More than half of them attribute their symptoms to the explosion that took place on 4 August. For others with pre-existing mental health issues, 82 per cent admit their symptoms increased in severity after the explosion.
“Two months after the blast, we are seeing an increase in number of consultations. Even though many people have by now treated their physical wounds, secured their external environment and basic needs – like housing, electricity, water – many still cry at night, or they are startled by any slight sound, like that of a pen dropping. They can feel that something isn’t right,” says Rima Makki, MSF’s mental health manager in Beirut.


Mental Health in Africa
While the global needs for mental health care are gradually becoming more visible, such needs remain inadequately addressed in Africa, especially among youth. Africa has the youngest population in the world and the highest level of youth displacement, often linked to man-made crises
Mental Health in AfricaBrazil
msf.orgLast year, in response to large numbers of children and adolescents fleeing the crisis in Venezuela and crossing the border into Brazil, MSF’s mental health team in Roraima identified three pillars of care: identity and self-esteem; inclusion and belonging; protection and prevention against abuse.

Belarus
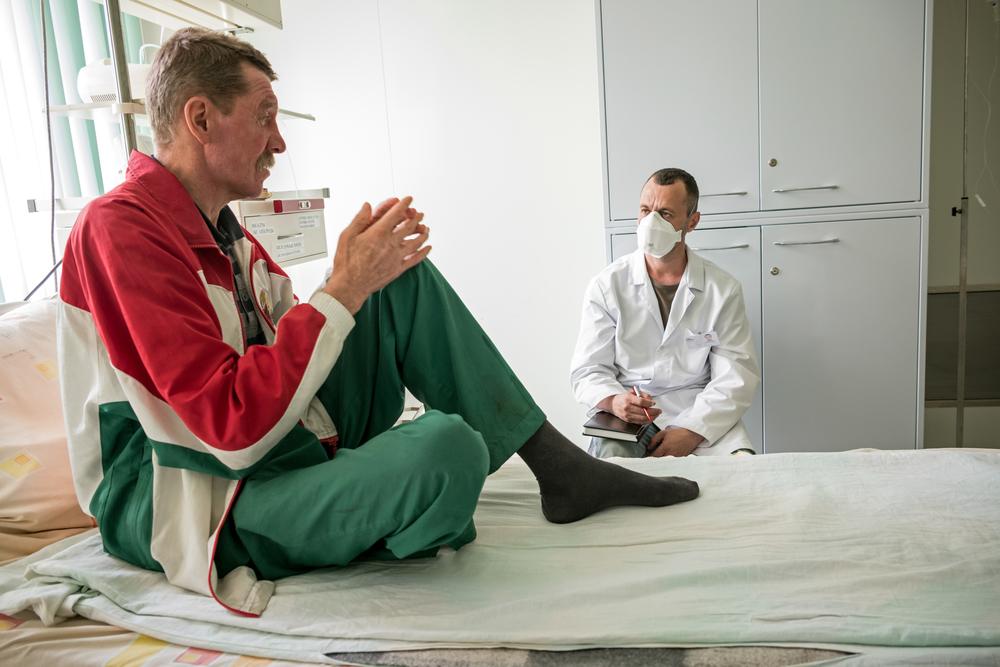
msf.orgMental healthcare is often provided as part of ongoing care for other medical issues. In Belarus, where there is a high burden of multi-drug resistant tuberculosis, MSF teams provide support in four tuberculosis facilities in Minsk. Together with the Ministry of Health, MSF provides a harm-reduction program helping patients with drug-resistant tuberculosis and alcohol-use problems to manage their dependency on alcohol and other substances in order to finish their treatment successfully
Honduras
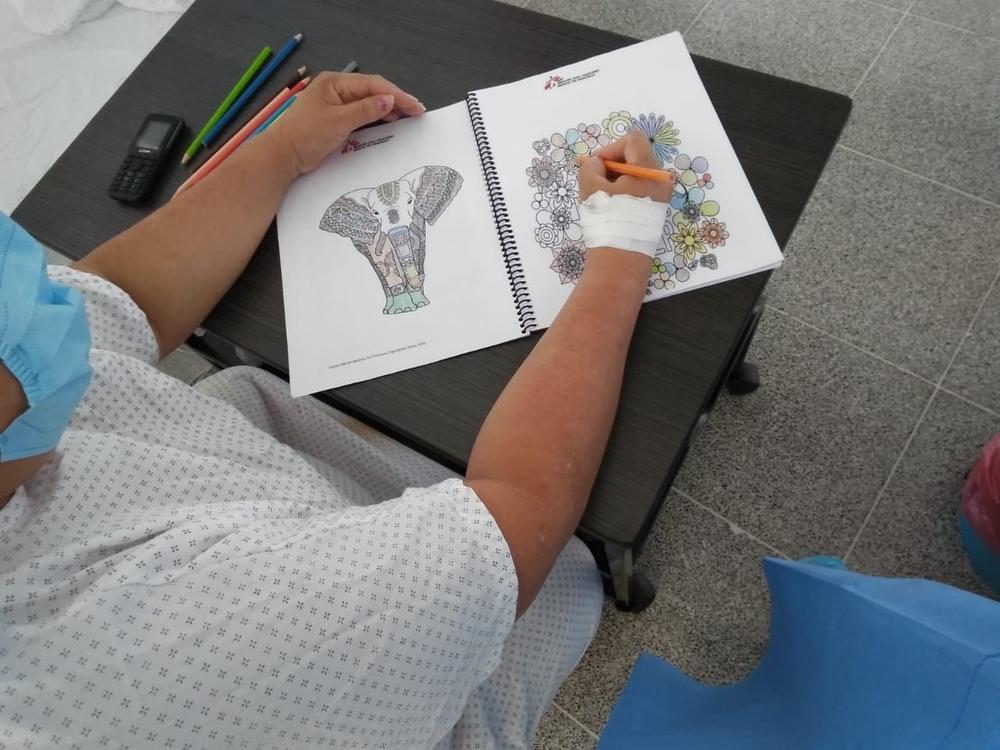
msf.orgIn June 2020, to help keep the hospitals from being overwhelmed, MSF started providing care for patients with mild to severe COVID-19 symptoms at the Autonomous University of Honduras. The health centre supports the Tegucigalpa hospital system by providing comprehensive medical care for patients and their families.
Psychologists and health promoters provide patients with an activity book upon admission, in which they can draw, paint, and read, as a tool for recreational activity and for mental healthcare. This activity goes hand in hand with psychological care, which is carried out by phone and in person.
Mexico
msf.orgMSF’s Centre for Integral Action, known by its Spanish acronym El CAI, provides care for migrants living in Mexico City, who have suffered from torture and other forms of extreme violence. The centre offers long-term care including psychological and psychiatric treatment and social services – including support with applying for asylum, education and job-training services. On average patients stay with the program for up to four months before they are ready to start the next chapter in their lives. Pictured here, a child at El CAI participates in a piñata-making activity during a psycho-social session in November 2019.
