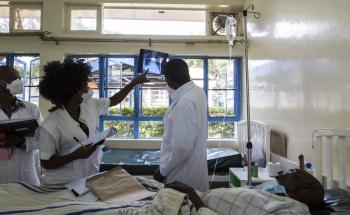
Research findings indicate that many women and girls cannot access the contraceptives that they need, which places their sexual and reproductive health in jeopardy
At the close of Women’s Month 2022, the Stop Stockouts Project* (SSP) releases its latest survey results on medicine stockouts at public health clinics across South Africa, which demonstrate that medicine stockouts most acutely impact women and girls. Key findings show that while there are generally fewer stockouts at facilities, contraceptives now represent the biggest share of medicine stockouts in the public health system.
The survey, undertaken in April 2022 in collaboration with the Ritshidze project**, indicates that stockouts of contraceptives represented 40% of all medicine stockouts reported. Adopting a progressive new survey methodology that puts patient experiences alongside data collected from health facility staff and official figures, the survey indicates that while medicine stockouts have declined in comparison to previous SSP surveys conducted in 2013-2015 and 2017, stockouts continue to form a barrier to women's sexual and reproductive health rights.
During the period April to June 2022, Ritshidze clinic monitors surveyed 15 750 public healthcare users and public healthcare providers of over 400 facilities and found that injectable contraceptives and oral birth control pills were most commonly out of stock at 76.3% and 19.4%, respectively. The research also indicates that other commonly reported medicines stockouts include HIV medication (16% of reported stockouts) and pregnancy tests (10% of reported stockouts). Facilities monitored were located in seven of the country’s nine provinces (excluding the Northern and Western Cape provinces).***
The impacts of contraceptive stockouts fall exclusively and negatively on women and girls. “With endemic violence against women in South Africa, failure to meet our reproductive health needs is another stressor as women without access to contraception are forced into a position of negotiating condom use, or risk an unplanned pregnancy. For some of the most vulnerable women in our country, this lack of access can be catastrophic,” says Dr Indira Govender of the Rural Doctors Association of South Africa (RUDASA).
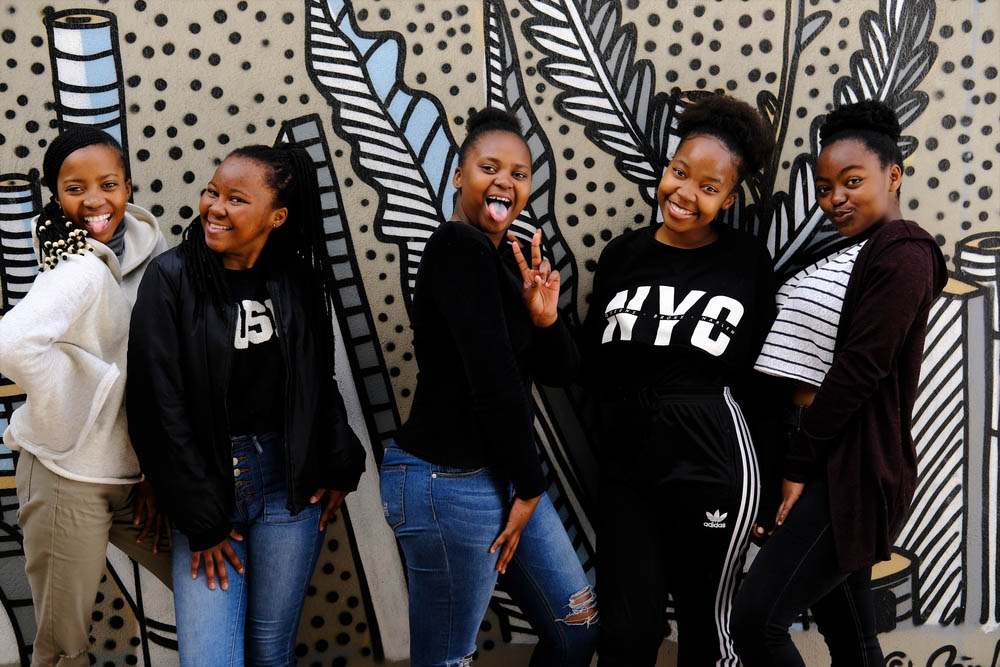
Survey results also indicate that healthcare workers do their best to ensure patients do not leave empty-handed. Of the healthcare workers surveyed who saw contraceptive stockouts for their patients, 58.3% recommended switching to an alternative. However, this is not a sustainable solution and can have detrimental effects on the lives of women and girls through side effects like hormonal changes, as well as the inconvenience of making such significant and sometimes risky changes to their lives.
“Women who take contraception have made a choice not to get pregnant. When supplies are not there, we take away their agency. It’s often risky to change from a long-acting method to a daily method, and it can be costly and time-consuming to women and girls to ensure future continuous access”, says Lucy O’Connell, a nurse and advisor at the Southern Africa Medical Unit of Doctors without Borders.
SSP has shared the full survey report findings with the National and Provincial Departments of health. Among other things, we urge the government to develop a plan that addresses stockouts at public healthcare facilities so that women and girls can access their preferred contraceptives, and develop guidelines for managing the impact of contraceptive stockouts for facilities.
Women who take contraception have made a choice not to get pregnant. When supplies are not there, we take away their agency.Lucy O’Connell, nurse and advisor at the Southern Africa Medical Unit of MSF
Health officials have not responded to our requests for comment on the report, but SSP remains committed to ensuring that recommendations are taken forward by working with health authorities.
SSP acknowledges the significant efforts of the National and Provincial Departments of Health in addressing stockouts of all medicines, which is reflected in the data collected in this survey. However, it is clear that there are important supply concerns for contraceptives, particularly injectables, which are often the required contraceptive of choice for women and girls in South Africa.
SSP, therefore, calls on the Department of Health to urgently address these issues in order to ensure that women and girls can always access their preferred contraceptive at any public health facility. “Failure to prioritise access to contraceptives for all who wish to access them is a failure by the government to prioritise the lives of women and girls across the country. The Stop Stockouts Project urges rapid action and response from the government to urgently address this issue,” says SECTION27 legal researcher Baone Twala.

“Women and girls are bearing the burden of the unavailability of contraceptives in South Africa, despite a clear constitutional right to access to healthcare services, including reproductive healthcare services. Inability to access contraceptives when needed can lead to unwanted pregnancies, which in turn can direct impact their physical and mental health, financial security, and ability to continue education or working,” concludes Twala.
*More about Stop Stockouts Project
Established in 2013, the Stop Stockouts Project is a consortium of five civil society organisations Doctors Without Borders (MSF), Rural Doctors Association of South Africa (RuDASA), Rural Health Advocacy Project (RHAP), SECTION27, and the Treatment Action Campaign (TAC) that aims to monitor and report on medicine and vaccine shortages and stockouts at primary healthcare facilities.
** More about the Ritshidze project
Ritshidze is a project being implemented by organisations representing people living with HIV—including the Treatment Action Campaign (TAC), the National Association of People Living with HIV (NAPWA), Positive Action Campaign, Positive Women’s Network (PWN) and the South African Network of Religious Leaders Living with and affected by HIV/AIDS (SANERELA+)—in alliance with Health Global Access Project (Health GAP), the Foundation for AIDS Research (amfAR), and Georgetown University’s O’Neill Institute for National and Global Health Law. Ritshidze works towards improving the quality of HIV and TB services provided in the public health sector through a community-led clinic monitoring system which is being rolled out in hundreds of primary healthcare facilities across the country.
*** The Northern Cape and Western Cape provinces were not surveyed because monitoring focuses on high-volume PEPFAR-supported clinics (which do not exist in the Northern Cape) and relies on authorisation for monitoring from each province (which the Western Cape has declined to provide).