MSF is no substitute for a functioning health system and calls on the Eastern Cape health department to urgently address leadership and medical staff gaps to avert unnecessary deaths, system collapse in future COVID-19 waves.
To prevent system collapse in Livingstone Hospital as the number of people infected with COVID-19 continue to rise in the Eastern Cape’s Nelson Mandela Bay Municipality, we are calling on the hospital’s senior leadership team to ensure that sufficient doctors and nurses are made available to staff the hospital’s primary COVID-19 ward, which our MSF team has supported since 29 June, on a sustained basis.
We have supported the Eastern Cape Department of Health (DoH) in all three COVID-19 waves, and during the second and third wave our teams worked in Livingstone Hospital, specifically in the basement COVID-19 ward – a hospital car park turned into COVID-19 centre.
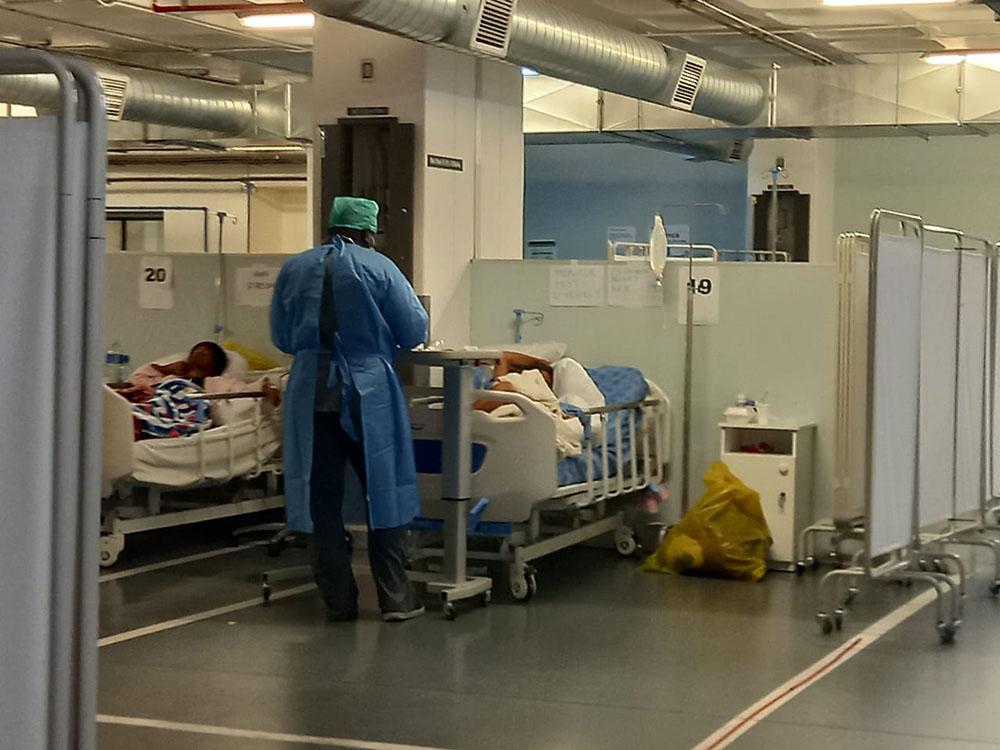
“A team of MSF doctors and nurses will continue to support in the basement ward in September, but this support has to be supplementary. It is not sustainable for the hospital to continue to rely on external support to the extent that it has. MSF acknowledges the rostering of DoH doctors for this ward from 30 August – this will go some way towards ensuring that more beds can be used in the basement ward, taking pressure off other parts of the hospital,” says Brett Sandler, MSF Emergency Coordinator.
The 70-bed basement ward is equipped with piped oxygen, and when sufficiently staffed it is able to receive most of the hospital’s COVID-19 cases. However, two doctors made available to the ward by the DoH both left for posts elsewhere in July, leaving MSF doctors working at the peak of the third wave alongside a courageous but overstretched team of DoH nurses, consultants, physiotherapists and nutritionists.
Given the extreme staff shortages, admissions to the basement ward have been limited to less than 60 per cent of capacity (30 – 40 beds) in order to ensure adequate patient care.
“In this wave of infections, patients we thought would make it simply have not. I don't think there is much more we can do, clinically. I think the bottom line is that when it comes to COVID-19 there is simply no magic bullet. The vaccine is the best tool we have."Dr Rosie Burton, senior MSF clinician
“Because all the beds in the basement ward cannot be used, patients are now backed up in the emergency department or referred to other wards, not all of which have optimal care for COVID-19 patients or access to high levels of oxygen, which is essential for patients severely ill with COVID-19 pneumonia,” says Dr Rosie Burton, senior MSF clinician.
The current wait time for a bed in the basement ward is between 24 – 72 hours.
"With COVID-19 you simply cannot play catch up, and often deteriorating patients are getting to us too late," Burton says.
The third wave of COVID-19 in Nelson Mandela Bay has been protracted. Hospital admissions have continued rising for a longer period compared to previous waves.
Most of the patients seen in the basement ward are critically ill and often include people in their 40s and even 30s, sometimes with the admission of more than one member of the same family at the same time. Despite their best efforts, the MSF team reports that mortality rates in the basement ward have been high.

Tackling COVID-19's third wave in Livingstone's basement hospital
“Vaccination coverage rates in communities must radically improve if we want to avoid going through the same ordeal again in late 2021."Brett Sandler, MSF Emergency Coordinator
“In this wave of infections, patients we thought would make it simply have not. I don't think there is much more we can do, clinically. I think the bottom line is that when it comes to COVID-19 there is simply no magic bullet. The vaccine is the best tool we have,” Burton says
A growing number of hospital high care units across South Africa have reported that very few vaccinated patients developed severe COVID-19 pneumonia in the third wave.
“Vaccination coverage rates in communities must radically improve if we want to avoid going through the same ordeal again in late 2021. In the meantime, the issue of senior leadership in Livingstone Hospital needs to be addressed urgently since it hampers life-saving progress. A permanent CEO needs to be appointed, and adequate staff should be rostered to work in the COVID-19 wards,” Sandler urged.
“A fourth COVID-19 wave is coming, and emergency preparations for this surge should be prioritised in all public hospitals as soon as possible. Plans should be activated in-between waves and not when admissions begin to rise.”