This World TB Day, the World Health Organization (WHO) is recommending for the first time that children with TB and drug-resistant forms of TB (DR-TB) should be cared for in their communities - ground-breaking new guidance that is partly informed by a programme developed by Doctors Without Borders (MSF) and partners in Khayelitsha.
According to the WHO, "A systematic review was conducted to assess evidence on the impact of decentralised and family-centred, integrated approaches on case detection and the provision of TB preventive treatment (TPT). The evidence showed that combined health facility and community approaches increased the number of children and adolescents diagnosed with TB, and decentralised services can increase the levels of TPT initiation.”
The MSF programme in Khayelitsha that partly informed this guidance began focusing on the diagnosis, prevention and treatment of DR-TB in children in 2020 as part of the project’s COVID-19 crisis adaptations in the high-density township of more than half a million people. To date, MSF has reached almost 300 individuals through family-focused activities, and while there have been many benefits to the community as a whole because of the programme, it appears the biggest benefit was for vulnerable children, who are usually the least served when it comes to TB treatment.
South Africa has been a global leader in the decentralisation of DR-TB care but the care of children at the community level has drastically lagged behind, with many children still being cared for by central hospitals.Dr Anja Reuter, MSF Khayelitsha’s medical activities manager

HIV and Drug-resistant TB Project in Khayelitsha
“This means that kids are kept away from their support systems for long periods of time, which is really disruptive and can be psychologically damaging,” says Dr Anja Reuter, MSF Khayelitsha’s medical activities manager.
When MSF began working closely with the health departments in the City of Cape Town and the Western Cape Province to provide care in communities with this approach, the diagnosis of DR-TB in children increased more than two-fold.
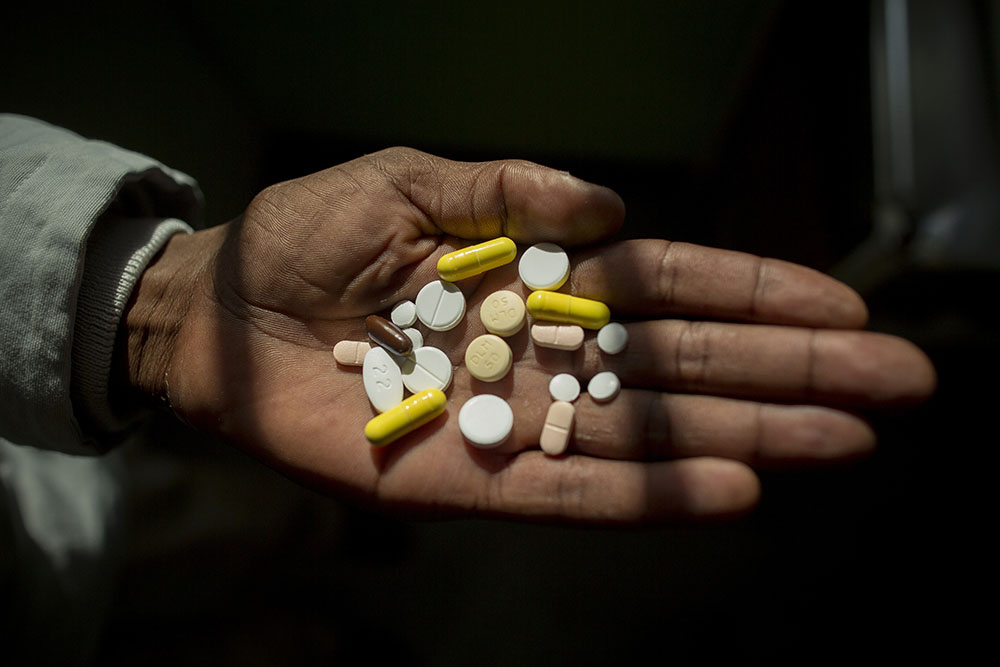
“Almost all of the children in our programme have been able to be fully treated in the community, and with child-friendly formulations of medications, which has been a huge relief to parents and carers who previously had to give the children adult-sized tablets, which were painful to swallow and had to be cut up so that the dosage was right,” she says.
In the MSF programme, the care of children with DR-TB was done largely by physicians and nurses working in clinics based in the community, meaning children and their families could get on with their usual daily activities while at the same time receiving world-class care without having to leave their homes.
What does it mean to take a family-centred approach?
TB and DR-TB are diseases that often affect an entire household because they are spread through the air people living together share. The public health approach to TB has, however, tended to focus care on the diagnosed individual rather than the entire family. As an example of this, children and adults may be given very different medications for treatment and prevention with little understanding of how the family will fare overall as a unit.
Further complicating things for families struggling with TB is that service delivery is usually based in healthcare facilities and ignores the context in which people live and interact with one another in communities. This often results in poor-quality care.
“These clinic-based models of care can actually make receiving treatment more difficult for family units struggling to make sense of what is happening to them and what they need to do as a family,” notes Reuter.
Writing in a blog for the journal Plos Global Health, Busisiwe Beko, a DR-TB counsellor now working for MSF in Khayelitsha, described the experience she had when she was pregnant with her daughter and became sick with DR-TB a number of years back.
“It was fear for what might happen to my child that preoccupied me most of all. How would the TB affect her? Would she get it too? Would the tablets I was taking to try and save my life end up hurting hers? I quickly found out that nobody in the clinic could answer any questions for me,” she writes.
When her daughter was born and diagnosed with DR-TB several months later, things became even more difficult. “Not only did I have my own health needs, but I also had to look after the needs of my child. Everything about the process of getting care for her and for me was also a struggle. We had to queue for hours, and when we did finally see the health staff, they were not equipped to deal with her as a child, me as a mother, and us as a family.”
MSF has worked for many years in Khayelitsha to introduce systematic changes to the way DR-TB is treated, but it was our experience during the COVID-19 crisis in 2020, with facility-based TB services often difficult to access, that made us realise how essential it is to meet families affected by all forms of TB in their houses and neighbourhoods.
“When people are visited in their homes, it allows health care providers and teams to give the family extended time away from the chaos that often characterises over-crowded clinics,” Beko writes, closing the blog with a call on healthcare leaders and practitioners to recommit to providing care for people where they need it the most.
MORE ABOUT THE MSF COMMUNITY-BASED TB CARE MODEL
Activities conducted during MSF household visits focused on children, adolescents, and vulnerable adults and included:
1) documenting all persons aged 18 years and younger residing in the household both at the time of the visit and in the month preceding the diagnosis;
2) counselling aimed at stigma reduction, tuberculosis education, and support through the diagnosis and treatment processes;
3) weighing all family members to assess for possible weight loss or changes in growth trajectories (children);
4) performing a basic physical examination;
5) offering HIV counselling and testing for willing family members;
6) screening for tuberculosis symptoms (including cough, fever, weight loss, night sweats, lethargy, and or reduced playfulness in children);
7) facilitating planned referral for persons with possible tuberculosis to clinics as needed for a full medical assessment and chest radiography;
8) collecting sputum or stool samples for tuberculosis testing among those with symptoms;
9) coordinating follow up and providing results; and
10) initiating preventive therapy for DR-TB among those who qualify for such treatment and in whom active DR-TB had been ruled out.



