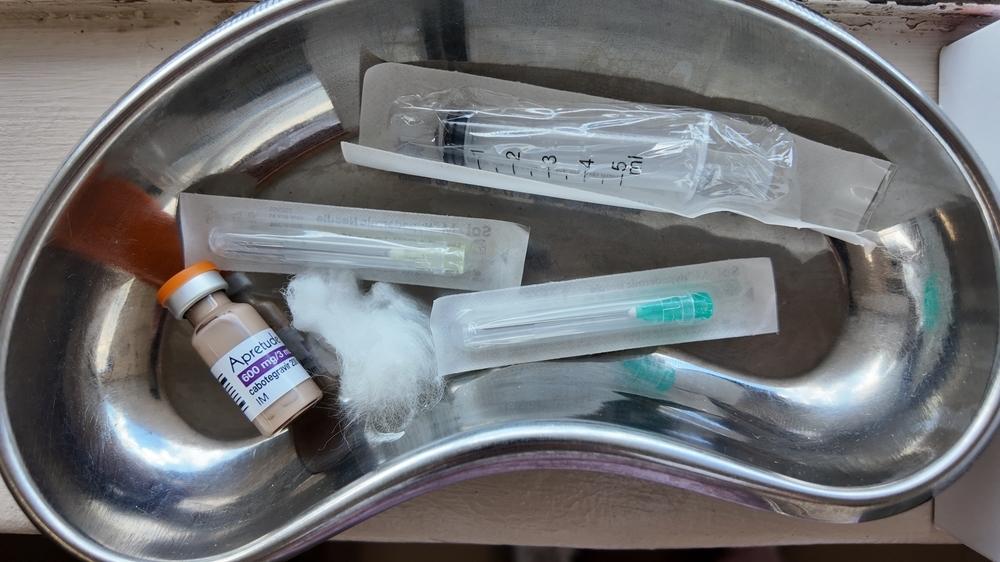
Doctors Without Borders (MSF) notes South Africa’s interest in exploring local production of lenacapavir (a long-acting injectable HIV prevention drug) and welcomes its ambition to diversify and expand global manufacturing. However, for local production to genuinely expand access, any agreement with Gilead must include substantially improved terms compared to the company’s existing voluntary licensing agreements with generic manufacturers.
Without such changes, local manufacturing risks deepening dependency by preserving Gilead’s tight control over supply, production, and geographic reach, and would simply lock South Africa—and many middle-income countries that are currently excluded by Gilead’s licensing from accessing generics when they come onto the market—into the same patterns of exclusion we are fighting to dismantle.
If lenacapavir is to fulfil its promise as a breakthrough in HIV prevention, governments must ensure that intellectual property protections, restrictive licensing and other barriers do not stand in the way of affordable production and global access.Candice Sehoma, MSF Access Regional Advisor for Africa

South Africa has a proud history of challenging barriers to HIV medicines to ensure equitable access for all. It must use this opportunity to negotiate equitable terms with Gilead, or even to issue a compulsory licence that would free local manufacturers from patent restrictions.
If lenacapavir is to fulfil its promise as a breakthrough in HIV prevention, governments must ensure that intellectual property protections, restrictive licensing and other barriers do not stand in the way of affordable production and global access.
-- Candice Sehoma, MSF Access Regional Advisor for Africa
Background
On 5 March 2026, the South African government announced that it is negotiating with Gilead Sciences to arrive at an agreement that would allow lenacapavir—a long-acting HIV-prevention injection—to be manufactured locally. The government has issued a call for expressions of interest to identify South African pharmaceutical companies with the capacity to produce lenacapavir.
HIV remains a key global public health challenge, with 1.3 million people becoming newly infected with HIV in 2023, with one every 24 seconds. UNAIDS modelling suggests recent cuts in global funding could lead to an additional 6,6 million new HIV infections by 2029.
South Africa has the largest population of people living with HIV in the world, at nearly 8 million people.
Lenacapavir, a long-acting injectable, has been proven to be highly effective in preventing HIV in cisgendered women (100% effective -PURPOSE 1 study) and in gender-diverse people (96% effective - PURPOSE 2 study). It is also available in twice-yearly injections, which would provide longer protection and could make adherence easier than the current medical HIV prevention options (emtricitabine/tenofovir disoproxil fumarate and emtricitabine/tenofovir alafenamide, which require a daily pill or event-based dosing, the dapivirine vaginal ring, which is replaced monthly, and cabotegravir, which requires an injection every two months).
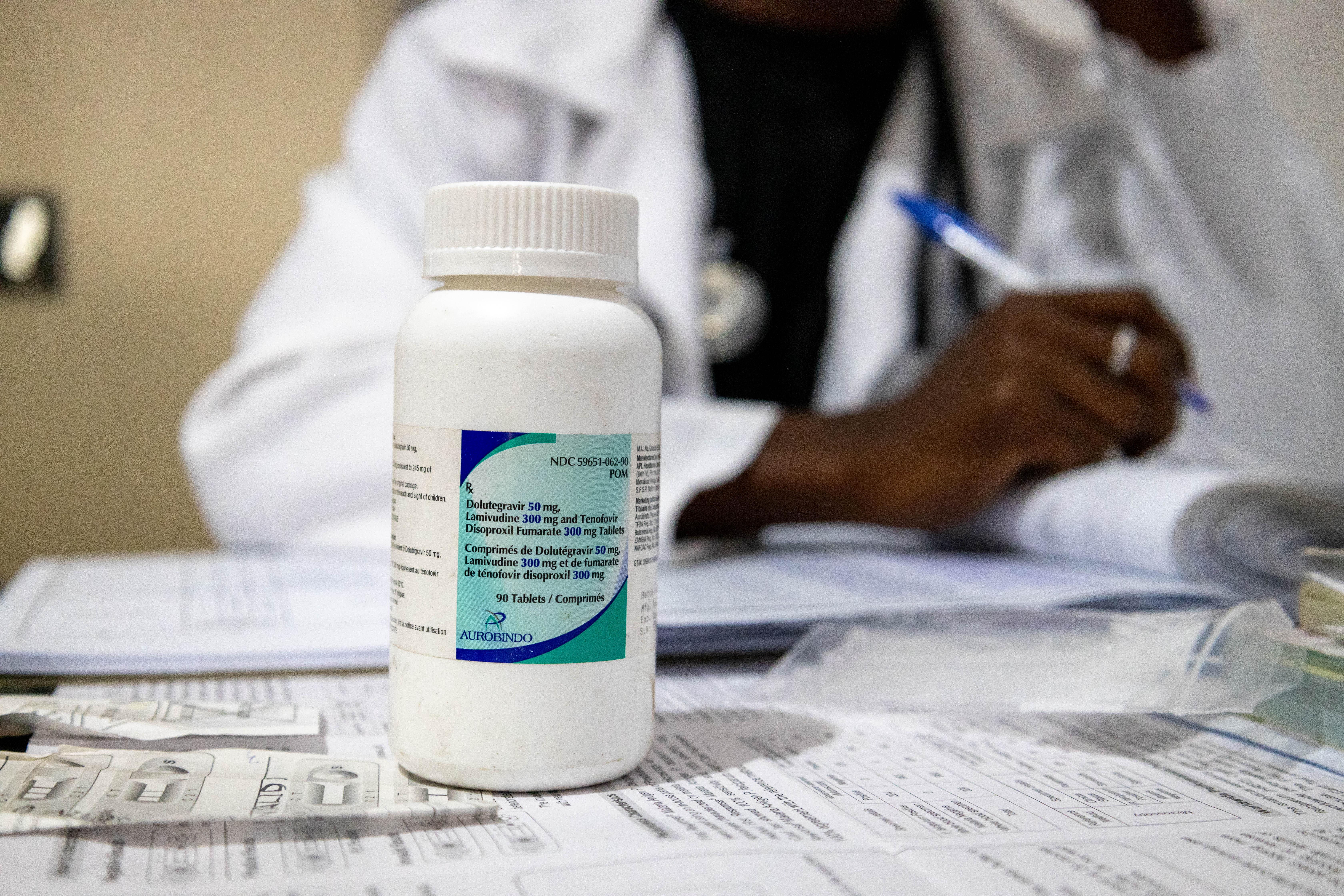
Currently, Gilead Sciences is the sole supplier of lenacapavir.
Gilead has signed a voluntary licensing agreement with six generic manufacturers, which will enable generic lenacapavir to be available in 120 countries and territories. However, some countries are excluded from the voluntary licence and will therefore not have this access, despite representing 25% of all new HIV infections. Some of the excluded countries (e.g., Brazil, Mexico, Argentina, and Peru) were participants in the clinical trials that enabled lenacapavir to be approved, but are now denied access to affordable forms of the HIV prevention tool they helped to bring about.
Gilead’-s voluntary licensing agreements also contain provisions that may limit the ability of generic manufacturers to expand supply beyond the designated territory.
These include:
- Geographic restrictions, under which licensees are prohibited from supplying lenacapavir outside the defined licence territories, which are reserved to Gilead.
- Strict anti-diversion measures, including requirements for product traceability and reporting obligations for downstream trading partners.
- Supply-chain provisions, which prevent licensees from sourcing lenacapavir materials or components from suppliers that also serve Gilead unless those suppliers first confirm that Gilead’s forecasted demand can be met.
These restrictions may constrain the potential for broader regional manufacturing and supply, even in countries where patent barriers may not exist or where governments use public-health safeguards to address them.