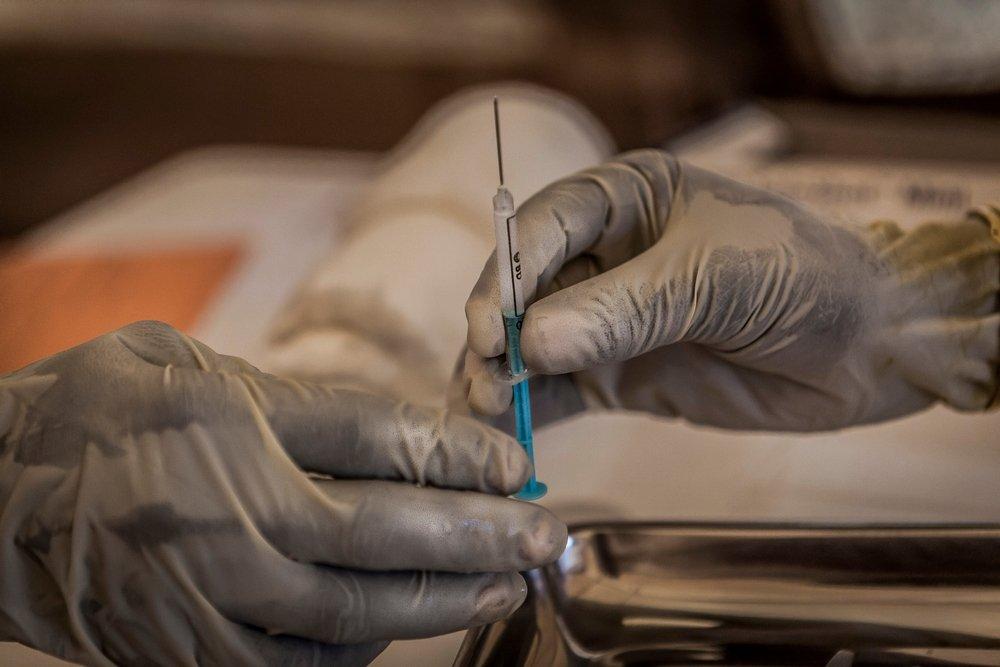
From April 11-13, the World Health Organization (WHO), governments, academics, and pharmaceutical industry and civil society representatives will meet in Johannesburg for the 2nd Fair Pricing Forum on access to essential medicines.
One critical topic up for discussion is the need for improved transparency in medicines pricing. Doctors Without Borders (MSF) is calling upon governments to put an end to the secrecy that rules in the field of pharmaceutical products.
As individual consumers, it is usually easy to compare the exact prices we will pay for things like cars, clothes and food in order to make informed purchasing decisions. But the same does not hold true for medicines.
Prices charged by pharmaceutical corporations vary wildly for the same medicine depending on who’s buying, and the exact prices that are paid are typically shrouded in secrecy.
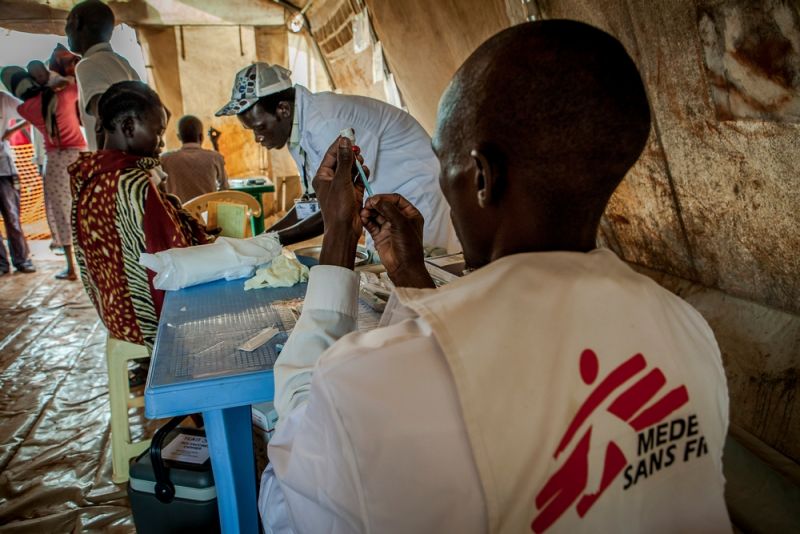
This lack of transparency gives pharmaceutical corporations the upper hand in price negotiations, keeping prices as high as possible while overstretched health systems and people in need of lifesaving medicines lose out.
Contrary to widespread belief, there is currently no direct connection between the costs of pharmaceutical research and development (R&D) and manufacturing, and the prices pharmaceutical corporations charge for medicines.
Instead, prices are increasingly set as high as ‘the market’ will bear, with pricing secrecy and confidential price negotiations the go-to tools that pharmaceutical corporations use to blindfold buyers and push prices continuously upward.
MSF witnesses the deadly impact that exorbitant medicines prices have on people in the places we work in. Pneumonia, for example, remains the world’s leading cause of childhood mortality, killing over one million children each year despite the existence of an effective vaccine: the pneumococcal conjugate vaccine (PCV).
In 2016, after a successful public campaign against the vaccine’s two producers, Pfizer and GSK, the companies committed to reducing PCV prices for MSF and other humanitarian organisations vaccinating vulnerable children in emergency settings.
However, in many countries, particularly middle-income countries ineligible for international donor support for vaccines, PCV remains priced out of reach. Although pharmaceutical companies claim to give poorer countries lower prices, Pfizer’s PCV13 has been sold at higher prices in Tunisia and Morocco (both lower-middle-income countries) than France.
Similarly, Ukraine pays approximately the same price as Spain for the pentavalent vaccine, which protects children from diphtheria, pertussis, tetanus, hepatitis B and Haemophilus influenza type B.
Countries sign confidential pricing agreements based on pharmaceutical corporations’ false assurances this will get them lower prices. In countries where publicly listed medicines prices exist, corporations set these at artificially high levels so they can appear to grant substantial discounts and favourable price reductions during negotiations.
These dubious rebates and discounts are also often granted only on condition of confidentiality. The pharmaceutical industry’s tactics are working. Medicine price secrecy stands in the way of fair pricing because it guarantees that one party will always arrive at the negotiating table disadvantaged and blindfolded: the public.
Meanwhile, as the United Nations starkly warned in their 2016 Access to Medicines report, prices continue to skyrocket for treatments against life-threatening diseases such as hepatitis C, cancers and diabetes – burdening health budgets and leading to rationing and delayed access to treatment all over the world.
Price transparency is both possible and desirable. MSF began documenting and publishing the prices of HIV antiretroviral (ARV) drugs in 2001. The Global Fund to Fight AIDS, Tuberculosis and Malaria has also long required that prices paid for the medicines it finances be publicly reported through its Price and Quality Reporting System.

Price transparency for ARVs has enabled competition and fair price negotiations, and the price of HIV treatment has dropped dramatically – from around US$10,000 per person per year in 2001 to around $100 today – enabling treatment scale-up to over 22 million people living with HIV/AIDS and saving millions of lives.
One thing is very clear: when countries know what others are paying for medicines, they have the leverage they need to demand fairer deals and increase access to treatment.
Numerous institutions and policymakers are recognising the harmful impact of medicine price secrecy on public health. In its recent report on the pricing of cancer medicines, the WHO came out strongly against confidential discounts and rebates that impair price transparency and competition.
In the US, legislative proposals to improve transparency have been introduced at the state and federal levels. And when national health officials meet at the World Health Assembly this May, a resolution will be put forward to demand that governments and the WHO take steps to increase transparency in the pharmaceutical sector, including on medicines pricing.
Fair pricing depends on fair negotiations, and there cannot be fair negotiations without transparency. MSF is joining patient advocates and healthcare professionals worldwide in calling on governments to make bold commitments to fair medicines pricing and mandate complete disclosure of the real prices at which medicines are sold. It is time for leaders to prioritise people’s health over pharmaceutical industry profiteering.