A South African MSF doctor spent six months working in a Malawian prison where living conditions put inmates’ health at great risk
Dr Simon Mendelsohn, a medical doctor from Cape Town, recently returned from a six-months assignment in Malawi where he treated prison inmates in Blantyre, Lilongwe, and Dedza where MSF runs medical activities, does research and advocates for improved living conditions.
An overcrowded, under-funded system has resulted in Malawi’s prisons becoming a breeding ground for TB, exacerbated by life-challenging conditions like HIV and malnutrition.
Here, Simon writes about the patients he met, the challenges he faced, and the way forward in improving the lives of Malawi’s neglected inmate population:

With a double barbwire fence and muddy, dirt-floored yard surrounded by concrete cell blocks, Maula Prison in Lilongwe is stark and uninviting. This is reinforced by the ragged, underfed, and sometimes emaciated inmates who greet us as we walk through the gate and into the yard.
But the true nightmare awaits in the cell blocks. These decrepit rectangular concrete structures with barred windows, which were built to accommodate 50 to 60 inmates, currently hold around 150 people. Each person has less than 1 square metre of floor space at night, meaning they must either sleep sitting up or with their flanks on the hard concrete floor and legs resting on other inmates. It’s these conditions which lead to infections and the spread of disease.
Maula prison houses some 2,842 inmates – over three and a half times its intended capacity – a mix of hardened criminals, petty thieves and minor offenders, as well as migrants without proper visas and vagrants picked up by police.
Working to support the medical system in Maula prison, we as MSF see the ravages of these conditions on the human body: the spread of TB, HIV and frequent cases of malnutrition, fungal infections and skin conditions like scabies. One inmate entered the prison last May as a young, strong, healthy 26-year-old. But as the months went on, he became more and more ill, eventually losing 20kg! He became malnourished, which then caused pellagra (a vitamin B3 deficiency) that was left untreated for several months. This led to chronic diarrhoea, terrible skin rashes and eventually dementia. This young man, full of life when he first entered the prison, was dead in the space of just 10 months trying to survive in these conditions.

‘Alarming numbers’
When we consider TB, prison congestion – combined with poor ventilation in the cells, under-nutrition and high rates of HIV – contributes to the rampant spread of this disease.
There were 94 new TB cases at Maula in 2016; 82 were diagnosed with TB at least 3 months after entering the prison. This means these men all likely developed TB while being incarcerated. There were also 5 TB-related deaths and several cases of inmates incapacitated by the disease.
By the end of February 2017, 43 inmates at Maula were on treatment for clinically confirmed TB. At 1,513 per 100,000 people, the current TB prevalence rate in Maula prison is more than three times greater than that of Malawi’s 2013 national TB prevalence rate in adults (452 cases per 100,000).
As a medical doctor, I am deeply concerned by the conditions of the men I treat and these alarming numbers, which point to a systemic problem. Chronic underfunding in Malawi’s prison system has been prevented the provision of adequate and nutritious food for inmates. In 2016 the Malawi Prison Service received only half the money it needed to feed everyone under its care. Much of this is used to pay off crippling debt, and what remains is only enough to feed 8,000 inmates.
But with an average of 14,000 inmates behind bars at any given time, a single daily meal of nsima (maize porridge) provided inconsistently provided, is not sufficiently nutritionally balanced to provide the daily minimum required calories or vitamins the human body needs. This leads to malnutrition and vitamin deficiency disorders (such as pellagra) resulting in prisoners’ immune systems rendered unable to protect their bodies. So near starving inmates are predisposed to active TB infection.
Inmates in Maula prison are also confined for months, and even years in spaces far less than the minimum international recommended 4 square metres per person. Consider for a moment that saliva droplets containing TB from a cough can travel up to 6 metres – the width of a Maula prison cell – far, this places all the inmates in the cell at risk of TB infection. The 13.7% of inmates living HIV are at especially higher risk of contracting TB. The total lack of TB patient isolation facilities also means inmates with confirmed TB share cells with those not infected. And so, a person with active TB sleeping in a congested cell places the other 150 cell inhabitants at risk.
The way forward
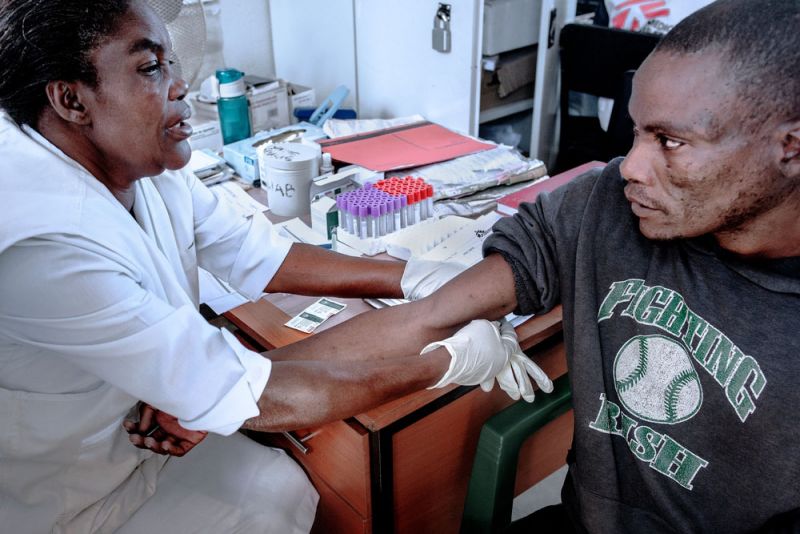
In 2014 MSF introduced a comprehensive package of medical interventions to prevent, screen, treat, and monitor HIV and TB in 2 central Malawi facilities (Maula and Chichiri prisons) determined by minimum standards set for prisons by the Southern African Development Community. More recently MSF rolled this out to two smaller district prisons in Dedza and Kachere. This involves screening inmates for HIV and TB when they enter prison, during their stay (twice annually), and at release back into the community. MSF also provides auxiliary out-patient care, including a therapeutic nutritional programme for malnourished inmates, as well as treatment of other medical conditions.
However, these interventions are not enough to control the rampant TB epidemic in the prisons. The root of the problem is that inmates are underfed and stuffed into overcrowded cells with inadequate ventilation.
As a way forward, Malawi’s prisons need to be decongested, ventilation improved, and prisoners adequately fed. A minimum package of care must be provided in all prisons in Malawi, and the rest of the SADC region. Until such time as the conditions improve, a prison sentence in Malawi is potentially a death sentence.
Find out more about MSF's work in Malawi.
