Beni is one of the recurring hotspots of the current Ebola virus disease epidemic in North Kivu province, Democratic Republic of the Congo (DRC). For more than a year, the outbreak response has been in full swing in the city. On-site since the early days of the epidemic, Doctors Without Borders (MSF) has recently started supporting vaccination activities, a promising tool in the fight against the virus disease. Yet reaching the right people in time is a complex endeavour.
Esther only winces lightly when a doctor of the vaccination team injects the investigational Ebola vaccine called rVSV-ZEBOV into her left upper arm in Kimbangu, a community in the south-west of Beni. Justin*, her two and half-year-old son, bursts into tears when he sees a new syringe being filled, and only calms down a few minutes after receiving his shot. The vaccine feels painful in the arm, but side effects are mostly mild and early results show the vaccine provides effective protection for a promising 95% of participants after ten days.
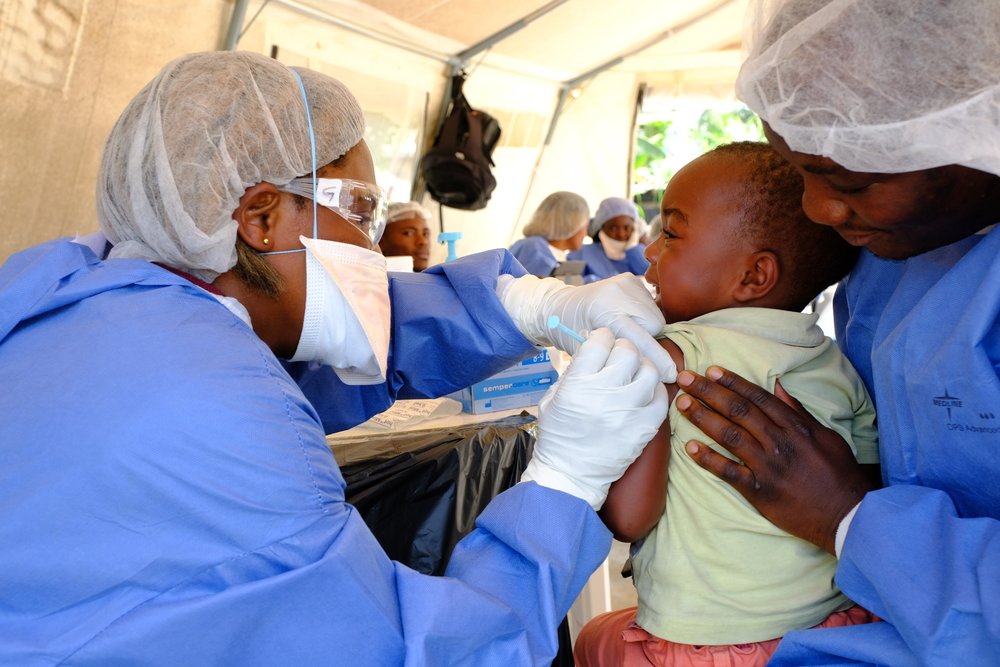
Esther and her son came to one of three vaccination sites set up by MSF every day in Beni, as part of the latest efforts to contain Ebola together with the response teams of the Ministry of Health and the World Health Organization. “There was a confirmed Ebola case in my neighbourhood, and a surveillance team told me that we should get vaccinated as we are likely contacts”, Esther said.
Setting-up the vaccination sites is a well-coordinated routine. A series of plastic tables are lined up next to a waiting area, registration and consent forms put into place, and the vaccination team dresses up in protective gowns. Then, an MSF vehicle delivers the first vials of the vaccine in a cooling container, and a member of the surveillance team starts identifying eligible participants.
While Ebola cases have been on the decline in Beni since late August 2019, there are still new suspect and confirmed cases admitted to isolation zones in local health care facilities or the MSF-operated Ebola Treatment Center (ETC) every day. Twice already, in December 2018 and June 2019, the outbreak seemed contained, only to soar again with even higher numbers.
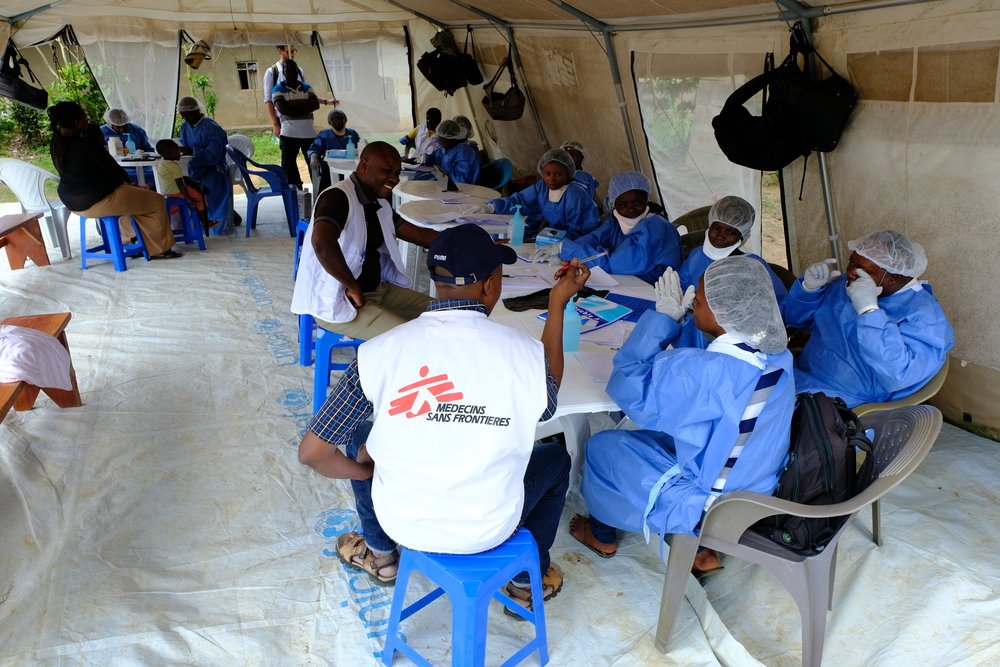
Ebola remains a deadly disease. Despite the availability of a vaccine to prevent infections and new treatments for confirmed patients, over 3,100 people have been infected since the beginning of this tenth and biggest outbreak in DRC, and over 2,100 died as of mid-September. Symptomatic patients showing fever, diarrhoea, or vomiting are infectious and should be isolated and treated as fast as possible. Yet in North Kivu, the average time span from suspecting to diagnosing an Ebola case is five days, during which patients often travel and visit several health centres.
Identifying and vaccinating contacts like Esther and Justin is, therefore, crucial to protect people at risk, and poses one of the major challenges of containing the outbreak. The three MSF-teams supported 700 vaccinations in the first two weeks of vaccinating alone, and over 51,000 people have been vaccinated in Beni by the national Ebola response and its partners so far.
Nevertheless, due to the restricted use and the investigational status of the vaccine, the vaccination strategy in North Kivu is currently limited to a ring approach. Only direct and indirect contacts of probable and confirmed Ebola cases or frontline workers like doctors and humanitarian staff are targeted by the current campaign. Through the outbreak, national surveillance teams however only manage to trace a quarter of known and probable Ebola contacts, while a majority remains unidentified or is never followed up with. MSF called for an international, independent committee to evaluate and extend the strategy and manage vaccine supplies more transparently.
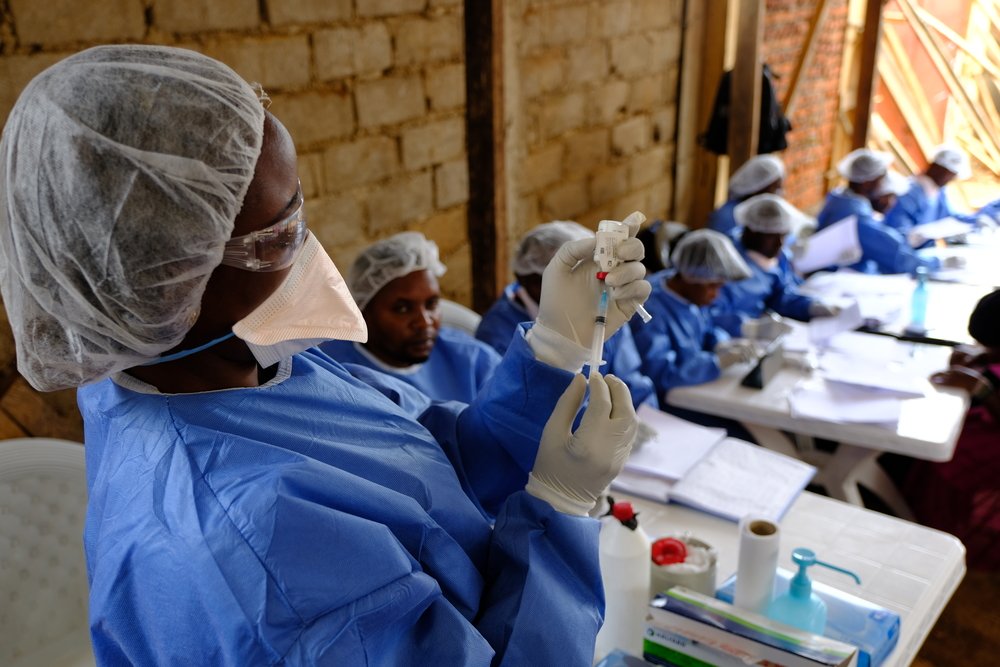
“We would like to broaden our vaccination strategy and be more flexible in responding faster to health zones with confirmed Ebola cases, but are currently limited to a fixed number of daily doses and working in pre-allocated vaccination sites”, said MSF Activity Manager Joseph Musakane.
Persisting fears and misconceptions around the vaccine in local communities pose an additional challenge for vaccination teams. “Many people believe the shot causes impotence, mental illness, or even Ebola itself, said Joseph MbokaniI Kambale, a sensitizing agent with the national Ebola response. “Others mistake Ebola symptoms for another disease or suspect poisoning, and we often need to convince people to come and get vaccinated”, he added.
Making treatment more accessible and building trust with the local population proved equally important for patients presenting with Ebola symptoms earlier in the outbreak. At first, MSF was working at a large central transit centre for suspect cases but soon realized isolation capacities were much better positioned closer to communities. “We started integrating small isolation structures into six of the eighteen health centres of Beni’s health zones, where patients and suspect cases felt more comfortable to present at the time”, said Tristan Le Lonquer, Emergency Coordinator with MSF in Goma.

The health centres now also make for possible vaccination sites, offering a secure and sheltered space close to communities. At the same time, MSF strengthens the centres’ existing primary health care services. “We support ambulatory patient consultations, maternities, or laboratory capacities, which are much-needed services at risk of being neglected during the complex Ebola response”, added Le Lonquer.
A second experimental vaccine requiring two doses given 56 days apart has just ben greenlighted in DRC as part of an extended clinical trial, and MSF and its research arm Epicenter are part of the global consortium leading the rollout.
In Beni, ending the deadly Ebola epidemic remains complex task, and MSF has only recently taken over the large Ebola Treatment Center with 13 isolation cubes for emergency care, 3 large isolation wards for up to 40 patients, and over 160 staff.
“Breaking the chain of transmission requires us to extend our vaccination approach, provide integrated isolation and treatment options, have a central ETC available, but also sustain other health care needs and build a relationship of trust with the local community. We need to be present on all fronts to win the complex fight against Ebola”, Le Lonquer concluded.
* Participant names have been changed to protect patient privacy.
