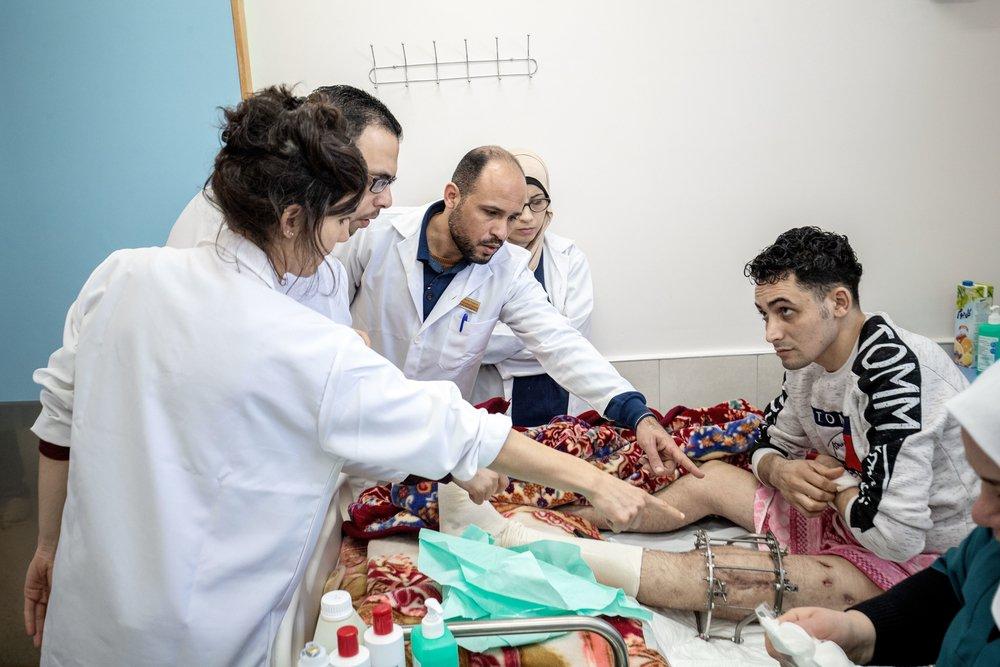
Amid the COVID-19 pandemic, Doctors Without Borders (MSF) teams in Gaza continue to provide medical care to hundreds of people wounded in over 20 months of protests known as of the Great March of Return.
By early June, 72 patients with COVID-19 had been confirmed in Gaza, all among people already isolated in quarantine centres after entering Gaza from abroad, and one COVID-19 related death had been reported. The first cases of COVID-19 in Gaza were identified in March when two residents returning from abroad tested positive. While many thought that the virus would spread quickly through one of the most densely populated areas in the world, the efforts and the preventive measures that the local authorities and other healthcare actors have put in place have so far prevented the widespread transmission of the novel coronavirus among Gaza’s population.
Nonetheless, COVID-19 is still a heavy sword of Damocles hovering on Gaza, a 360 square-kilometre stretch of land housing two million people. An unchecked outbreak would dramatically worsen the already critical situation of healthcare in Gaza, which has been crippled by a chronic shortage of medical services, resources, professional training, medicine and equipment.
Thirteen years of the blockade imposed by the Israeli government, internal political divisions and three military operations in the last seven years have driven Gaza’s healthcare system and its economy to collapse, and led to an appalling rate of unemployment (up to 60 per cent among young adults). This has turned the Strip into a dreadful cage for many people and pushed thousands to take to the streets over the last two years, in protests known collectively as the Great March of Return.
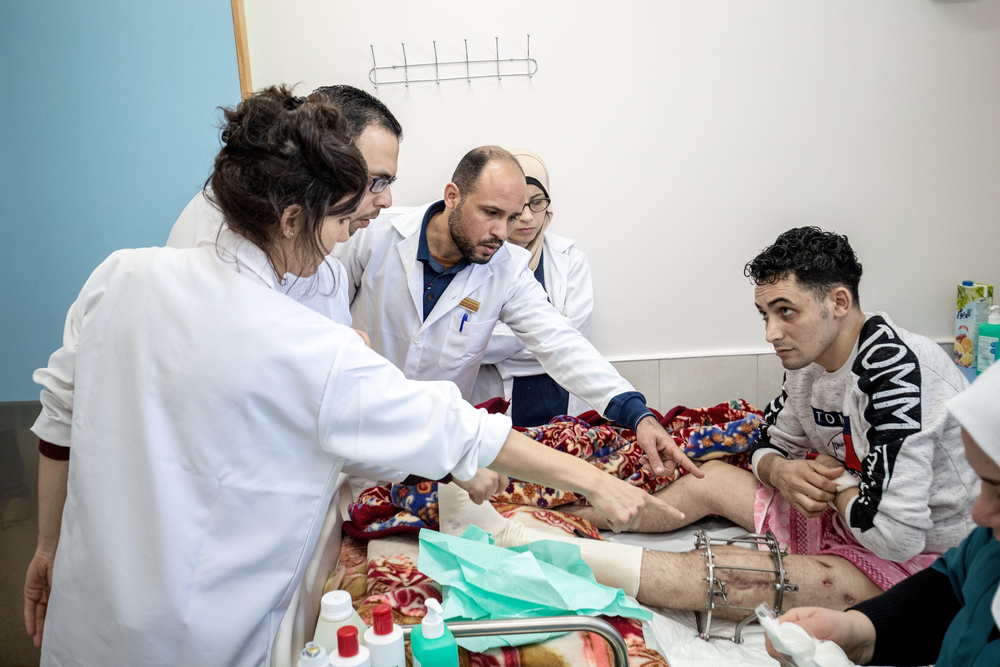
According to the UN, between March 2018 and December 2019, 8,800 people were injured by live ammunition fired by the Israeli army near the fence separating Gaza from Israel while attending protests. After more than two years since the beginning of the protests, many of them still need follow-up surgery, extended treatment for infected wounds, and require long courses of rehabilitation and specialised care. The threat of COVID-19 is making their excruciating recovery process even longer and harder since many medical services and activities have been reduced or temporarily suspended.
MSF opened its first project in Gaza in 2000. We currently manage two inpatient departments, three surgical teams and four outpatient clinics to treat patients with trauma and burns. In 2018, MSF scaled-up its medical capacity to care for the thousands of people shot during Great March of Return protests. MSF teams provide plastic and orthopaedic surgery to close large wounds caused by live rounds and is developing capacity to repair the loss of and damage to the bone. After surgery, our teams provide dressing changes, physiotherapy, health education and psychosocial support.
Since March 2018, MSF teams in Gaza have treated over 4,830 people injured in the protests. In 2019 alone, MSF performed almost 2,000 surgical interventions and provided more than 71,000 physiotherapy sessions.
Mohammed, 28, has his left leg held in a metallic external fixator. He was shot on 30 March 2018, the first day of the protests. “Two years ago, I went to the fence to call for our right to a dignified life. I didn’t want to harm anybody. I wanted a solution for our situation, not a war,” he says. “Life in Gaza is unbearable. We survive here only because we have no choice. We go to school, we graduate and then we look for a job that doesn’t exist, while the next military escalation could destroy our home. When we want to have children, we have to think about the life we can give to them. Is it fair to have a child in Gaza? Is it a life or a death sentence?”
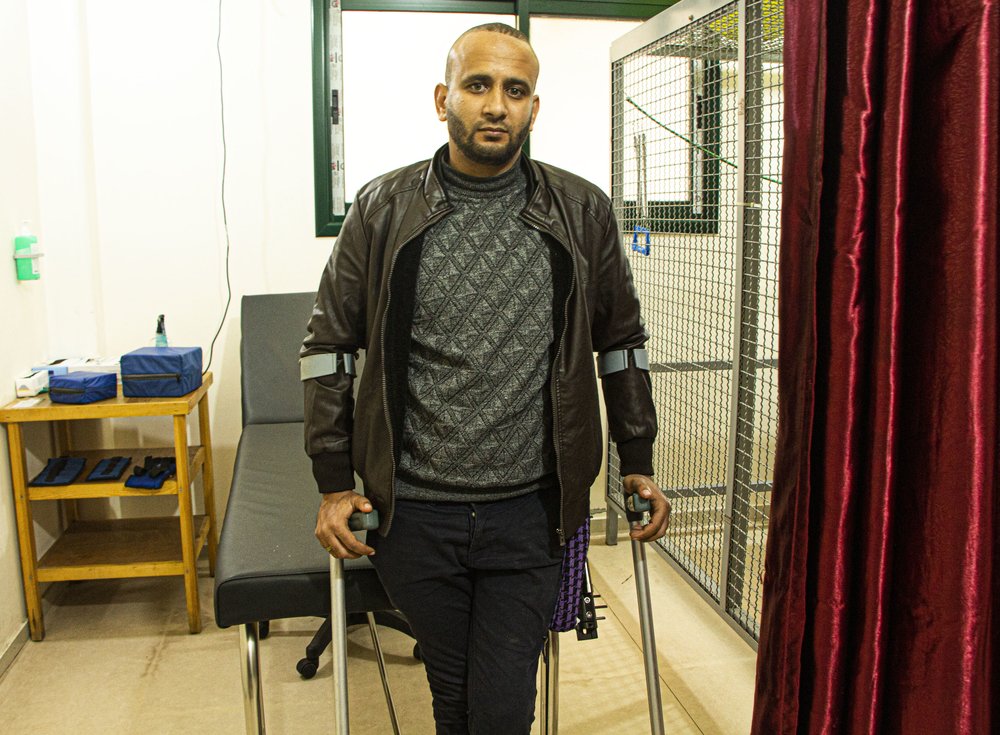
After over a year in the hospital and many surgeries, Mohammed still has a long recovery process ahead. “I haven’t really slept for two years; the pain keeps me awake at night. In the morning, the first thing I see is my leg and the fixator around it, and I wish I didn’t have it. I’m losing hope. I studied business administration and I used to manage my own taxi company. Now I can’t walk, I can’t drive, I can barely move.”
Mohammad is one of the patients receiving regular treatment, medical follow-up, physiotherapy and psychosocial support at the MSF clinic in Gaza City. However, he hasn’t been able to regularly attend his medical and physiotherapy sessions at the clinic lately because services have been reduced to prevent the spread of COVID-19.
In the last three months, measures to prevent the spread of COVID-19 have forced us to adapt our regular services. While MSF’s commitment to treat the hundreds of patients wounded during the protests has not changed, our teams at the four clinics and two hospitals supported by MSF have had to reduce non-urgent activities and services. This gives them the capacity to reinforce preventive measures and infection control precautions and enables medical personnel to prepare for a potential outbreak in Gaza.
“Working under the threat of COVID-19 means we must pay greater attention to protecting our patients and our medical personnel,” says Dr Mohammed A. Abu Mughiaseeb, MSF medical referent in Gaza. “We wear additional protective equipment and we implement precautionary measures, like drastically decreasing the number of patients coming to the clinics for physiotherapy and temporarily suspending non-urgent surgical interventions to reduce the risks. We’re doing what it takes to ensure the continuity of our services. We simply can’t stop providing medical assistance to people with such complex injuries; otherwise, we will compromise their already long and difficult recovery process.”
Rida, 45, was also injured attending the protests in December 2018. A bullet fired by an Israeli sniper tore apart at least 10 centimetres of her tibia. “After more than a year my leg hasn’t healed yet. I still have an external fixator and the pain never leaves me,” she says.
“The doctors told me that I have a long way to go, but I’m determined to get my life back and walk again. I used to provide for my family, working in a kindergarten, but now I cannot even stand on my own. My husband is fragile; he has a mental illness, so I have to be the mother and the father for my five daughters and four sons. None of them has a job. The only thing I want now is to stand up and take care of my family.” Rida’s leg is surrounded by a metallic external fixator with 28 pins to keep her bones in place. She will need further surgeries, physiotherapy and treatment.
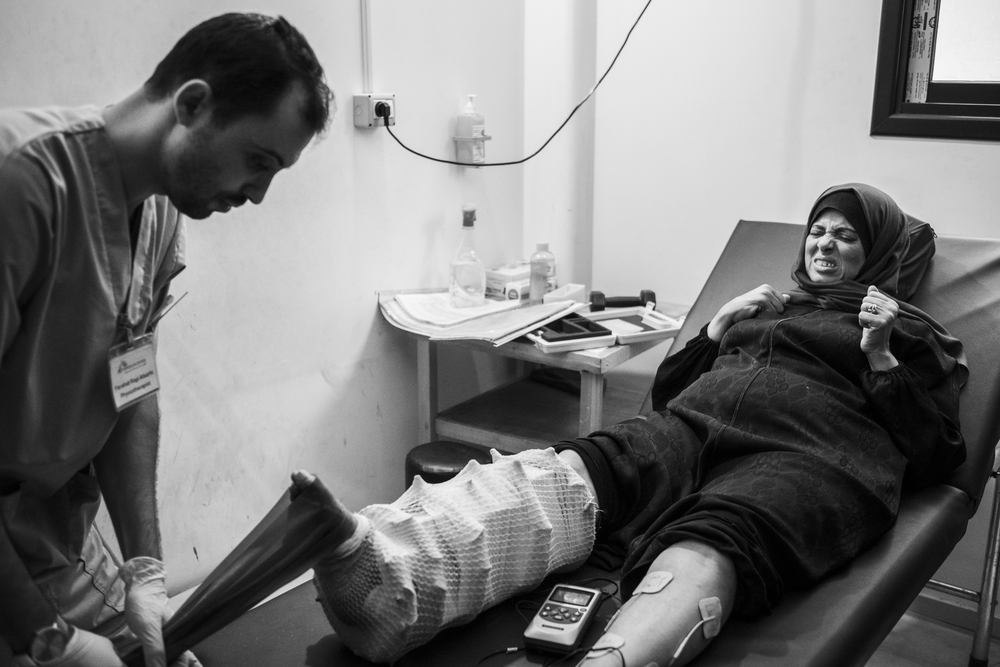
“Reducing the frequency of the physiotherapy sessions for our patients means prolonging their recovery process and, in some cases, even jeopardising the progress they have made,” says Shadi Al Najjar, MSF physiotherapist supervisor.
“That’s why it is essential to ensure, as much as possible, some continuity of services, even if it is not optimal. We provided our patients with physiotherapy treatment tools and explained how to use them to exercise at home. And we follow up with them daily by phone. The hardest thing now is keeping their motivation high and preventing them from dropping off. The exercises can be painful, and the encouragement and personal support we give them during the sessions are incredibly important in their recovery process. So right now, these phone calls are essential.”
MSF teams in Gaza provide psychosocial services for people severely injured in the Great March of Return protests. This support is crucial because most of the patients have been experiencing stigma and isolation, and have developed psychological injuries on top of their physical pain. The injuries they have suffered during the Great March of Return have impacted all corners of their lives, often leading to social isolation, loss of friendships and strained relationships with family members.
The restrictions and the social limitations, compounded by a sense of fear and uncertainty that has come with the COVID-19 pandemic, have deepened their psychological discomfort. Since mid-March, all face-to-face activities have had to be reduced due to COVID-19, but MSF counsellors continue supporting our patients with regular phone and video calls.
“When our patients aren’t able to come to the hospital or the clinic they miss an important moment of socialisation, as many of them suffer from depression and choose to self-isolate. The medical personnel and the other patients are often a safety net and the only social interaction they have,” says Luciano Canchelara, MSF mental health activity manager in Gaza. “Now that this mutual support can’t be guaranteed, it’s even more important to make those people feel cared for. The COVID-19 pandemic has forced us to adapt our activities, but stopping them is inconceivable. We see every day how much of a difference it makes to our patients.”