Five epidemics to watch out for in 2016
Outbreaks of cholera, measles and meningitis are common in resource-poor settings, despite affordable and efficient vaccinations being available; high seasonal peaks of malaria go unreported, and therefore the health response remains insufficient, and outbreaks of the lesser-known illnesses such as dengue and Chikungunya have recently been reported in new countries and areas.
These are all epidemics that could either erupt or worsen in 2016, and we need to be prepared. Vaccination needs should be identified and addressed pre-emptively, surveillance should be reinforced, responses should be adapted as the one-size-fits-all approach often does not work, and R&D for diagnostic tests and treatments should be prioritised. Below are some recommendations that we as MSF suggest, based on what we have seen in the field.
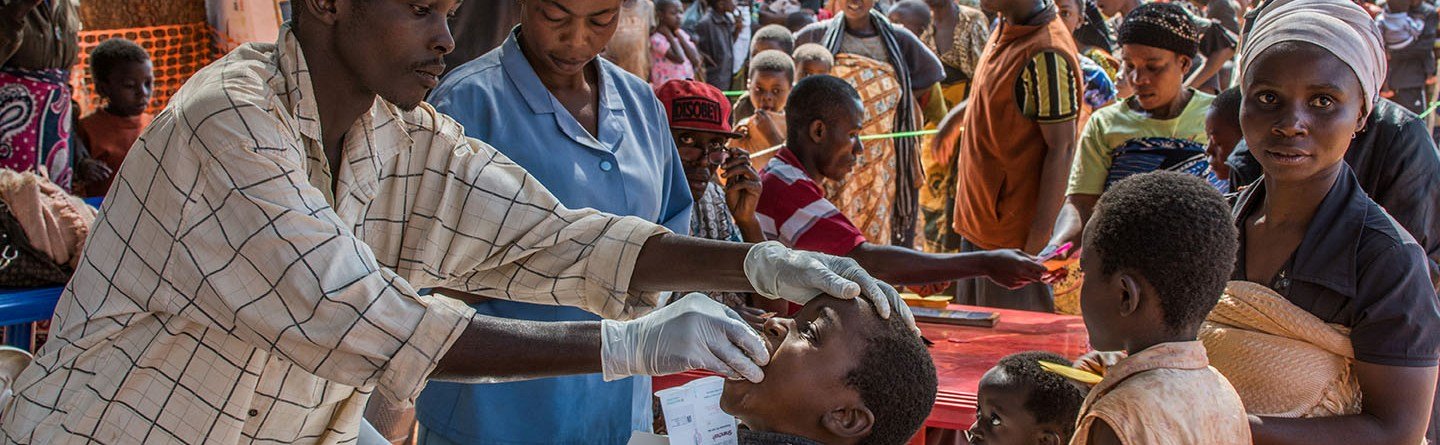
Cholera
Cholera is a water-borne, gastrointestinal infection that causes acute watery diarrhoea and vomiting, which can lead to severe dehydration and death within hours if left untreated.
Cholera is transmitted by contaminated water or food, or through direct contact with contaminated surfaces. The infection is most common in densely populated settings where sanitation is poor and water supplies are unsafe.
Displaced populations, people living in areas without basic infrastructure, and those living where conflict has disrupted services are most at risk.
Cholera outbreaks are predictable and can be prevented and treated. Unfortunately, in several of the worst-affected countries, basic needs are unmet, preparedness is insufficient and the response to outbreaks is both late and poor.
In 2014, MSF treated 46,900 people for cholera in 16 outbreaks affecting six countries (Cameroon, Democratic Republic of Congo (DRC), Haiti, Niger, Nigeria and South Sudan).
As soon as an outbreak is suspected, patients are treated in centres where infection control precautions are taken to avoid further transmission of the disease. Strict hygiene measures must be implemented and large quantities of safe water must be made available e.g. through water chlorination.
In addition to these measures, the oral cholera vaccine reduces transmission of the infection. However, due to short supply, its use is restricted; currently, the vaccine is primarily used in outbreak response or as a preventative measure in high-risk situations such as camps for displaced people.
A stockpile managed by the International Coordinating Group (ICG) was created in 2013 to maximise the impact of the doses available.
Countries that want to use the vaccine to prevent outbreaks in high-risk areas have to submit their proposals to the ICG, where they are assessed by a group of experts and arbitration is undertaken if required.
The scarcity of vaccines means that countries and humanitarian actors cannot vaccinate large populations as part of an overall preventative strategy in countries where cholera is endemic, in specific risk areas or when confronted by an outbreak.
An example of this in 2015 was the cholera outbreak in Juba, the capital of South Sudan, which has an estimated population of 500,000 people.
To help reduce the spread of cholera in the city, MSF launched a vaccination campaign in coordination with the South Sudanese Ministry of Health but unfortunately, the number of doses available was not enough to cover the entire population at risk.
Therefore MSF in agreement with the Ministry of Health decided to implement a single dose campaign (instead of the usual two doses) targeting areas with the highest transmission in Juba.
MSF ASKS
There are only two WHO pre-qualified vaccines available. The most adapted vaccine for outbreak response is produced by an Indian company that has no capacity to scale-up production to cover worldwide needs.
The majority of doses are available only through the stockpile system. There is a need for scale-up production and for more options to be validated by the WHO.
Currently, a two-dose strategy is recommended. According to researchers, a single dose strategy may prevent more cases than a two-dose strategy that is given to half as many people.
More flexibility in the allocation of vaccines and support from the WHO for single dose campaigns is required.
Malaria
Malaria is transmitted by infected mosquitoes, and severe malaria can lead to organ damage and death if left untreated.
On average only two in every 100 cases of malaria reported are the result of outbreaks, but one in every four deaths is outbreak-related.
Although the total number of malaria cases worldwide is decreasing thanks to the success of control and elimination initiatives, unexpected high seasonal peaks and epidemics still occur and result in high mortality rates.
In addition, we are currently facing the threat of resistance to antimalarial drugs and to insecticides.
In 2014, MSF provided treatment to 2,114,900 patients affected by malaria and gave seasonal malaria chemoprevention (SMC) to more than 750,000 children below five years of age. MSF also responded to malaria emergencies in DRC and Chad.
Population displacement, global warming and gaps in control and elimination strategies have resulted in localised increases in malaria cases.
In countries or areas with the ongoing transmission, it is very difficult to identify an outbreak. Weak surveillance and a lack of functional alert mechanisms mean that unexpectedly high seasonal peaks remain undetected and an adequate response is not deployed in time.
Patients lack access to timely treatment and the number of deaths increases at the community level. In 2014 and 2015, unexpectedly high seasonal peaks of malaria in DRC and Chad translated into high mortality at the community level.
Free care was not guaranteed diagnostic tests and lifesaving drugs were not available in remote rural areas.
MSF ASKS
- Ensure a universal access to diagnosis, treatment and preventive measures: diagnostic tests and treatment need to reach the rural and hard to reach areas.
- Increase the availability of injectable artesunate for the treatment of severe malaria, and increase blood transfusion capacity.
- Adapt the vector control tools according to emerging trends of resistance to insecticides.
- Reinforce malaria surveillance and define the outbreak threshold per country, per region and per district to improve alert mechanisms. The meteorological data needs to be incorporated into the analysis in order to identify earlier potential outbreaks or unexpectedly high seasonal peaks to avoid a high number of deaths.
- The WHO should provide better guidance for the use of preventative strategies, such as SMC, mass drug administration (MDA), intermittent preventive treatment (IPT) and Focused screening and treatment (FSAT) for outbreaks
- Free malaria treatment during outbreaks or seasonal peaks needs to be guaranteed.
Measles
Measles is a highly contagious viral disease, for which there is no specific treatment. In high-income countries, most people infected with measles recover within two to three weeks, and mortality rates are low.
In developing countries, however, the mortality rate can be 3 to 15%, rising to 20% during outbreaks and in areas where people are more vulnerable.
Death is usually due to complications such as diarrhoea, dehydration, severe respiratory infection or encephalitis (inflammation of the brain).
Children suffering from measles are more likely to become malnourished and are more prone to other infections such as pneumonia or malaria.
There exists a highly protective, safe and cheap vaccine against measles, but coverage in many countries remains insufficient and there is currently a resurgence of measles worldwide.
The number of measles cases and related deaths have decreased dramatically over the past few decades thanks to the introduction of the vaccine through expanded vaccination programmes.
But the emphasis is given to regular preventative activities sometimes has a backlash on outbreak response, which is not prioritized, can be delayed or prevented. In 2014, MSF treated 33,700 patients for measles and vaccinated 1,513,700 people in response to outbreaks.
Delays in identifying and declaring an outbreak, and initiating outbreak control measures are common. The response to outbreaks of measles is usually late and very generic.
The accepted strategy of vaccinating specific age groups needs to be re-assessed in order to maximise the impact of reactive campaigns.
There is also a need to rethink and to be more creative when it comes to outbreak response – it is currently very dogmatic.
MSF ASKS
- Patients should be treated for free during a measles outbreak (including for associated pathologies, such as malaria).
- There is a need for greater involvement of emergency actors and the Ministry of Health in the provision of case management.
- Long-term vaccination campaigns should support, not block, epidemic response. To prevent outbreaks we need to build on the current policies of routine vaccination and planned supportive activities to improve their impact – so, for example, how to build on the strength of polio campaigns/Supplementary Immunization Activities (SIAs)
- Need better surveillance and early declaration of outbreaks – flexibility and reactiveness.
- The response needs to be adapted to each outbreak, as the one solution/strategy for all is not working. Epidemiological data such as affected age groups, mortality, time from outbreak onset, geographical dissemination, etc needs to be taken into account to adapt the response.
Examples:
Dadaab, Kenya, 2011
During the measles outbreak in Dadaab in 2011, MSF had to fight to increase the vaccination age to 30. Cases were originating from a non-vaccinated region of Somalia and young adults were severely affected.
DRC, Katanga, 2015
There have been recurrent measles outbreaks in the same area, demonstrating that SIAs (by the Ministry of Health, UNICEF, supported by GAVI, etc) are not working fully.
Measles is still present in many regions and is popping up in different places. There needs to be a rethink about how to address different outbreaks of measles depending on their duration, phase and location, whether they are erupting in the same country or region.
Meningitis
Meningitis is the inflammation of the thin membranes surrounding the brain and the spinal cord. It is most often caused by infection – bacterial, viral or fungal.
Meningitis occurs throughout the world, but the majority of infections and deaths are in Africa, particularly across the ‘meningitis belt’, an east-west geographical strip that runs from Ethiopia to Senegal. In this area, epidemics are most likely to be caused by meningococcus A.
A new vaccine against this strain provides protection for at least 10 years and even prevents healthy carriers from transmitting the infection.
Large preventive vaccination campaigns have now been carried out and have resulted in a decrease in the number of cases and the likelihood of meningitis A outbreaks.
However this year, there could be a large number of outbreaks of other strains of meningitis across the ‘meningitis belt’. In 2013, small outbreaks of other strains were reported in Nigeria and Burkina Faso, and there has been a gradual increase in the number of meningitis C cases.
Meningococcal C vaccines are not available in sufficient doses, those that are available are very expensive, and production is not currently being scaled up
MSF ASKS
- Rational use for highest impact – focus on the medical and outbreak control criteria. Use of the vaccine should not be a political consideration. The vaccine needs to be available, accessible and affordable to those who need it – WHO and UNICEF need to ensure that sufficient stocks are mobilised to cover the needs of high-risk countries during the next meningitis season.
- Encourage diversification of manufacturing and procurement channels (not only UNICEF) to ensure a rapid response when an outbreak occurs.
- Manufacturers need to ensure that – at the very least – their commitment to the ICG is fulfilled and they should increase vaccination production immediately.
- The WHO need to push/accept/promote alternative strategies to vaccination to protect individuals and limit outbreaks (e.g. mass distribution of antibiotics).
Example:
Niamey, Niger, 2015
In 2015 in Niger, lack of visibility on meningitis vaccines and treatment possibilities in remote areas forced MSF to adjust its intervention. In 2016, the situation is even more worrying. The big meningitis outbreak is predicted and the available amount of vaccines is known to remain limited.
Emerging and re-emerging viruses and parasites
Outbreaks of dengue, Chikungunya, Zika, Middle East Respiratory Syndrome (MERS) and haemorrhagic fevers have all been reported in 2015.
Although the current death tolls from these outbreaks are not that high (Ebola being an exception), the number of cases are on the rise and outbreaks of dengue and Chikungunya have been reported in new countries and areas.
Though not all of these have high fatality rates, they are painful and incapacitating, which means that people can’t work or study. Currently, there are no reliable and easy to use diagnostic methods, preventative measures or treatments available.
Parasitic infections such as visceral leishmaniasis (kala-azar) that were under control are now on the rise again. This is due to a number of reasons: people being displaced from or towards endemic areas; climate changes which can cause an increase in vectors; and outbreaks of conflict which can result in the disruption of health services and the collapse of control programs.
In 2014, MSF treated 4,700 Ebola confirmed patients, 1700 patients for Chikungunya and 9,500 patients for kala azar including responding to an outbreak affecting South Sudan.
MSF ASKS
- Identify and declare outbreaks in order to speed up vector control measures.
- Capacity building and training for better identification of diseases, case management and infection control.
- Step up health education to avoid risky behaviour, and inform the affected population about the diseases and what to do if infected.
- Research and development for diagnostics, vaccines and treatments
Download the report "Epidemics: Neglected emergencies?"
Read the report online
