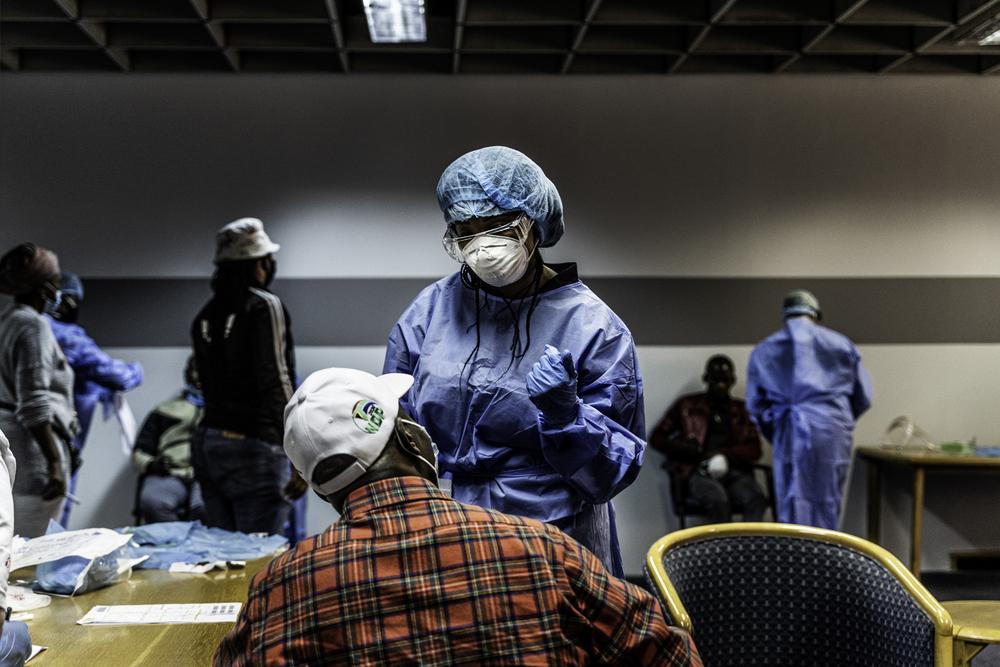
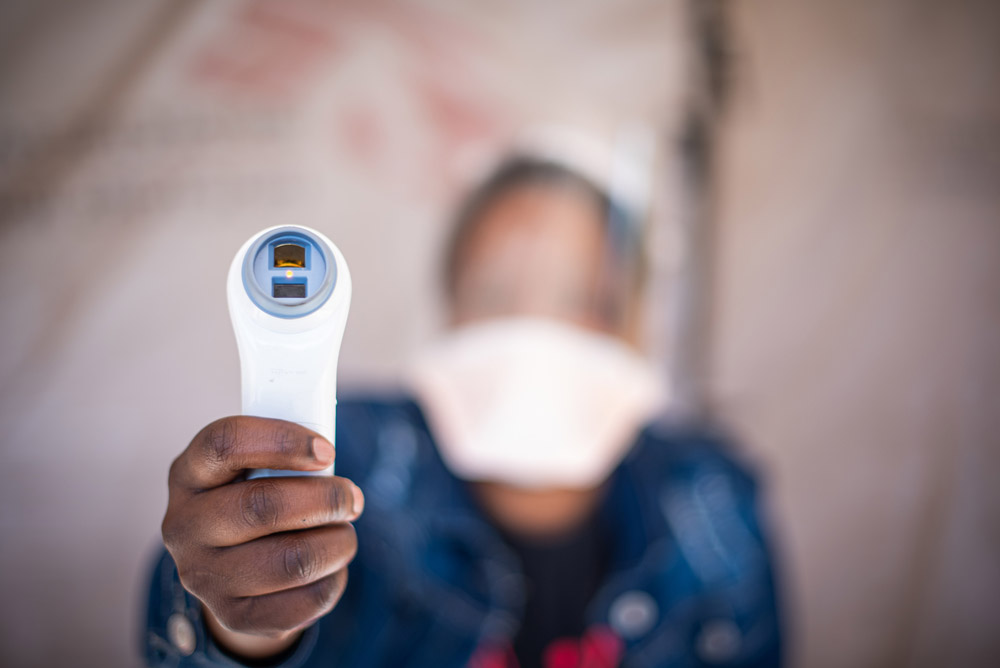
We’re concerned how people living in precarious environments will be affected by the pandemic. People living in overcrowded conditions, on the streets, in makeshift camps or substandard housing are at particular risk of COVID-19. Many are already in poor health and excluded from the formal healthcare system. We know social or physical distancing will be infinitely more difficult or impossible for these groups of people. We have to find other ways to help people keep themselves protected such as mass distributions of soap, water, and, in carefully considered circumstances, reusable cloth masks.