Medical careAs sexual and gender-based violence can occur anywhere at any time, MSF ensures that all of its projects are equipped to handle sexual violence cases.
However, in some countries, such as Colombia, Kenya and Democratic Republic of Congo, for example, we have projects that are set up specifically to provide treatment to victims of violence, including sexual violence. In these situations, we:
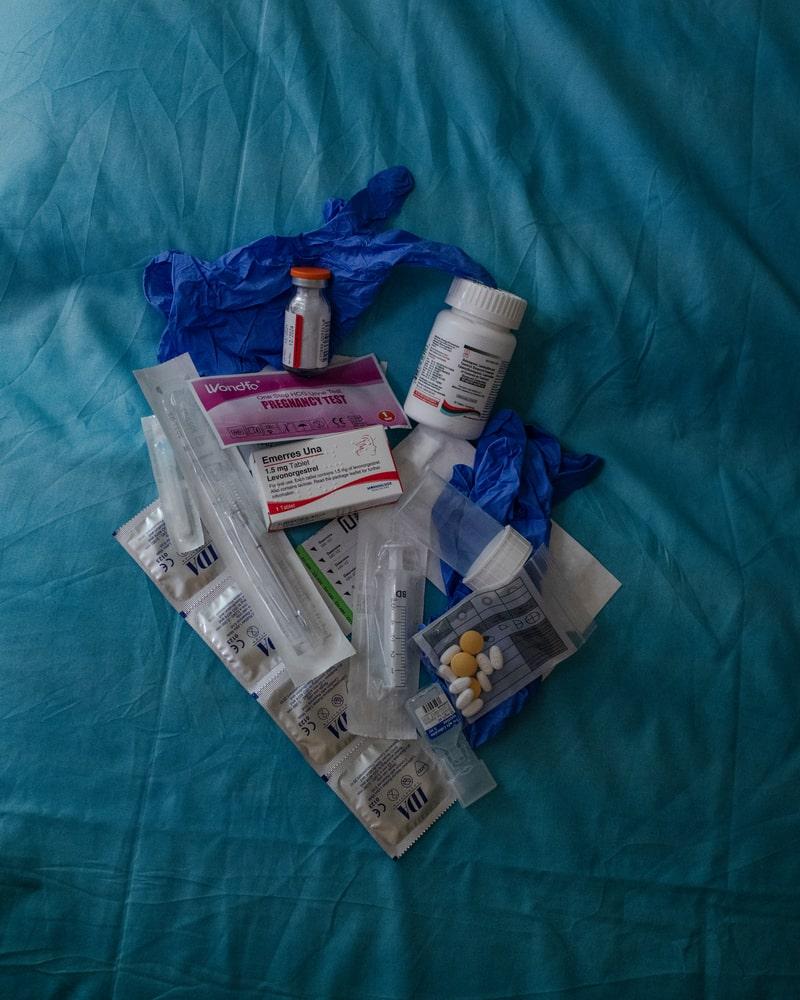
- Prevent against infection (HIV, STIs, Hepatitis B, Tetanus)
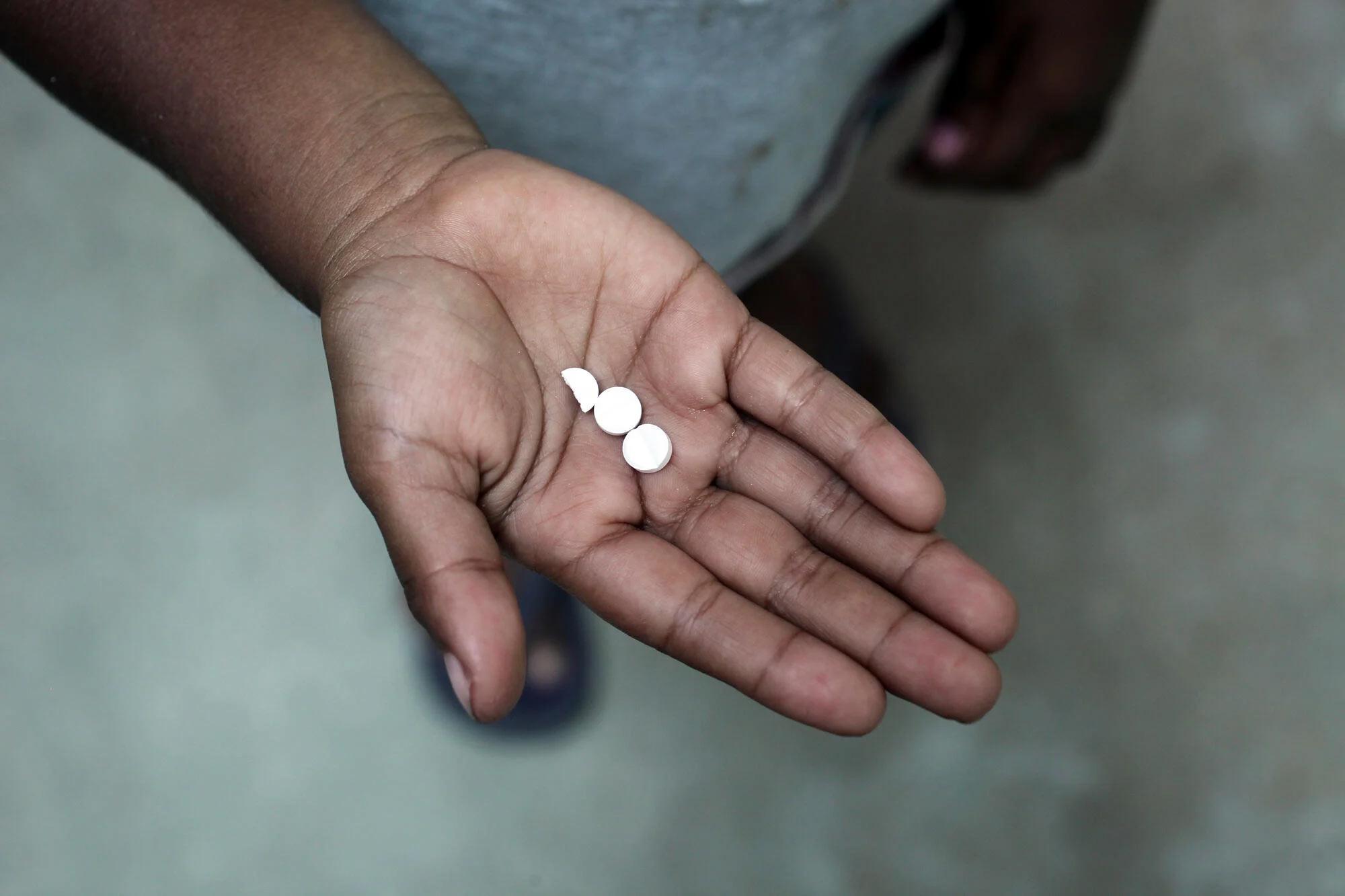
- Provide pregnancy tests and emergency contraceptives
- Help to manage unwanted pregnancies
- Provide psychological support
- Treat physical injuries
Our medics urge people to seek treatment within three days of an attack, to not only treat physical injuries but also to prevent disease.
Survivors of rape are given post-exposure prophylaxis to try and prevent possible infections, such as HIV. The sooner the drugs are given the more effective they are.
Antibiotics, vaccinations and emergency contraception can also be provided.
Psychological careAs well as treating physical injuries, MSF also provides psychological support to victims of sexual and gender-based violence.
We provide initial counselling to help patients deal with shock, as well as counselling and follow up care to prevent the development of post-traumatic stress.
Awareness and access to careMedical care is central to MSF’s response to sexual violence, but stigma and fear may prevent many victims from coming forward.
A proactive approach is necessary to raise awareness about the medical consequences of sexual violence and the availability of care.
Where MSF sees large numbers of victims – especially in areas of conflict – advocacy aims to raise awareness among local authorities, as well as the armed forces when they are involved in the assaults.