
Guinea
MSF has been responding to HIV/AIDS in Guinea for over 20 years. In 2024, one in four people living with HIV in the country received treatment at health centres in the capital, Conakry, where MSF provided direct care, training, and medication donations.
Providing HIV services within general health facilities allows us to both treat HIV as a chronic condition and integrate specialised care into the national health system. With this strategy, we also aim to reduce the stigmatisation around HIV, which is still strong. Many activists, both HIV-positive and -negative, support it, as it helps to combat the stereotypes surrounding the disease.
Our activities in 2024 in Guinea
Data and information from the International Activity Report 2024.
248
248
€8.9 M
8.9M
1984
1984
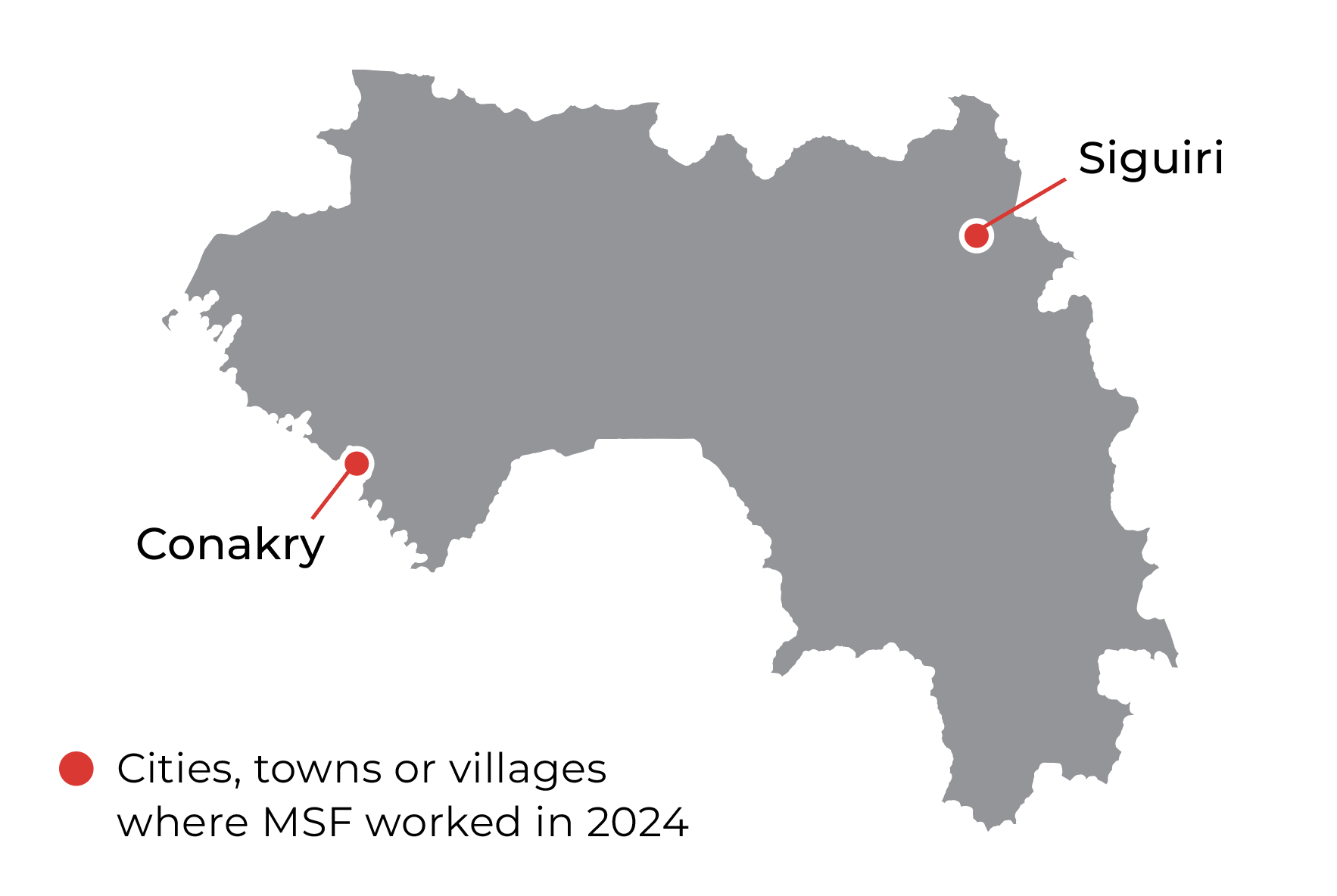
MSF collaborates with the Ministry of Health in nine health facilities in Conakry, supporting HIV testing and treatment, with a focus on prevention of mother-to-child transmission and paediatric HIV care, as well as treatment for opportunistic infections. In 2024, we increased our services for victims and survivors of sexual violence, including access to safe abortion care.
In addition, we manage a 31-bed facility at Donka hospital for people with severe complications of HIV.
Training is another important component of our project; we have trained over 300 medical staff in HIV care.
In Siguiri, in northern Guinea, MSF teams were involved in an emergency response to a diphtheria outbreak that started in August 2023. We supported treatment, referrals, and community awareness-raising campaigns – which led to a reduction in the deaths linked to the epidemic – until May.
IN 2024

17,600
17,6
13,400
13,4
2,707
2,707


Le VIH est dans mon sang, sa lutte est dans mon âme

Innocent Maniraruta: “Contributing to the invaluable mission of MSF”
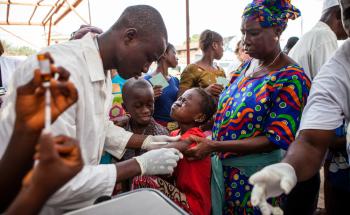
Guinea battling a large scale measles epidemic

The Politics of Fear
