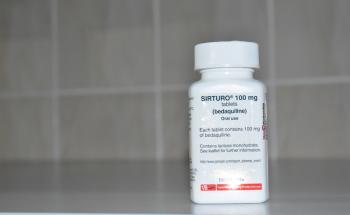

India
Our patients struggled with the high costs of private healthcare before diagnosis, and suffered stigma after receiving their diagnosis.
Working in collaboration with the Bihar State Health Mission and the Bihar State Department of Health and Family Welfare, we provided comprehensive, advanced HIV care at Guru Gobind Singh hospital in Patna.
Our Activities in India in 2024
Data and information from the International Activity Report 2024.
669
669
€15.2 M
15.2M
1999
1999
In Chhattisgarh state, despite an increase in violent clashes between government security forces and armed groups, we continued to run mobile clinics to deliver essential healthcare in remote areas, including safe abortion care. In 2024, we initiated a new mobile clinic in Hirmangunda, and collaborated with the Ministry of Health on a measles vaccination campaign following an outbreak.
In Manipur state, the situation remained unstable following an outbreak of inter-ethnic conflict in 2023, which posed challenges to the provision of care to our HIV and tuberculosis (TB) patients and to the transportation of supplies.
In Mizoram state, we offered healthcare to refugees fleeing violence in Myanmar. At our clinic in Zokhawthar, we organised specialist referrals and delivered care in the surrounding area. We also provided relief items to newly arrived families in displacement camps.
In Mumbai, we handed over our project treating complex cases of drug-resistant TB to India’s National TB Elimination Program and the Brihanmumbai Municipal Corporation at the end of 2024. Since 2006, this project has played a pivotal role in improving outcomes for patients who had no other treatment options.
In Jammu and Kashmir, where years of conflict have taken a toll on people’s mental health, we provided counselling services.

21,399
21,399
6,779
6,779
1,040
1,04
290
29

Kala Azar Explainer
Have you heard of kala azar?
KALA AZAR IS A NEGLECTED BUT POTENTIALLY FATAL TROPICAL DISEASE. INDIA ACCOUNTS FOR 30 PER CENT OF CASES WORLDWIDE. This short animation explains what kala azar is, how it relates to HIV, and what we are doing in response.
Since 80 per cent of India's kala azar cases are reported in Bihar, we set up a programme there in 2007.
People living with HIV are particularly vulnerable to kala azar, so since 2016 we have been focusing on treating patients co-infected with the two diseases, in partnership with the Rajendra Memorial Research Institute of Medical Sciences (RMRIMS) in Patna, Bihar.

Major opportunity to increase access to newer, safer DR-TB drugs is at risk

MSF responds to potential compromise on the ‘TRIPS Waiver’

ViiV will not license new game-changing long-acting HIV prevention drug to generic manufacturers

Letter: Launch of negotiations on TRIPS IP waiver at the WTO
