

Tajikistan
In Kulob district of the Khatlon region in southwestern Tajikistan, we continued our 'Zero TB' project, which is designed to demonstrate the feasibility of eliminating TB in geographically contained areas with appropriate treatment and preventive strategies.
Our holistic approach comprises social assistance, mental health support, and adherence counselling, as well as medical care, ensuring effective treatment. Our project uses advanced technology, such as digital x-rays, to facilitate early detection of the disease.
Our activities in 2024 in Tajikistan
Data and information from the International Activity Report 2024.
115
115
€3.1 M
3.1M
1997
1997
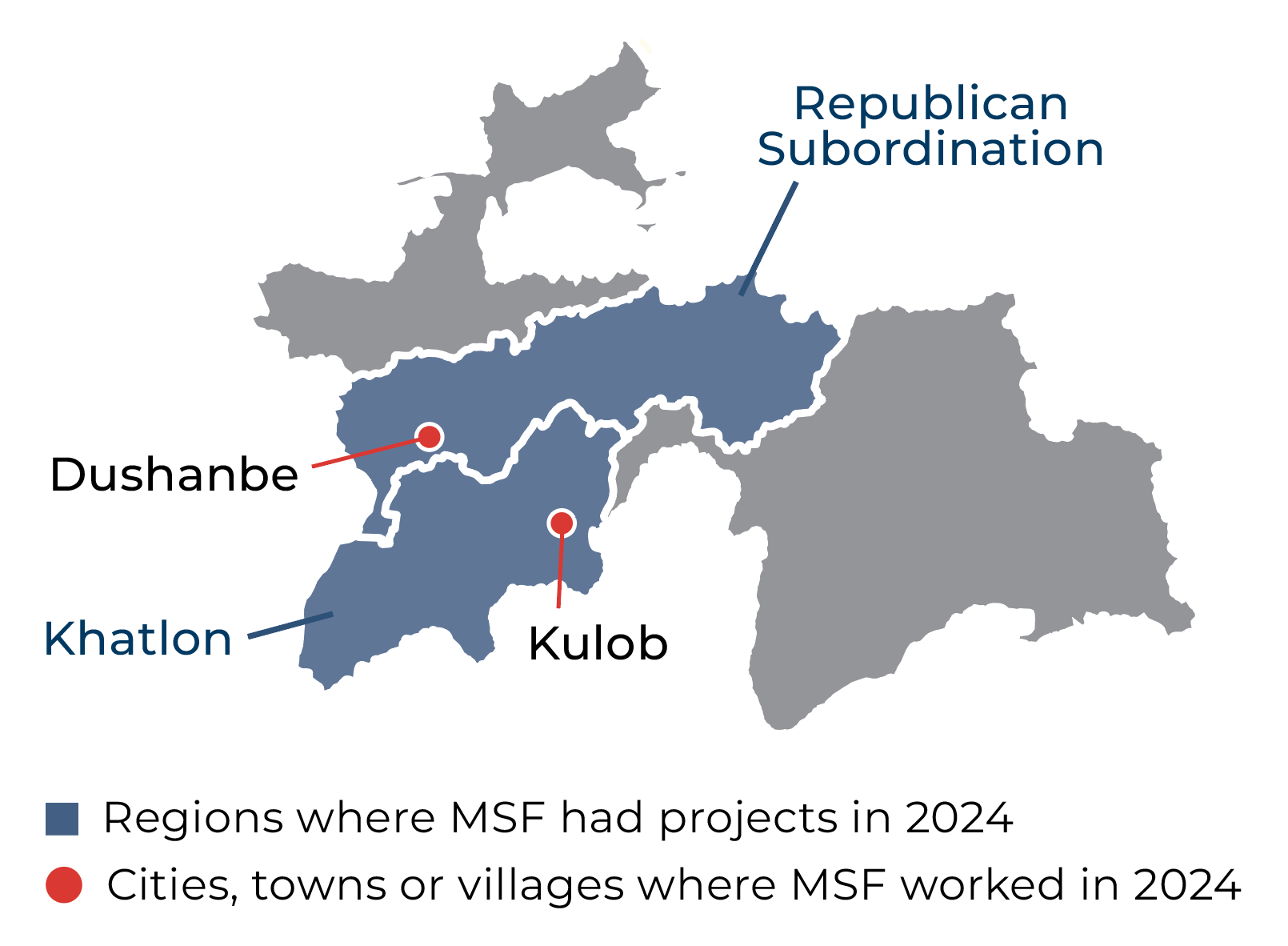
In June, we handed over our comprehensive TB care project in Dushanbe, which we had been running for 13 years, to the Ministry of Health and Social Protection of the Population. The project focused on improving TB detection, treatment, and support, especially for children and their adult family members, as well as the staff of and people incarcerated in prisons.
Through innovative methods such as F-DOT (family directly observed therapy), which allows patients to take their medication at home under the supervision of a family member, MSF empowered patients and involved the community in TB control.
During our time in Dushanbe, we achieved many milestones, including the introduction of better diagnostic tools and new medicines, such as bedaquiline and delamanid.
MSF continued to support the national TB programme and the Ministry of Health and Social Protection of the Population to implement shorter, all-oral treatment regimens for both drug-resistant and drug-sensitive TB, and initiated the first cohort of eligible patients in 2024.
IN 2024

11
11
