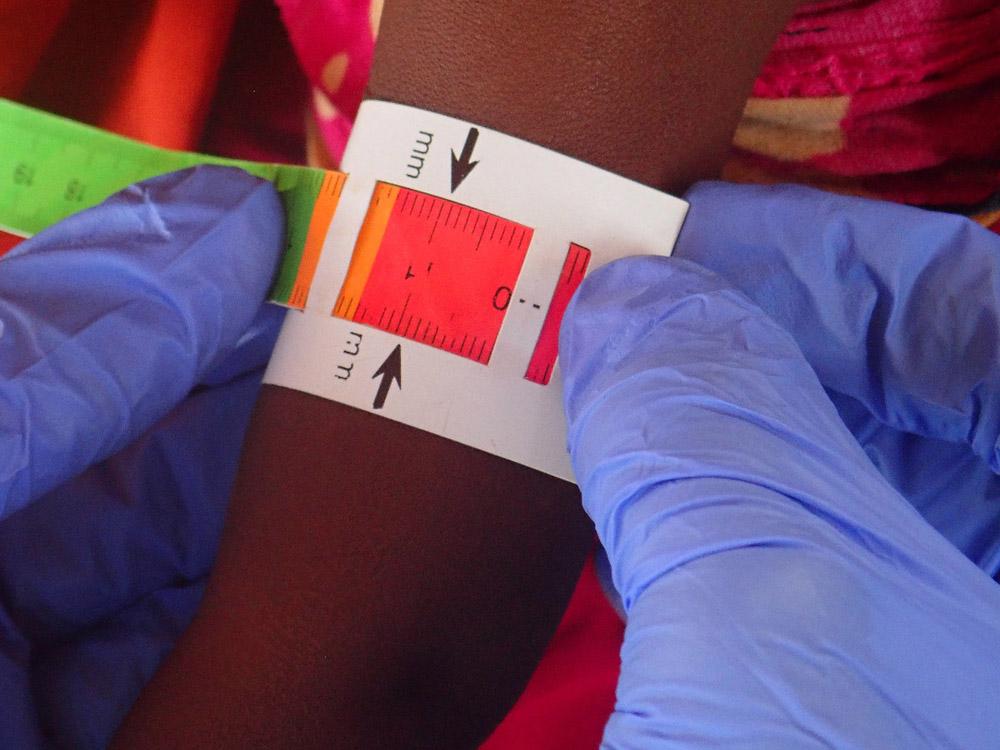
Increased rains seem to increase the number of people with vector- (insect) borne diseases, such as malaria and dengue fever. In Angumu health zone, Democratic Republic of Congo, malaria is the main cause of death among children under five. In recent years, our teams have observed what appears to be a trend of heavy rains and have treated a high number of malaria patients in the area. In 2018 and 2019 in Honduras, considered a climate change hotspot, we responded to the country’s worst outbreak of dengue fever in 50 years, following a prolonged rainy season.