
News and Resources
Publications
Here you'll find our annual activity reports, MAMELA – our donor magazine, our advocacy reports, opinion and analysis and other resources for those wanting to learn more about MSF.
Reports
Read reports on MSF’s operations saving lives across the world, in the most unimaginable conditions. Donate now to help us continue

Briefing Documents
View briefing documents compiled by MSF highlighting issues worldwide, such as: poverty, war and epidemics. Donate now to help fight these issues.
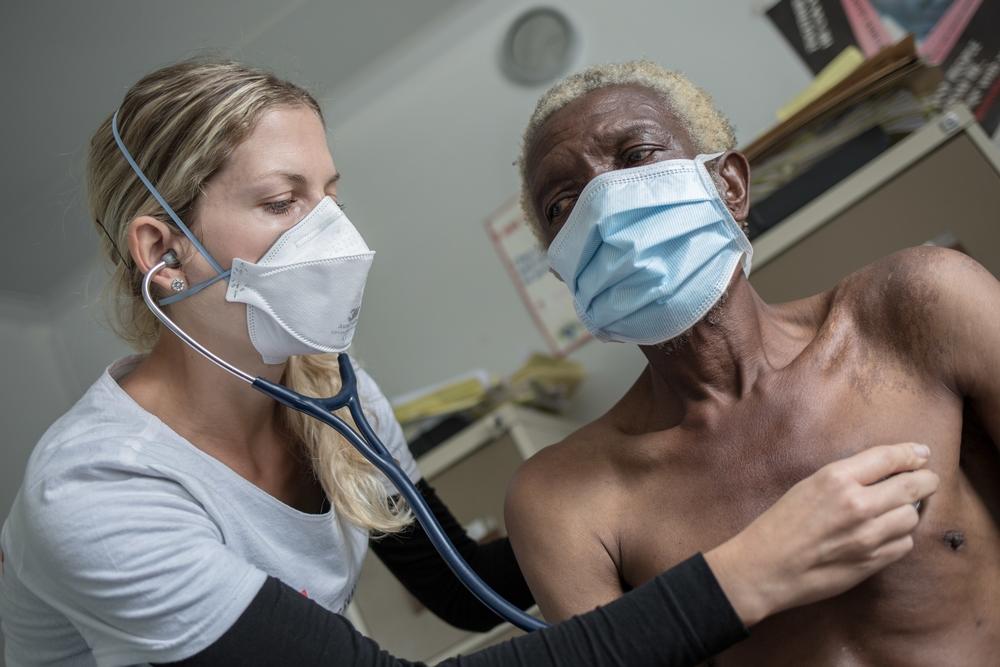
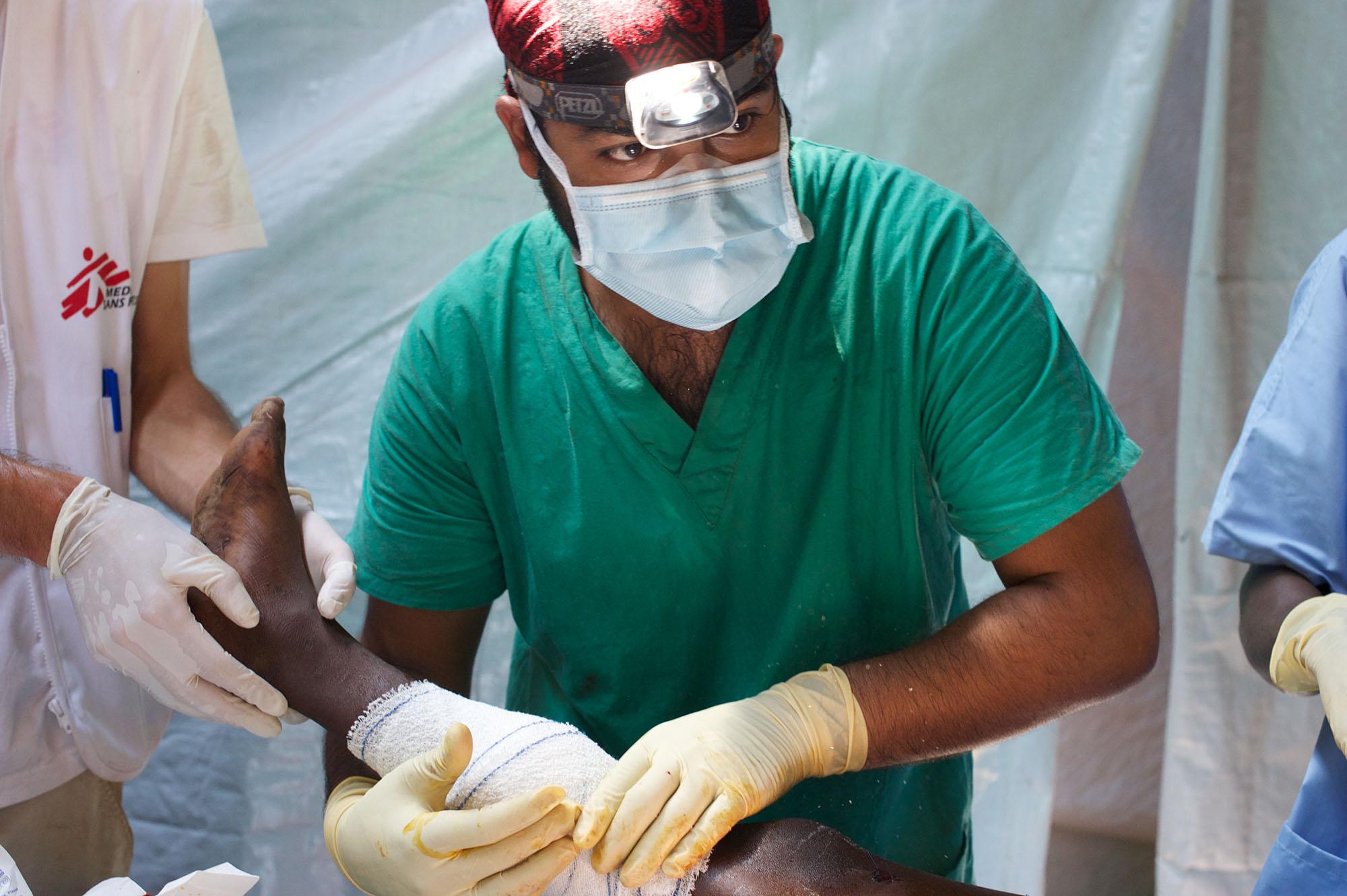
Opinions and Analysis
Read up on MSF's opinions and analysis of some of the worlds biggest issues.

Speech & Open Letter
Read up on MSF's open letters and speeches to companies and countries around the world. We keep up to date on all current events and always have our say.

Books
Read and purchase books written by MSF. Donate now to help us continue to save lives everyday.
