In the bustling emergency ward of Jahun General Hospital's maternity department, the rhythm of activity beats with urgency and determination, like a pulse in the air. In this hospital, Doctors Without Borders (MSF) collaborates with the Jigawa State Ministry of Health to provide comprehensive emergency obstetrics, newborn, and fistula care. Since commencing services in 2008, MSF teams have assisted 90,000 deliveries.
Nigeria is the third country in the world, after South Sudan and Chad, where a woman is most likely to die giving birth, according to the World Health Organisation. With an average of more than 1,000 maternal deaths per 100,000 live births each year, Nigeria is far from the global target for 2030 of less than 70 maternal deaths per 100,000 live births, as set under the UN Sustainable Development Goals.

Access to Maternal Healthcare in Nigeria
Maternal mortality rates far exceed the country average in northern Nigeria, where more than half of the country's estimated 200 million people live. In Jigawa state, the most significant factor is the limited access pregnant women have to antenatal care and delivery care for complications in childbirth, which frequently occur.
Unity Enuebuke, MSF Nursing Activity Manager, has been working in Jahun General Hospital for more than 10 years. “We see a lot of women with serious complications, with the most common ones being anaemia, haemorrhage and eclampsia,” she explains. The high number of patients means the maternity wards are often fully occupied, if not over capacity. Unity says, “We regularly have up to two women sharing a bed, and depending on the type of complications we see, things can escalate very quickly.”
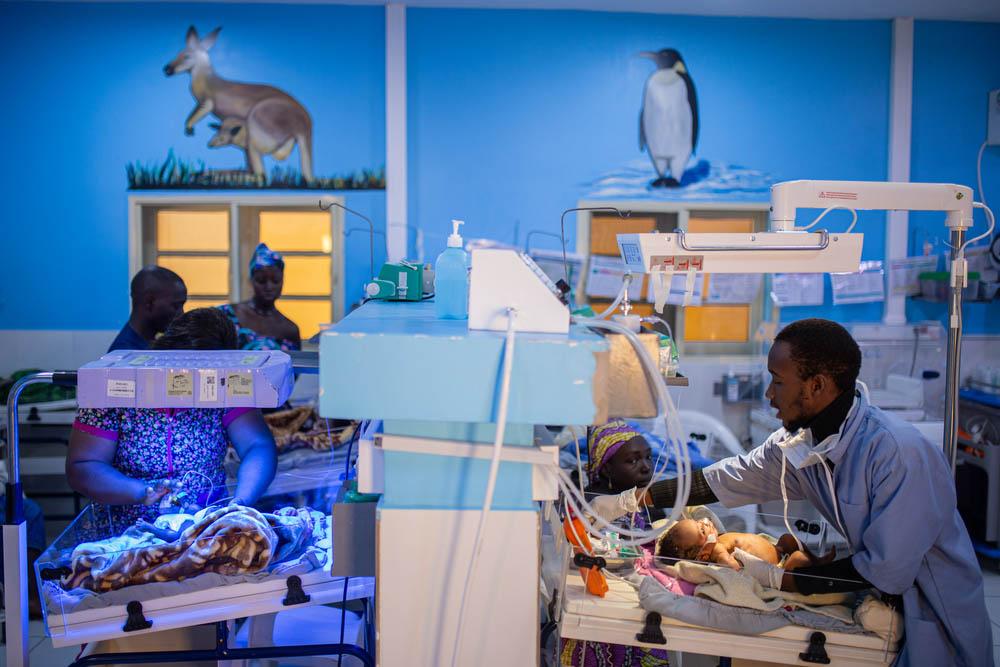
Ramatu
Ramatu, a mother of two, suffered life-threatening eclampsia—seizures due to high blood pressure—when she delivered her first baby in Jahun Hospital. This is her second time here, overcoming the considerable distance from home. “I live five hours away from Jahun General Hospital. There is no hospital where I live, and the closest one does not open at night,” she explains.
In Jigawa state, many of the estimated 749 primary healthcare centres do not have the drugs, healthcare workers, and medical equipment to serve the thousands of women of childbearing age. Despite efforts from public health authorities, the current healthcare infrastructure does not come close to meeting the needs of the population.

This dire situation leaves pregnant women who want to attend a healthcare facility with limited choices, such as giving birth at home and, if complications arise, embarking on a treacherous journey to try to reach one that is functioning.
It is also not enough that healthcare facilities are available; they must also be affordable. The economic reality in this region, worsened by soaring inflation rates, makes it difficult for people to afford hospital fees, drugs or even transportation to health facilities.
The result is that women become hesitant to go to the hospital, preferring to give birth at home with the help of more affordable traditional birth attendants, hence increasing the risk of experiencing complications.

Zainab's testimony
Khadijah
Women have given birth at home for centuries, but mothers’ and babies’ survival can hinge on preparing and planning for managing complications, which may also occur without warning. In Jigawa state, health professionals and facility-based delivery rates remain low, with up to around 80% of deliveries occurring at home.
Nurse Unity says, “Most times, family members don’t bring the mother to the hospital until they see that the baby is not coming out and the mother herself is having seizures.”
Khadijah, a 58-year-old traditional birth attendant in the Aujara community, Jigawa state, understands the value of hospital care if she can’t manage a complication but has experienced women’s hesitation firsthand. “Some women take my advice when I say they should go to the hospital, while some refuse to go to the hospital because they say that they are used to giving birth at home.”
In many communities in Jigawa state, pregnant women often require permission from their husbands or mothers-in-law to visit the hospital. This practice is compounded by a trend of early marriage at an age when women are not fully informed about pregnancy and are not physically ready to carry a child.
Khadijah explains that for some, “it is their husbands that prevent them from going to the hospital. Some men don’t see the relevance of antenatal care, while others don’t want another man to treat their wives.”
What needs to be done?
To tackle maternal mortality, a multitude of factors must be addressed. State authorities and international organisations must scale up their activities and increase funding to healthcare in the region, ensuring that budget allocations for primary healthcare centres are properly utilised and thorough planning and strict implementation processes are in place. In 2023, MSF teams assisted 15,754 deliveries, performed 1,911 caesarean sections and completed 43,785 antenatal consultations. Yet, it is still a drop in the ocean when looking at the needs of women in Jigawa state.
Primary healthcare facilities, which are often the first point where pregnant women seek healthcare, need to be equipped with trained personnel, equipment and resources to manage childbirth-related complications. “Eighty two percent of the cases we receive at Jahun General Hospital are complicated cases that could have been prevented at the primary healthcare level.” says Abdulwahab Mohamed, MSF medical coordinator. “Women, especially those of childbearing age, also have to be informed about their health and wellbeing through health empowerment programmes led by state authorities or other health stakeholders”.

Pregnant women must be encouraged to go for antenatal care, where they can be informed about their pregnancy journey and what to expect. Efforts must be made to mitigate cultural practices that hinder women from seeking care in medical facilities. Women should be allowed agency and freedom to make health decisions.
MSF supports the Jigawa state Ministry of Health in providing comprehensive emergency obstetrics and newborn care. Our support started with vesicovaginal fistula repair in 2008, however, the project evolved into a 161-bed facility to care for pregnant women and newborns experiencing complications. MSF teams also provide maternal and neonatal healthcare in the states of Kano, Benue, Cross River, Zamfara and will open a large maternity hospital in Maiduguri in June 2024.



