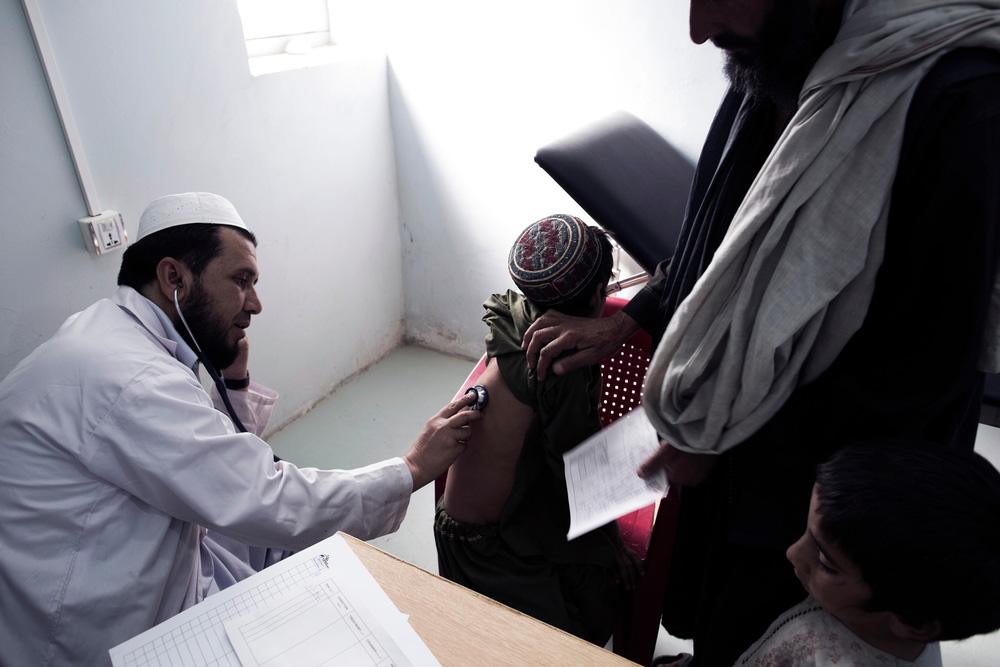
Throughout the year, our teams observed an overall increase in the number of individuals seeking care at our facilities. Although the security situation in the country has stabilised and people can more safely travel to reach healthcare, public hospitals and health centres are experiencing severe shortages of medications and staff. In addition, there are high levels of poverty and unemployment, and increasingly restrictive social policies designed to remove women from public and professional life. As a result, many people struggle to obtain the treatment they need.
The pressure on provincial and regional hospitals is intense. In 2024, MSF teams in Afghanistan reported very high bed occupancy rates, with two or even three patients sharing one bed in some facilities. Over the last three years, the number of patients treated by MSF has doubled.
Early in the year, we launched an emergency response to an unusually high seasonal measles peak in Balkh, Bamyan, Herat, and Helmand. In Herat, we expanded our isolation ward to admit more suspected cases. MSF also called on the government to increase access to vaccinations, for example, by reducing the age for the first dose from nine to six months.
The situation for women continued to worsen in 2024. In August, the Islamic Emirate of Afghanistan (IEA), also known as the Taliban, published a new law containing 35 articles detailing wide-ranging behaviour and lifestyle restrictions, mainly affecting women. The law formalised many existing restrictions and introduced new ones, such as forbidding women from speaking aloud in public.
Further reducing women's access to education, a process which began in 2022, the IEA banned women from studying at medical institutes, including nursing and midwifery schools, in December. Fifty per cent of MSF’s medical staff in Afghanistan are women, but we face ongoing challenges in recruiting gynaecologists in our maternity projects. We are committed to continuing our advocacy efforts and engaging with IEA officials to increase women’s access to medical education and education more broadly.
This year continued to see high numbers of Afghan returnees from Pakistan, Iran, Türkiye, and some European countries, and we conducted a series of needs assessments in some border areas.
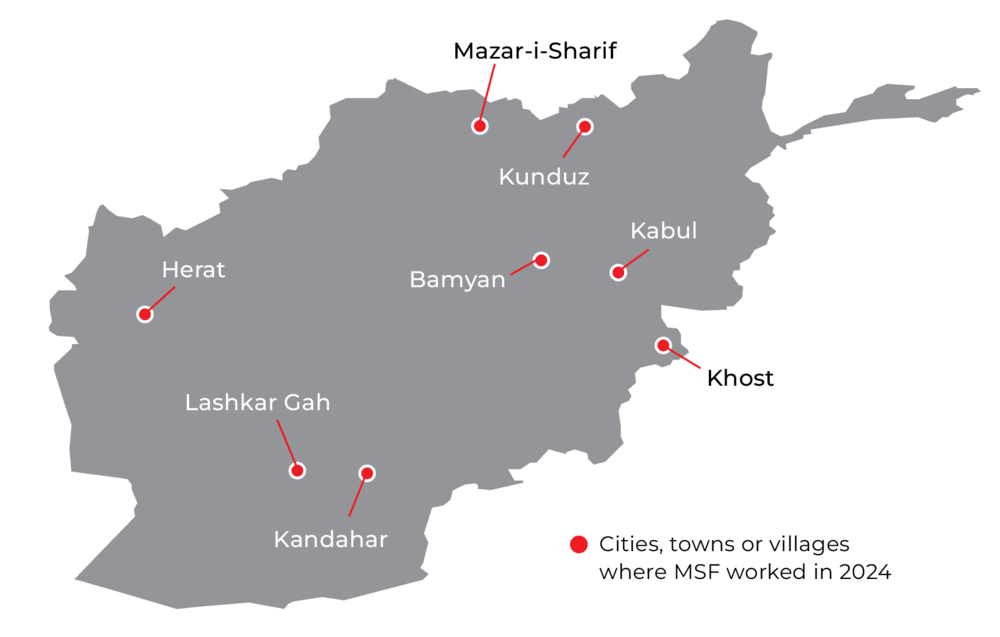
Balkh
MSF has been supporting Mazar-i-Sharif Regional Hospital in Balkh Province since August 2023, working alongside the Ministry of Public Health to reduce paediatric and neonatal mortality rates. Our teams work in the triage and emergency rooms, the neonatal ward and since May, the paediatric intensive care unit. We also supported a designated measles isolation ward in 2024.
Bamyan
Since December 2022, we have been operating a healthcare program in Bamyan Province. In collaboration with the community, we constructed and staffed eight health facilities in remote districts in the province between 2022 and 2023. We continue to support the facilities and staff by providing training, medical, and other supplies.
The MSF-supported facilities offer mother and child health services, including obstetric and gynaecological consultations, ante- and postnatal care, family planning, deliveries for uncomplicated pregnancies, and outpatient services. We also boosted the provincial hospital’s capacity to respond during the spring measles outbreak.
Helmand
MSF has been working alongside the Ministry of Public Health at Boost Provincial Hospital in Lashkar Gah City, Helmand Province, since 2009. The hospital is the main referral centre in Helmand, and for nearby facilities in the surrounding provinces.
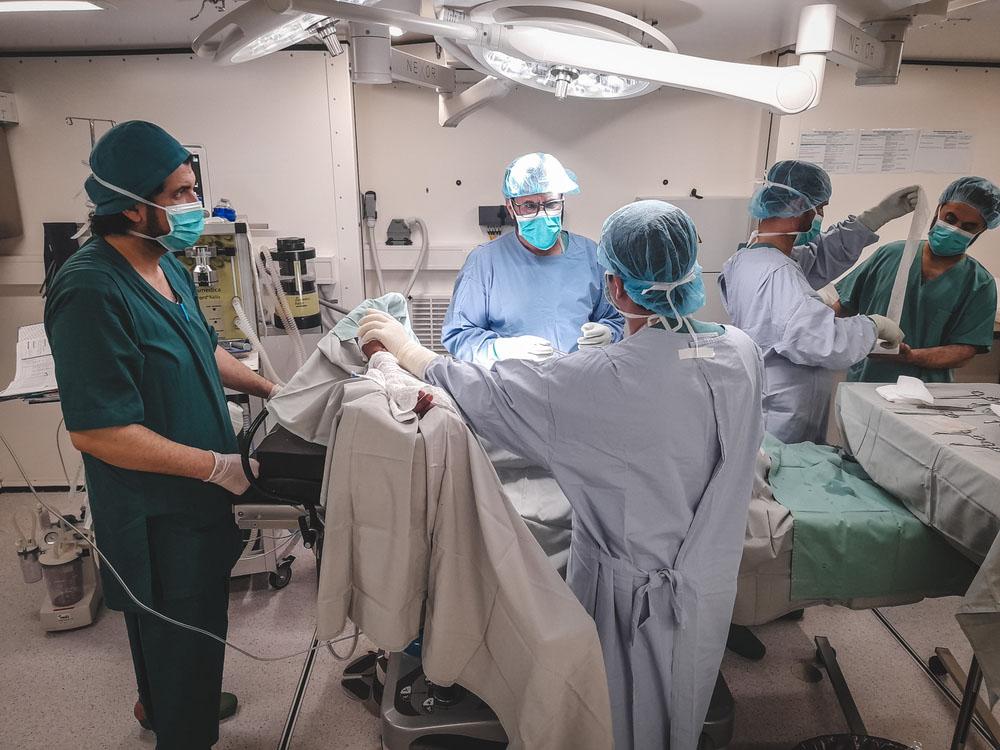
MSF works in nearly every department of the hospital, including the emergency department, paediatrics, neonatology, maternity, surgical services, internal medicine, and isolation wards. Each day, the emergency room sees between 800 and 1,000 patients, and the maternity department delivers around 75 babies. People continue to travel long distances to reach the facility due to the lack of free healthcare elsewhere.
Herat
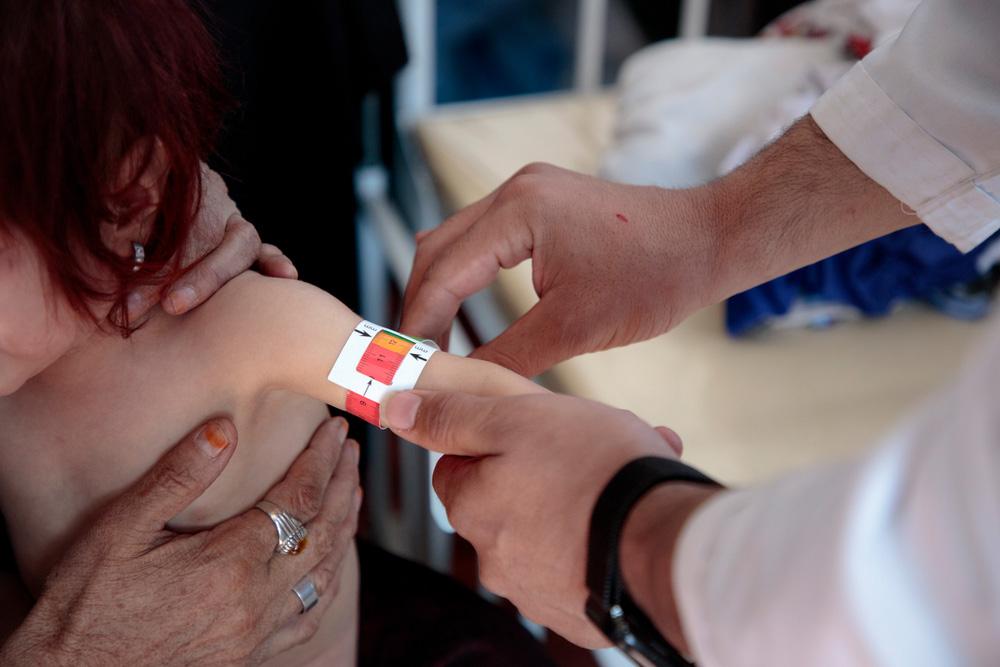
MSF also supports paediatric care at Herat Regional Hospital. We have teams working in triage, the emergency room, inpatient and outpatient therapeutic feeding centres, and the intensive and intermediate care units. In 2024, we opened a paediatric laboratory and started mental health activities to increase the connection between mothers and their children, and improve children’s cognitive and social development.
In October, we closed our Kahdestan outpatient clinic in the Injeel district to concentrate resources at the Herat Regional Hospital. We referred all patients with chronic non-communicable diseases to other organisations in the region.
Kabul
In Kabul, MSF provided financial support to the Afghan Midwives Association until the end of the year. Between January and April, we supported three facilities run by the Agency for Assistance and Development of Afghanistan, which treat children under six months old with malnutrition.
Kandahar
Since 2016, MSF has been treating patients with drug-resistant tuberculosis (TB) in Kandahar province, and supporting the detection and treatment of drug-sensitive TB in other facilities across southern Afghanistan.
We also provide nutrition programming through our inpatient and outpatient feeding centre.
Khost
In Khost province, our maternity hospital provides comprehensive emergency obstetric and neonatal care, with a focus on reducing high maternal death rates. We also offer financial support and training for staff in eight healthcare centres, to improve the capacity and accessibility of maternity services in Khost.
In May, we established a microbiology laboratory to strengthen our response to antimicrobial resistance in the maternity hospital.
Kunduz
MSF delivers trauma care in order to prevent avoidable deaths, illness, and disability at our dedicated trauma centre in Kunduz. We partner with Humanity & Inclusion to deliver physiotherapy services. MSF also runs a microbiology lab and has set up an antimicrobial stewardship programme to address the high burden of antimicrobial resistance in the province.
In Chahardara district, we run a health post, which stabilises injured patients and conducts outpatient consultations, screening for malnutrition, and routine vaccinations for children.
In May, when flash floods swept through Baghlan, Takhar, and Badakhshan provinces, MSF treated some of the wounded and donated over 100 trauma kits to Baghlan hospital.