The Syrian people endured nearly 14 years of war. While political developments brought significant changes to the country at the end of 2024, the humanitarian situation remained dire. Since the beginning of the war, over 14 million people have been displaced, and 16.7 million require humanitarian aid [1]. Many continue to live in precarious conditions, with little or no access to basic services and healthcare.
For many, the constant search for clean water, food, fuel, electricity, and heating has become a daily part of their lives. These issues are compounded by the country’s collapsing economy and drastic cuts in international financial support. The health sector is critically underfunded, and the likelihood of disease outbreaks and a further decline in public health remains high.
Northwest Syria
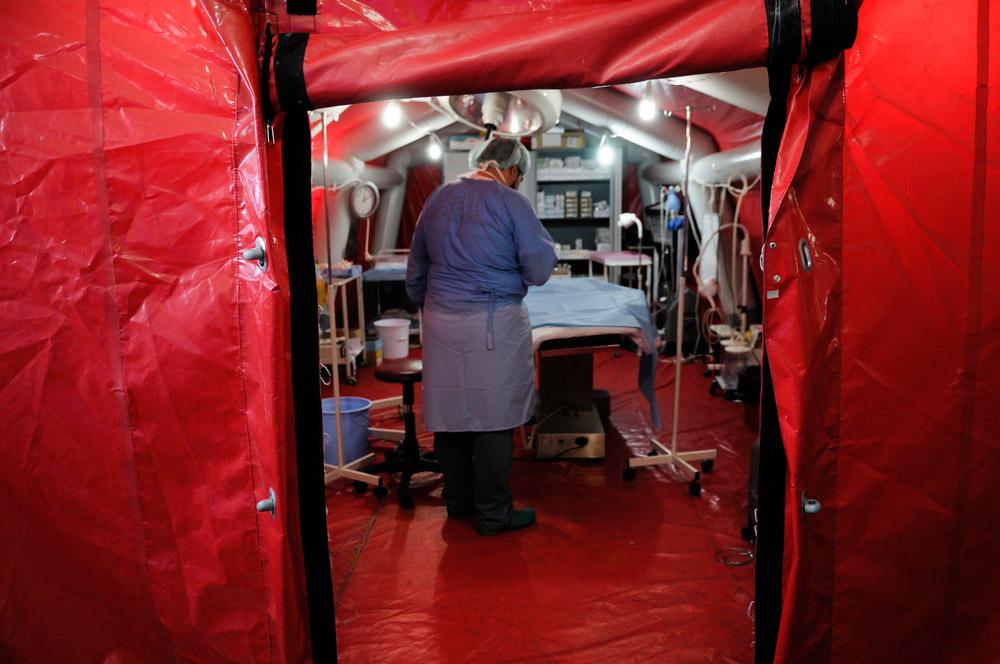
Chronic underfunding and conflict have eroded the healthcare system in the northwest of the country. There is a severe shortage of medical care, with hospitals and other health facilities forced to shut down or reduce services. Throughout the year, millions of people were still living in displacement camps in this region [2], in cramped, dire conditions, with scarce access to basic services, including medical care.
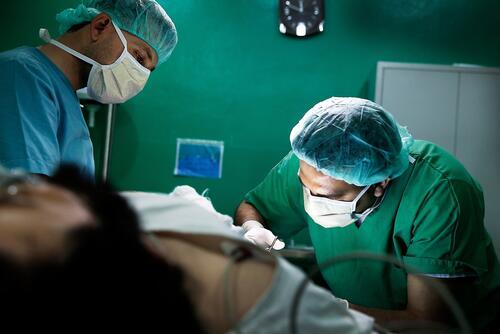
In 2024, MSF teams supported six hospitals, offering a range of medical services, including maternal and paediatric care, vaccinations, surgery, mental health support, and treatment for chronic diseases such as high blood pressure, diabetes, and skin conditions. We also continued to run our burns facility, where our multidisciplinary approach comprises surgery, mental health services, physiotherapy and palliative care.
In addition, we managed or supported 12 general healthcare centres, prioritising sexual and reproductive health and community health promotion, while our mobile clinics delivered essential medical services to displaced people across the region.
Northeast Syria
The communities in northeast Syria, including refugees and internally displaced people, face daily challenges in accessing healthcare and clean water. This situation was exacerbated by the failing economy and the destruction of key civilian infrastructure, such as water, electricity, and oil networks, by airstrikes during 2024.
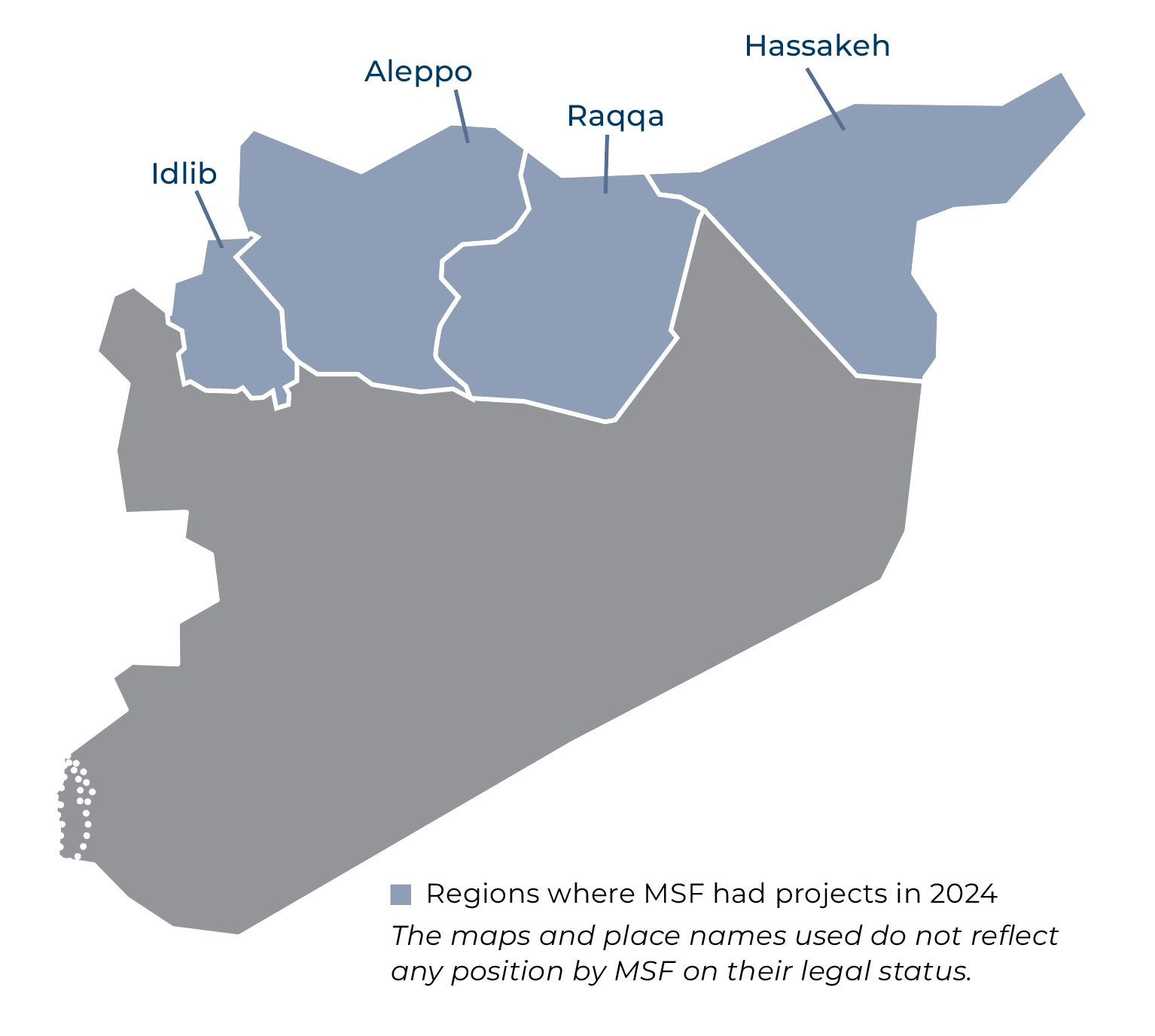
Throughout the year, MSF supported general healthcare clinics by offering treatment for people with non-communicable diseases, as well as mental health consultations and psychological support, through our projects in Al-Hol, Hassakeh, and Raqqa. Our teams also ran inpatient and outpatient therapeutic feeding centres, and supported an emergency room in Raqqa.
In Al-Hol camp, where approximately 40,000 people, mostly women and children, remain indefinitely and arbitrarily deprived of their liberty, MSF ran a mobile clinic and a health facility that provided basic health services, treatment for non-communicable diseases, sexual and reproductive health services, and home-based care for housebound patients. We also operated a water treatment plant to supply people with safe drinking water.
In late November, in response to new waves of displacement, MSF teams distributed essential supplies, such as hygiene kits, diapers, blankets, pillows, mattresses, and warm jackets, to 87 emergency shelters in Tabqa, Raqqa, and Hassakeh. We also improved access to clean water, including by trucking water, and enhanced sanitation by cleaning latrines in makeshift shelters.
[1] UNHCR - https://www.unrefugees.org/emergencies/syria/
[2] OCHA - https://www.unocha.org/publications/report/syrian-arab-republic/north-west-syria-situation-report-18-october-2024-enar