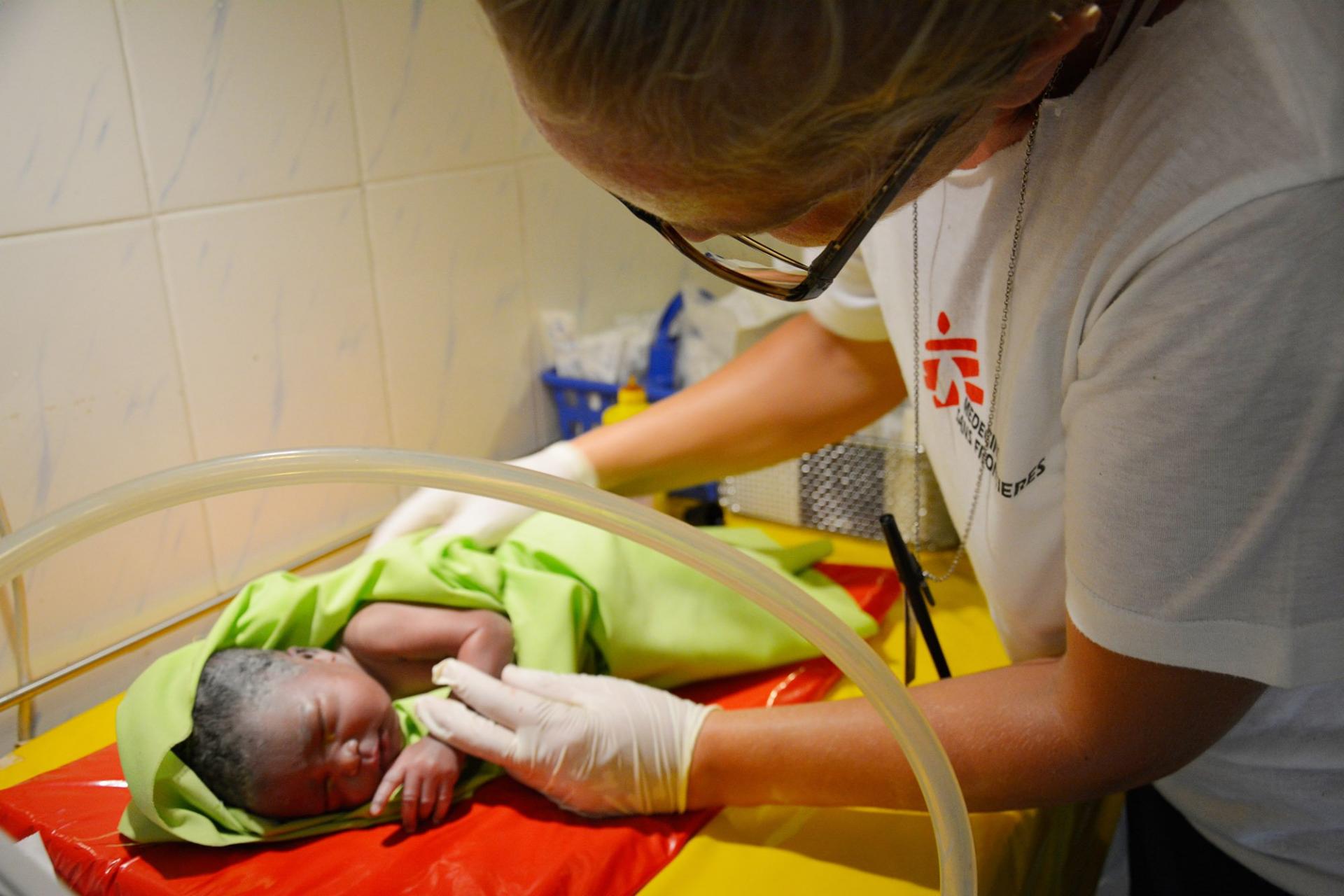
A Kenyan midwife completed her first MSF field assignment to Old Fangak, South Sudan. She shares the story of a patient she will never forget.

People may think giving birth is the same wherever you are in the world.
But not always in Old Fangak, South Sudan, where I recently worked as a midwife for Doctors Without Borders (MSF).
In most places, first-time mothers will come to the hospital early. But in Fangak, they arrive only when they’re fully dilated and ready to give birth, and want to leave straight after.
So even trying to get patients to stay an extra 24-48 hours to be monitored for complications is a challenge.
In Fangak, mothers-to-be also bring many people with them – usually a room full of aunts and grandmothers who help them through the birthing process.
And instead of laying on their backs to give birth, women prefer to kneel on the floor, squat down and then deliver their babies – not a common method seen in the western world, but quite similar to the way that Turkana women in my home country Kenya prefer to deliver their babies.
Patients in Old Fangak usually have to walk or row for kilometres to reach a health centre. It’s very remote, and there are no cars, just a few boats.

But despite the challenges, the women there are lucky in one sense: they are tall in stature, and their build has a hip and pelvic ratio that benefits them during childbirth.
In all my time there, most deliveries we did were easy natural births. There weren’t many complications that required us to do a caesarean section – which was good because culturally, the community dislikes C-sections and it’s often difficult to get families and patients to agree to the procedure.
But a C-section is sometimes the only option, as was the case with one 17-year-old first-time-mother I won’t forget.
She arrived at our health centre, 9 months pregnant with her first child, complaining of pain. Even though she was barely dilated and still had very far to go, we decided to admit her and monitor her labour.
It was during a routine physical examination that I noticed she had a limp. I did an assessment and realised it would probably affect her pelvis, making natural birth difficult.
When the patient went into labour, things progressed well at first, but when she reached time to deliver, she tried all she could to push but nothing was happening.

She was a first-time mother, and I wanted to give her more time so we waited and tried and tried. After 1 hour, I knew it wouldn’t happen naturally and we had to move.
I went out to tell the family that she would need to have a C-section. They were not pleased.
One of the aunts looked at me and said:‘You don’t look experienced, let us try’. (This happens to me sometimes. Because of how petite and young I look, many don’t believe I have 8 years’ experience as a midwife).
I had already informed my medical referent that we would need to prepare for a C-section. But I always think it’s better to work with the patient and their family, to help them understand our decisions and feel comfortable.
So I monitored the foetal heart rate, put a drip on the patient just in case, and said to the aunt: ‘okay, the floor is yours’.
Suddenly, a group of some 15 women – cousins and grandmothers and aunts – all filled the room, it was like a marketplace, all of them trying every means to get the patient to push.

After an hour of this, the aunt who had said I’m not experienced came back and told me: ‘We are done, we are also not experienced’. I then asked them: ‘Do we all agree that she needs to go for the Caesarean?’ and they agreed.
We took the patient in and in almost no time, she gave birth to a healthy baby boy – 2.8kg in size.
The mother was so grateful. She had noticed everything we did, and all the time spent trying to help her deliver normally, and she wanted to express her thanks.
So when the time came to name the baby, she said that since I’m called Judith, she will call him Jude.
A few months after, I left. But I’m glad knowing I left another Jude in Old Fangak.
Find out more about MSF's work in South Sudan.