- Overshadowed by outbreaks of Ebola last year and by COVID-19 today, the measles epidemic in DRC continues to kill children every day.
- With vaccination campaigns delayed and access to healthcare reduced because of measures to contain COVID-19, we are likely to see an increase in the spread and the death toll of measles and other major killer diseases.
- MSF teams are responding to COVID-19 in DRC while continuing to vaccinate and provide care to children in areas most affected by the measles epidemic.
“It's going to be lively!” warns Héritier, before starting up his motorcycle on the sandy track between Lisala and Boso Manzi, in Democratic Republic of Congo’s northern province of Mongala. “It hasn't rained for a while, and with so much sand, getting there is going to be tough.”
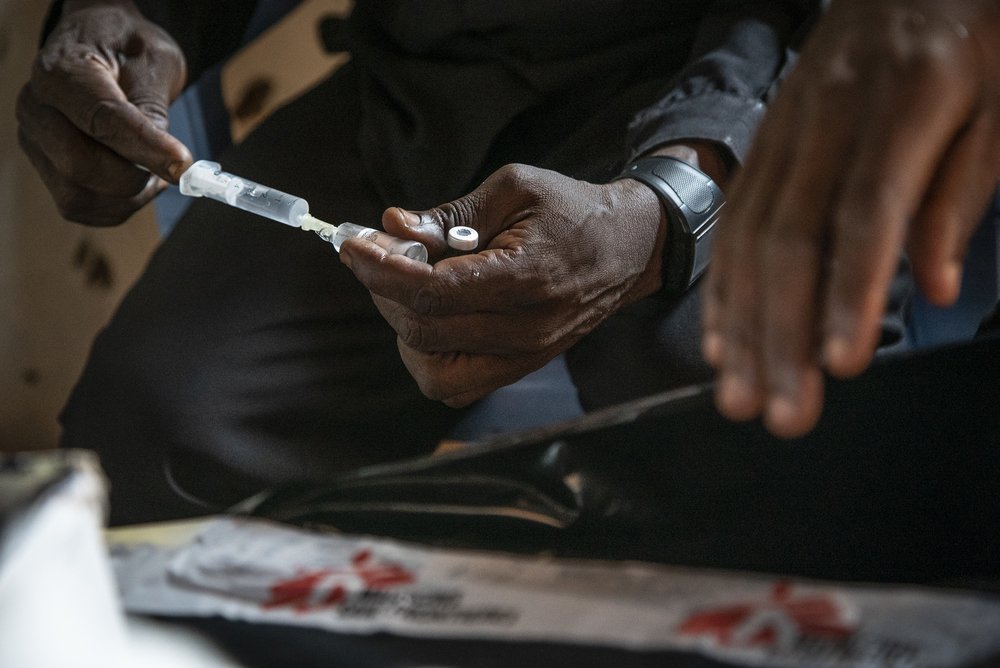
Like the convoy of MSF bikers behind him, Héritier is carrying a big box full of ice packs, filled with one of the most vital medical items in this area: measles vaccines.

Measles in the Central African Republic
Mongala province has been hit hard by the measles epidemic that has spread across DRC over the past year, killing more than 6,600 children since January 2019. Despite a vaccination campaign carried out by the Ministry of Health and World Health Organization (WHO) in this area last December, there have been hundreds of measles cases in Boso Manzi health zone since early 2020. This prompted MSF to send an emergency team in February to assess the needs, begin a new vaccination campaign and support the provision of care.
Every delay fuels the outbreak
Overshadowed by the Ebola outbreak in the east of the country, the measles response has been neglected from the start. It took months before the epidemic was finally declared in June 2019, while the vaccination campaigns organised by authorities were marked by delays, coordination issues and a lack of supporting partners, many of whom were focused on the response to Ebola. A supplementary vaccination campaign, intended to 'mop up’ those children who had been missed, was repeatedly postponed, before finally taking place in late 2019.
All of these factors contributed to the disease’s heavy toll in DRC, making it the country’s deadliest measles epidemic recorded to date and the largest in the world today.
“Today, the overall number of cases may have reduced, but the epidemic is far from over,” says Emmanuel Lampaert, MSF operations coordinator in DRC. “Some areas are even reporting increases and there are about 100 health zones where action is urgently needed. Since January, more than 50,000 cases and 600 deaths have already been officially notified. But many zones with increasing numbers of cases and deaths are not included in the latest national measles response plan.”

In this already difficult context, the COVID-19 pandemic has created extra barriers to vaccinating children against the disease.
“Implementing preventive measures to reduce the spread of COVID-19 is vital to protect communities and health workers, especially in a country like DRC where the health system is very limited,” says Lampaert. “Unfortunately, these measures are having an impact on the overall measles response, including transporting vaccines, assembling dedicated teams and launching vaccination campaigns.”
These obstacles are affecting the efforts to bring the measles epidemic under control, says Lampaert. “Every delay and every obstacle increases the risk of the epidemic continuing to spread, killing more children. The same happened during the West African Ebola outbreak, when measles vaccination activities were disrupted, leading to a resurgence of the disease.”
“The needs here are huge”
On the road to Boso Manzi, people cheer the arrival of the motorbike convoy after its six-hour drive. As in many remote places in DRC, local people know all too well the toll taken by ’silent killers’ such as measles, malaria, diarrhoea and respiratory infections.
“The needs here are huge but the supply of medicines to health centres is problematic,” says Gédéon Mushadi, the health zone’s chief doctor. “The few medicines available in the health facilities do not cover the needs.”
Alphonsine Ekima, 43, and her family have felt the direct impact of this. Six weeks ago, her three-year-old daughter Marie died of measles. She was buried on the same day as her cousin, who died from the same disease. “Marie was the fourth child taken away from me,” says Alphonsine.
Like Alphonsine, Mada Mado’s child also died of measles a few weeks ago, while her other children all have symptoms of the disease. “My six other children have all been infected, even though they were vaccinated last December,” she says.
The lack of protection afforded by this vaccination does not surprise Dr Philippe Mpabenda, coordinator of MSF’s 6-week emergency response that started in February. “The effectiveness of the vaccine depends on it being kept at a temperature of 2 to 8 degrees Celsius until the injection,” he says. “But in hard-to-reach areas like this, local health centres don't have cold chain capacity to keep vaccines refrigerated. They also lack transportation. As a result, vaccinations are often concentrated in the immediate vicinity of the health centres and don’t reach those children living in more remote communities.”

Measles and beyond
At Boso Manzi general hospital, where MSF is supporting care for measles patients, the impact of the epidemic is striking. In the dedicated measles ward, sick children, accompanied by their mothers, occupy the many beds.
In the middle of the room, Dobo Mambanza, aged three, lies groaning in her mother’s arms. Her face is blotchy from the disease and she struggles to open her mouth. Her mother travelled 65 km by motorbike to reach the hospital after traditional treatments failed to cure the early symptoms.
“Measles weakens the immune system and makes children vulnerable to many other infections, leading to respiratory, neurological and ocular complications as well as malnutrition,” explains MSF doctor Patrizia Giangrande, as she examines the little girl. “Unfortunately, because of her eye infection and the damage to her cornea, Dobo will not be able to see again.”
Next to her, three-year-old Mbisa Eme Kosenge, is also battling the disease. As well as measles, she has contracted tuberculosis and is showing signs of malnutrition. But after 10 days of hospital care, she will soon be able to return to her family in their village 55 km away.
“We are chasing the hotspots”
MSF has treated more than 1,000 patients like Dobo and Mbisa at Boso Manzi hospital during its 6-week emergency response. Beyond the hospital, MSF has vaccinated 44,000 children across the health zone.
“We chasing the hotspots,” says Dr Mpabenda. “Last month, our team was in Equateur province and in a few weeks we’ll be deployed in another area. That’s the reality of the epidemic at this stage.”
From Haut-Uélé to Kongo Central, from North Ubangi to South Kivu, MSF teams have already been deployed in a dozen provinces across DRC in 2020; this year they have already vaccinated more than 260,000 children against measles while caring for more than 17,500 that already had the disease. Last year, MSF vaccinated 816,000 children against measles and cared for more than 50,000 patients with the disease.

Today, with all eyes focused on the threat of COVID-19, MSF teams are continuing to respond to other health emergencies such as measles, in DRC and beyond.
“As we adapt our approach to the coronavirus pandemic and support the response to it, it is important to remember that a one-track focus on COVID-19 will sow the seeds of other major health crises,” says Lampaert. “Reducing vaccinations, nutrition support or malaria prevention in the face of a public health crisis will lead to other crises, making the situation even worse. Neglecting the other health issues would make us complicit in many more future deaths.”
