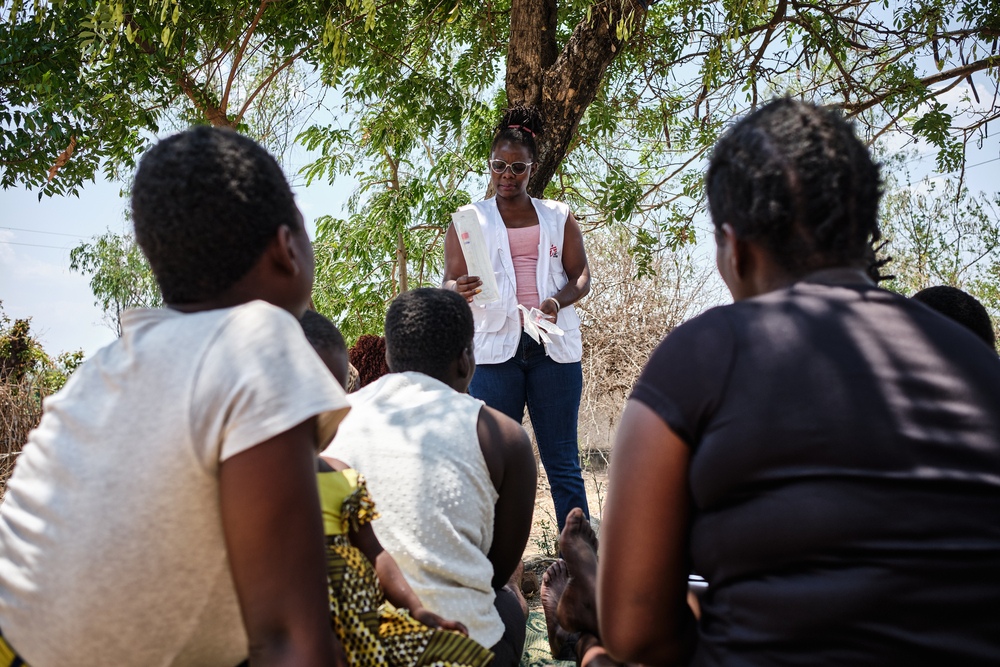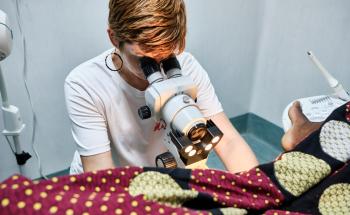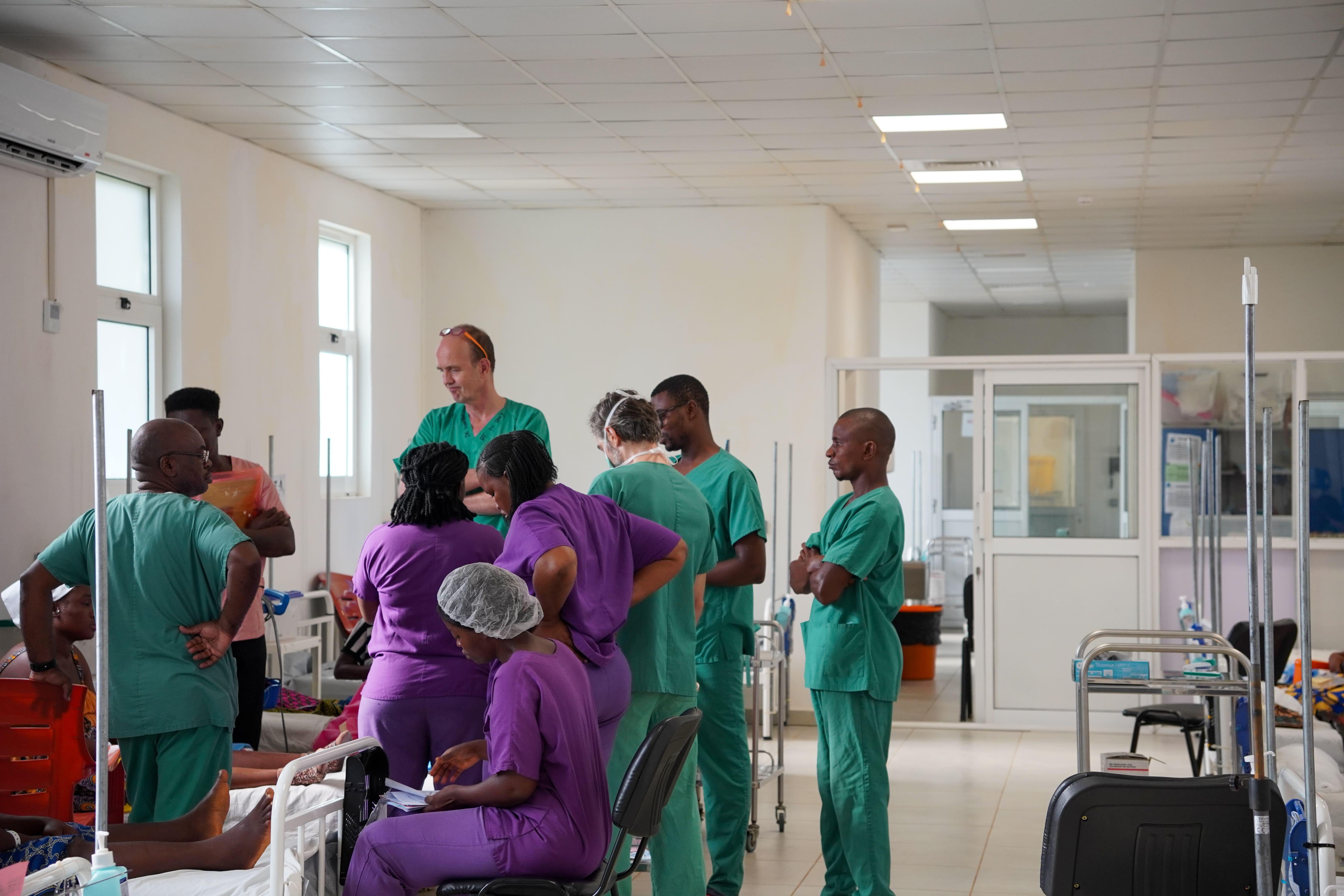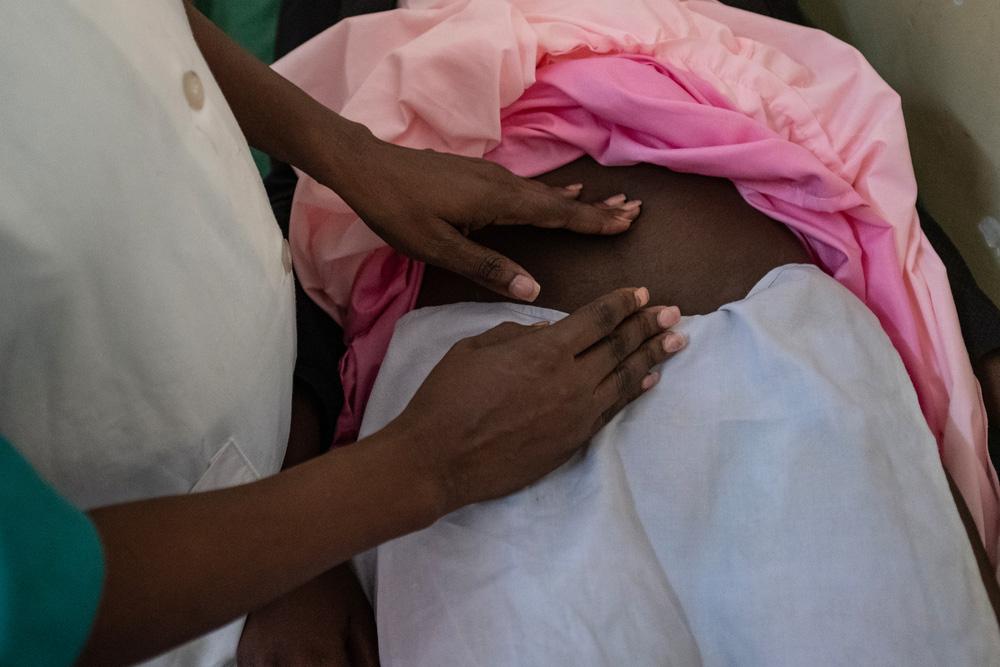
Maternal mortality
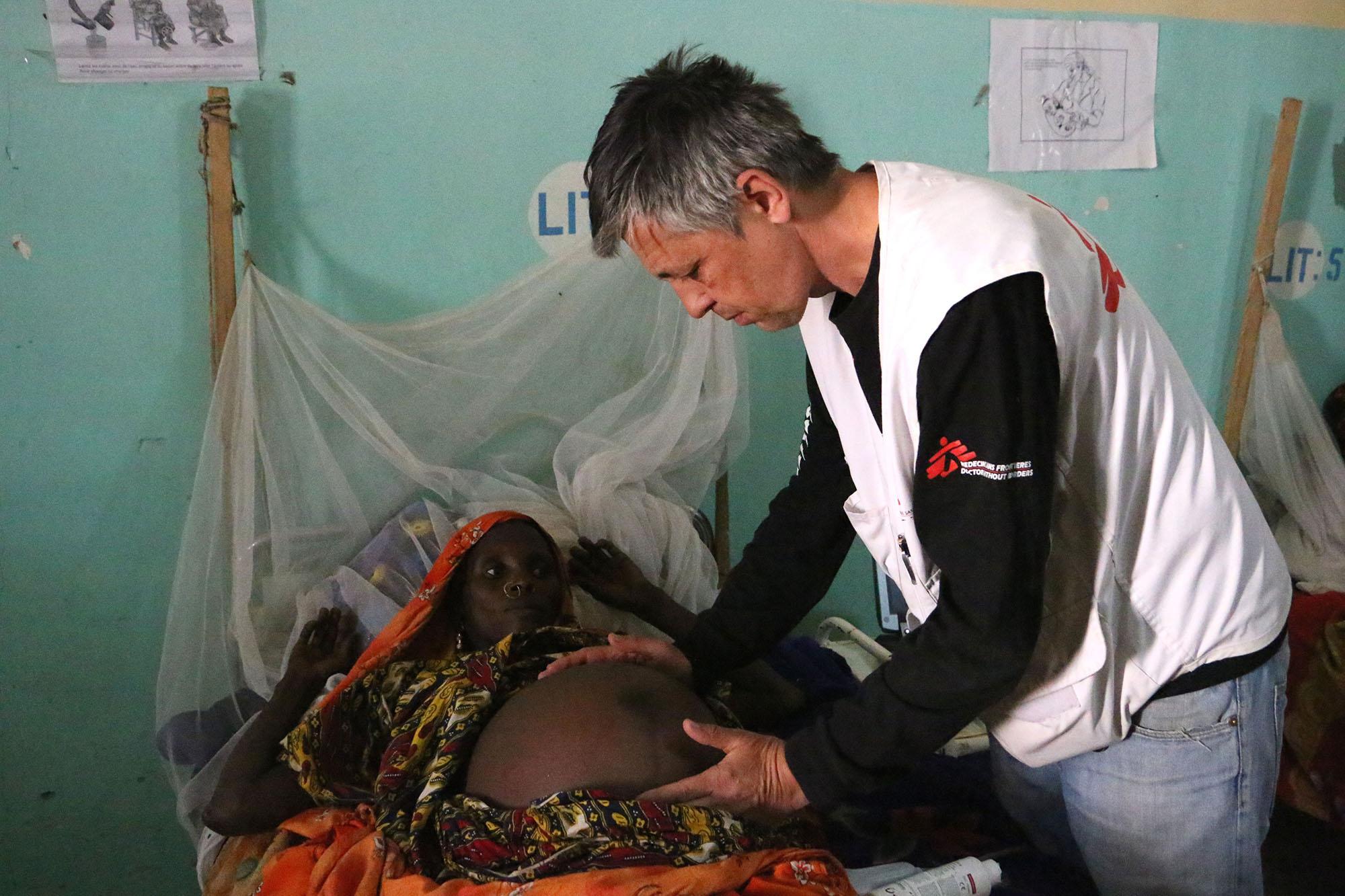
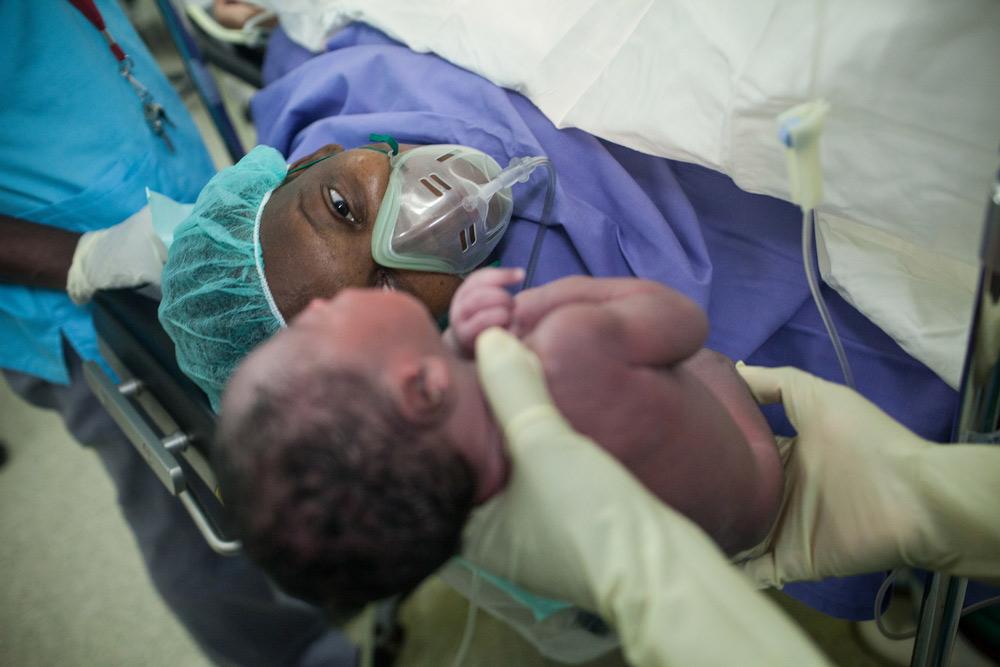
Half of all maternal deaths occur during or within 24 hours of delivery. Common causes of maternal death include postpartum hemorrhage, reproductive tract infections, eclampsia, complications from unsafe abortion practices, obstructed labor, and serious infectious diseases. Serious, untreated complications during pregnancy or delivery can be fatal to both mother and infant.
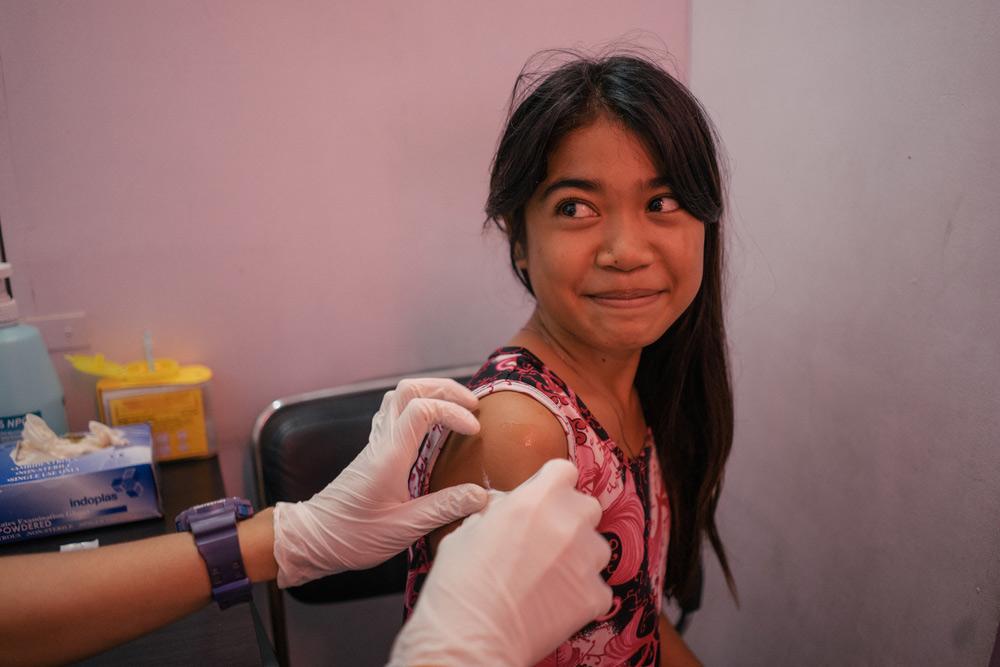
Maternal health care is vital to reduce maternal mortality and suffering, and it includes access to safe abortion care. Unsafe abortion is the only main cause of maternal death that is almost entirely preventable.
Emergency obstetric care is a key component of MSF’s strategy to reduce maternal mortality, and its rapid implementation is incorporated in our response to crises such as conflicts or natural disasters.