

Mozambique
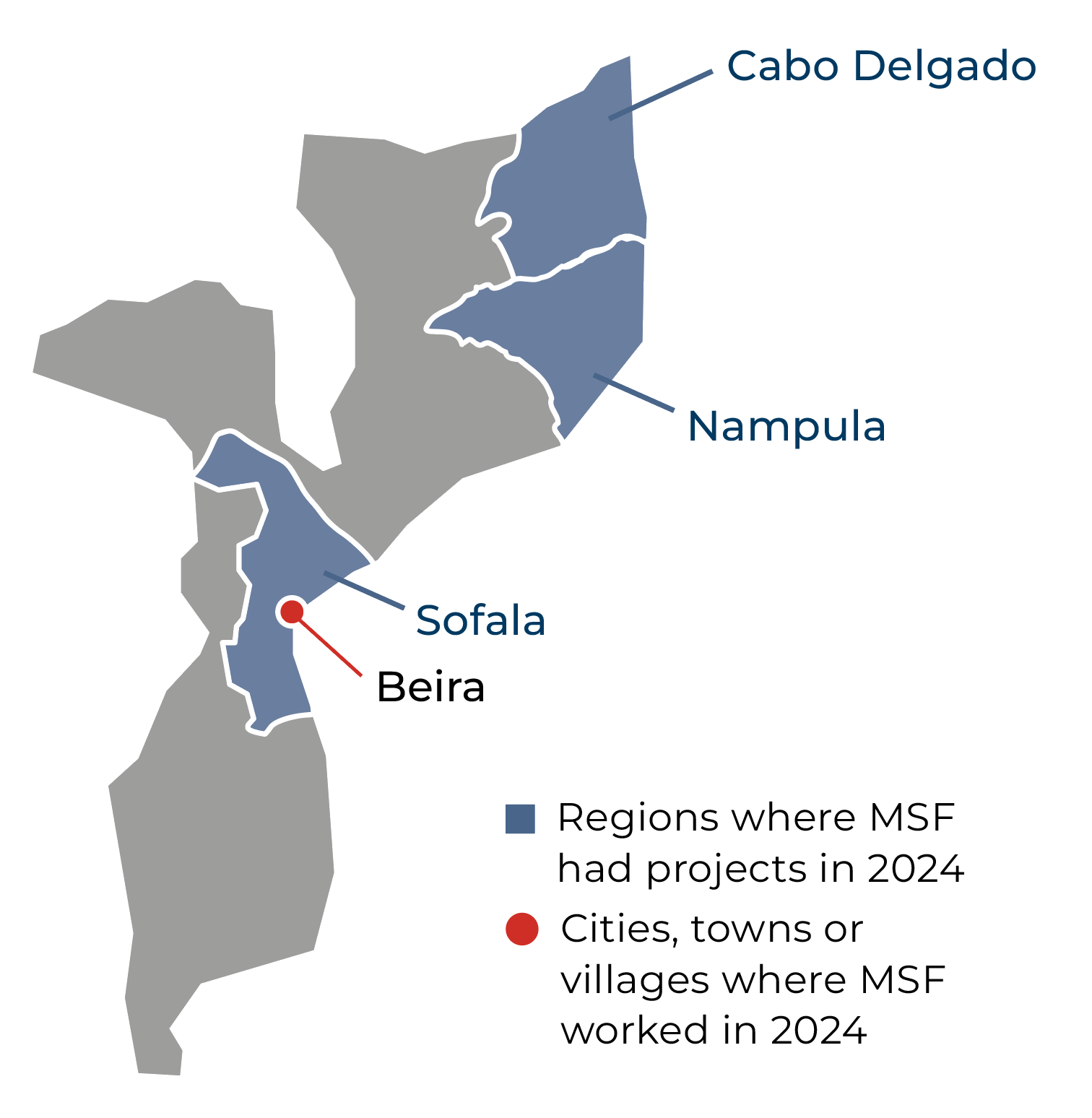
In Cabo Delgado province, where about 580,000 people remained displaced due to ongoing conflict and unrest, our teams continued to provide healthcare through community-based activities and support to health facilities in the districts of Palma, Mocímboa da Praia, Macomia, Mueda, Muidumbe, and Nangade.
In May, Macomia was attacked by an armed group; MSF’s warehouse was looted, and our cars stolen. This attack and the increased insecurity forced us to suspend our work in Macomia town, temporarily cease running our mobile clinics and outreach activities in the district, and reduce some services in other areas of Cabo Delgado.
Featured
Our Activities in Mozambique in 2024
Data and information from the International Activity Report 2024.
834
834
€22.5 M
22.5M
1984
1984
In December, we launched an emergency response in the Mecúfi and Nanlia districts of northern Mozambique, following the devastation caused by Cyclone Chido, which affected over 680,000 people. Our response focused on providing lifesaving emergency healthcare, mental health support, rehabilitating damaged health facilities, and restoring essential water, sanitation, and hygiene services.
In Nampula province, MSF teams diagnosed and treated neglected tropical diseases (NTDs) at rural health centres, and provided blood transfusions for people suffering from severe malaria. In November, we launched a surgery campaign in Nametil to assist patients with hydrocele, a complication of filariasis, an NTD which causes an abnormal accumulation of fluid in the testicles. We performed surgical activities during the first weeks of the month; however, we had to suspend all activities in Nametil by the end of November due to escalating security incidents.
In Sofala province, our team in Beira worked with the Ministry of Health and local organisations to deliver sexual and reproductive healthcare, including safe abortion care for vulnerable and stigmatised groups, treatment for people with advanced HIV, and support for addressing antimicrobial resistance.

201,100
201,1
6,010
6,01
133,000
133,
369
369


MSF demands sustained investments and political will to end the neglect of children with tuberculosis

MSF winds down operations in Mueda following transition to local health authorities

Lessons learned reaching key and vulnerable populations

MSF launches emergency response as violence drives over 100,000 people from their homes in northern Mozambique

