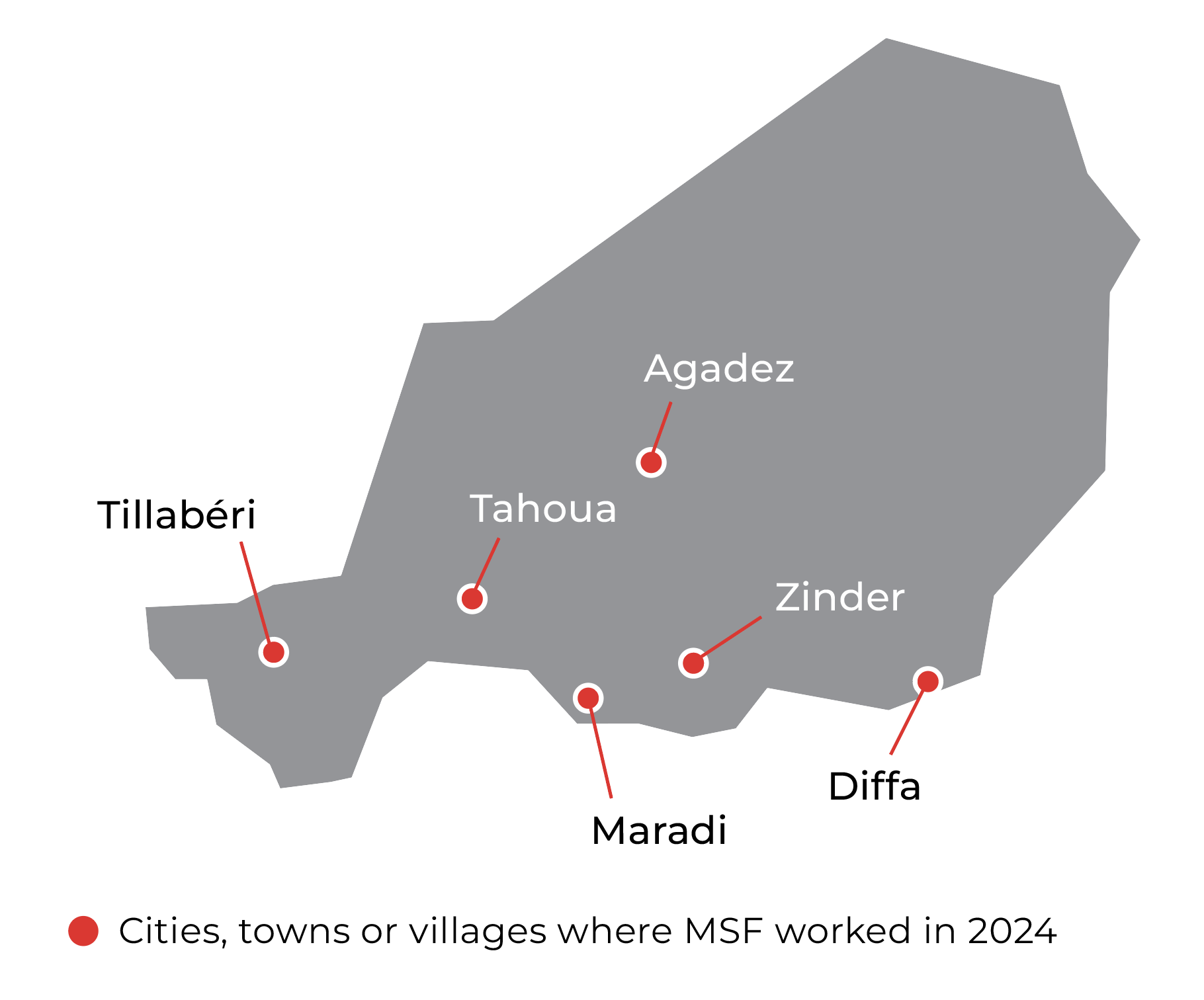
In 2024, border closures, insecurity, and other challenges continued to disrupt supply chains, including for medicines and nutrition products in Niger. Despite these obstacles, our teams treated an increased number of children in the facilities we support in the Maradi, Zinder, Tahoua, and Diffa regions between June and November—the so-called lean season, when rainfall is heaviest and food stocks are depleted.
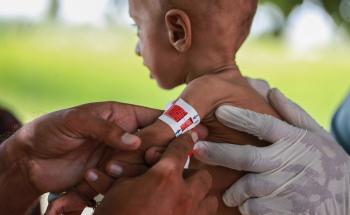
To further address the situation, in Magaria, we carried out an indoor residual spraying campaign in partnership with the national malaria control programme in 25 villages, aiming to curb the proliferation of mosquitoes, which transmit malaria. Meanwhile, in Madarounfa, we hired an additional 200 healthcare workers to cope with the influx of malnourished and sick children. Additionally, in Diffa, we collaborated with local health authorities to open 40 community-based healthcare sites to treat malaria, and referred patients requiring further care to the hospitals we support in Diffa and Nguigmi.
People in the Tillabéri region have extremely limited access to healthcare and other essential services, due to armed violence and forced displacement. In addition to our general healthcare in Torodi, our teams supported the hospital in Téra and four other health facilities, including Banibangou health centre, where we set up an operating theatre. Through 28 community-based healthcare sites, we supported in bringing care for malaria, respiratory infections, and diarrhoea, closer to home.
MSF continued to assist people migrating through Agadez, many of whom had been expelled from Algeria and left stranded in the desert. Our teams provided mental health support along migration routes, facilitated protection referrals for vulnerable people, and continued advocating for the dignity and security of migrants. We also ran search and rescue activities in the desert and distributed relief items such as hygiene kits and blankets.