Sierra Leone
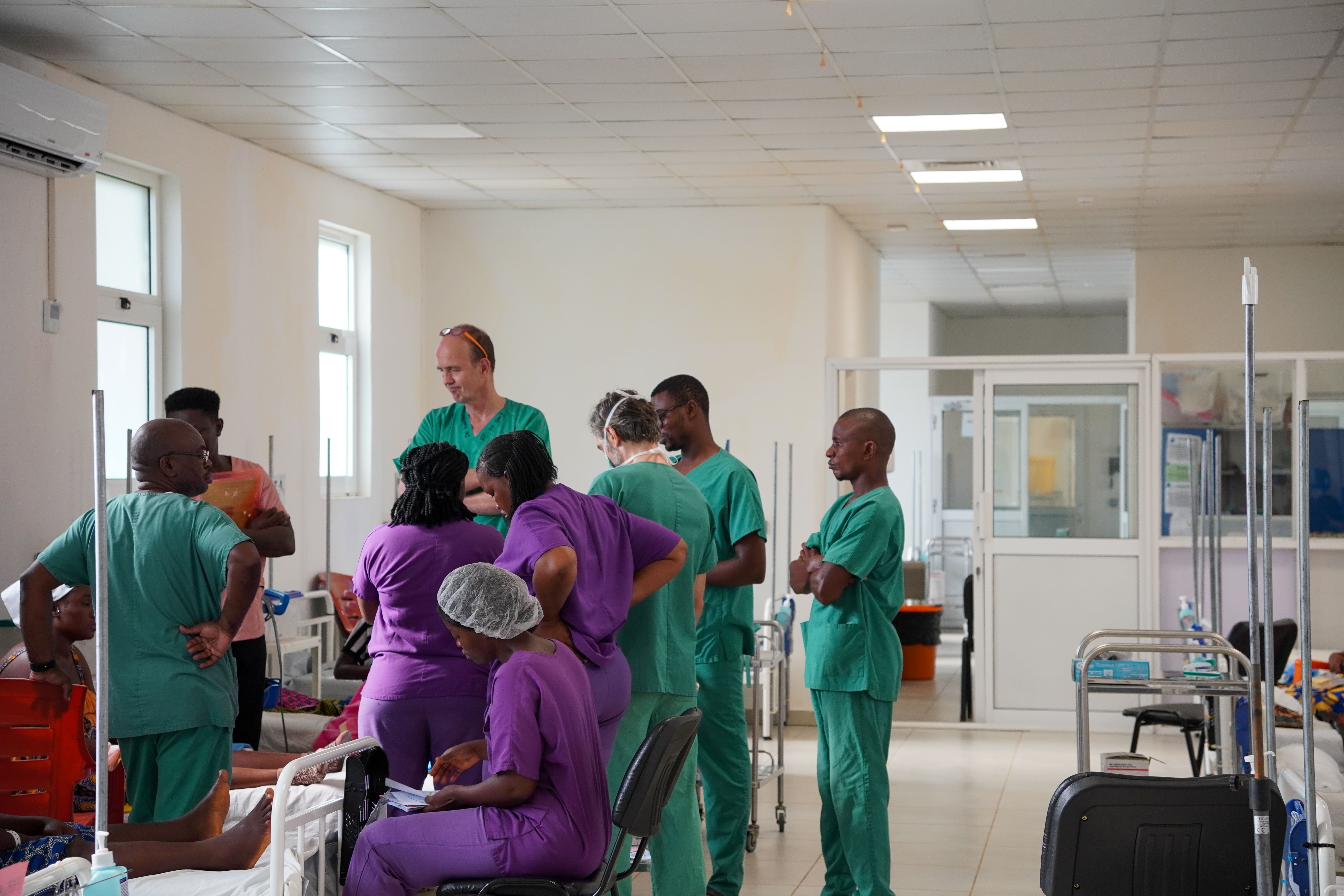
In Kenema district, Eastern province, pregnant women, lactating mothers, and children under the age of five receive lifesaving medical care in the 164-bed mother and child hospital built by MSF.
In addition, we run mobile clinics to serve communities living in remote villages where no healthcare is available.
Featured
Our activities in Sierra Leone in 2024
Data and information from the International Activity Report 2024.
1,283
1,283
€22 M
22M
1986
1986
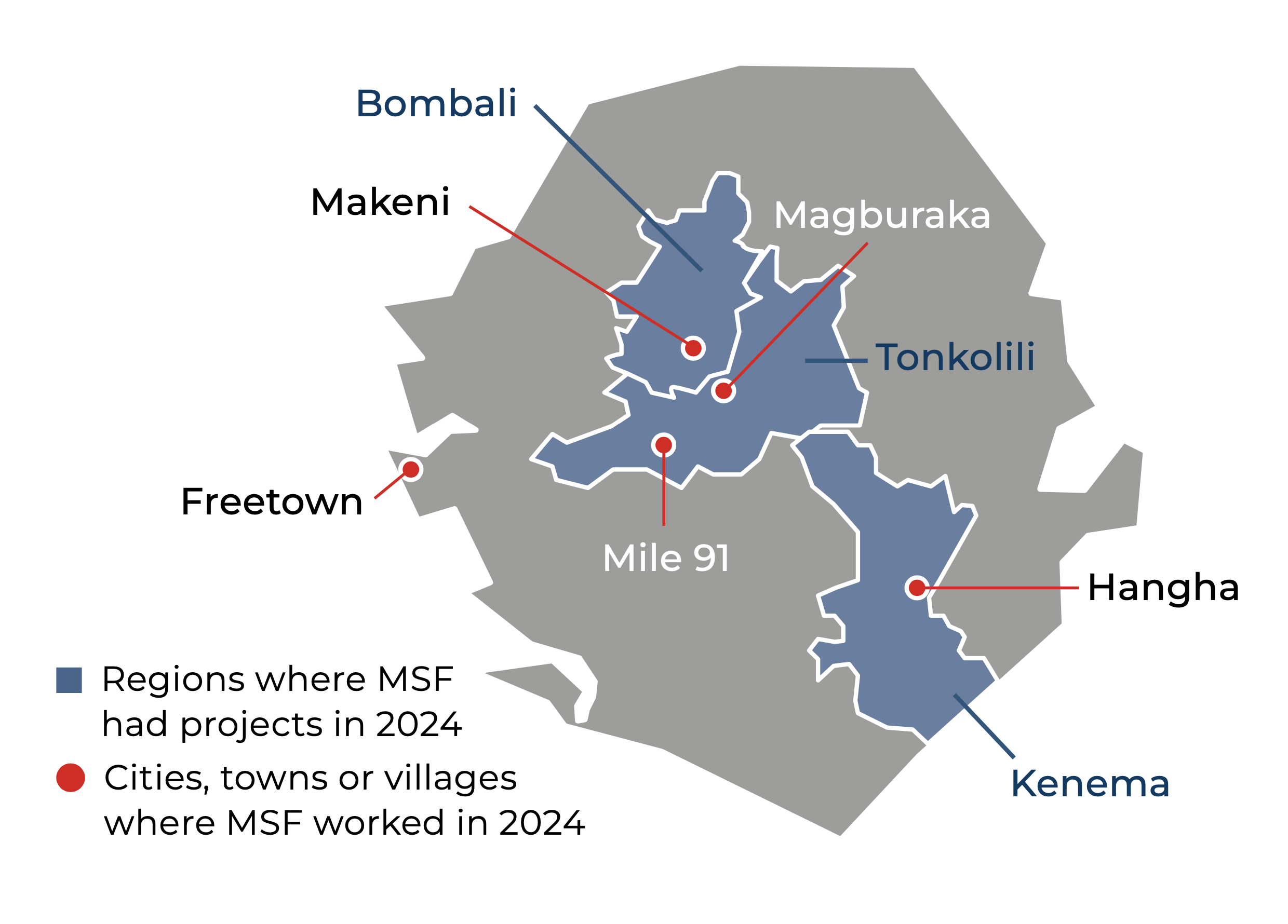
In 2024, our teams provided rapid malaria testing and treatment, vaccinations for children under five years old, family planning, antenatal care, and referrals to specialist facilities. We also supported six general healthcare facilities in the district by donating medical supplies, renovating buildings, and training Ministry of Health medical staff.
In Tonkolili district, Northern province, our teams continued to support 12 healthcare facilities by supplying medicines, completing rehabilitation work, providing water and sanitation services, and training medical staff. With our support, we aimed to reduce maternal and child deaths in Mile 91, Magburaka town, and the surrounding villages. We also drilled seven boreholes in the district to ensure that people have safe drinking water.
In Magburaka government hospital, we continued to offer specialist care for pregnant women, lactating mothers, and children under the age of five, and supported the referral of patients in need of more advanced care from a general healthcare facility to the hospital.
In Bombali district, also in Northern province, MSF worked to improve access to diagnosis and treatment for both drug-sensitive and drug-resistant TB for adults and children. People who are at high risk of contracting TB are provided with preventive therapy through the country’s National Leprosy and Tuberculosis Control Programme, of which MSF is supporting the roll out.

116,293
116,293
86,500
86,5
6,070
6,07
2,120
2,12

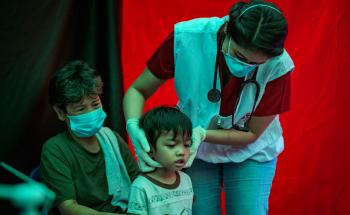
Urgent Action Needed as Governments and Donors Fail Children with TB
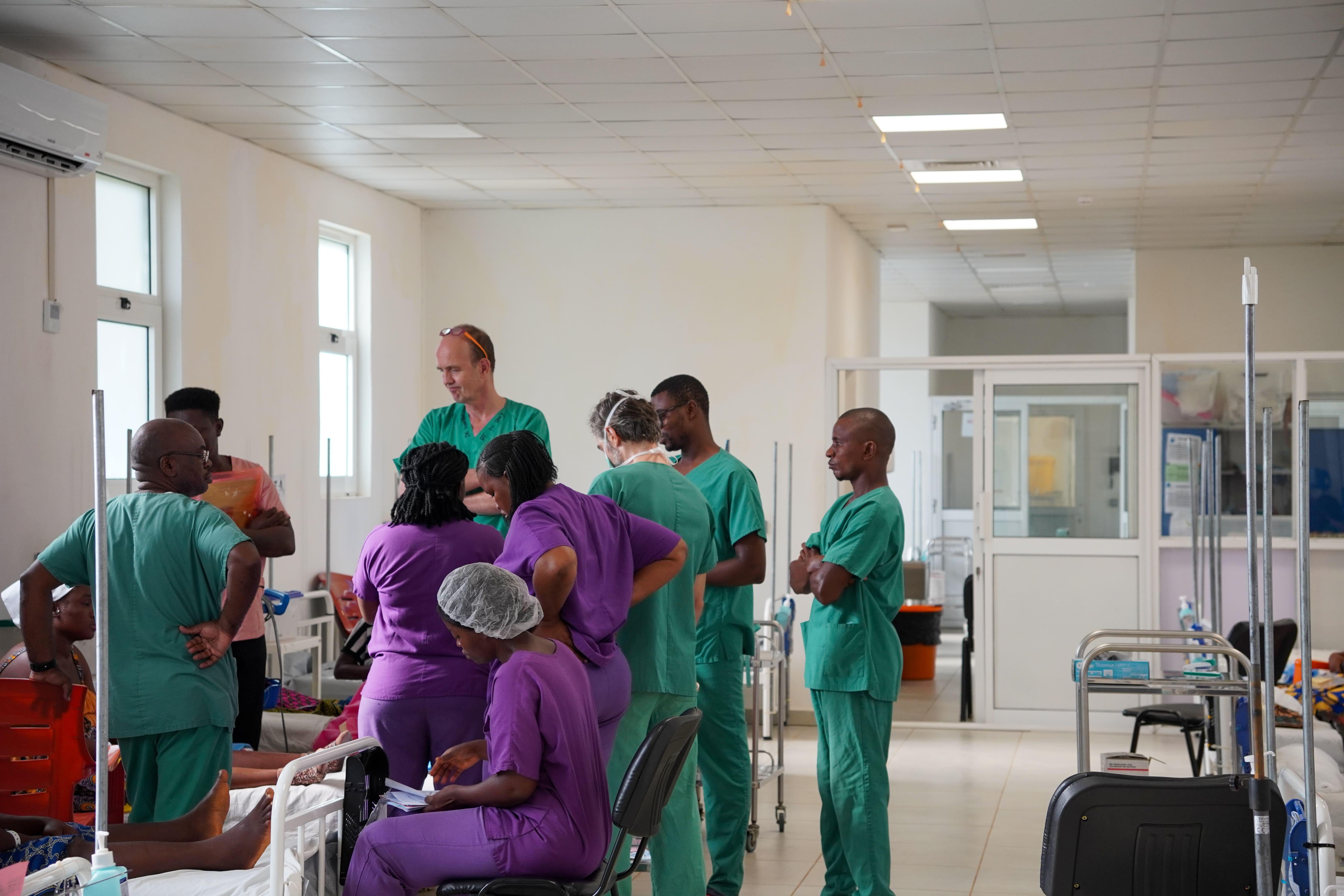
A Midwife's Journey in Kenema, Sierra Leone

Danaher Charges Exorbitant Prices for Lifesaving Medical Tests for HIV, Hepatitis & XDR-TB

Helping pregnant women reach hospital in time