Somalia
In 2024, droughts and floods forced over half a million people from their homes, bringing the total number of displaced people in Somalia to more than 3.5 million. Many are living in overcrowded, unsanitary conditions in camps, with little access to healthcare, leaving them vulnerable to measles, cholera, and respiratory infections. Hundreds of thousands of people are facing severe malnutrition, as repeated extreme weather events have led to crop failures and the death of livestock, as well as a shortage of clean water.
Our activities in Somalia and Somaliland in 2024
Data and information from the International Activity Report 2024.
132
132
€15.5 M
15.5M
1979
1979
Featured
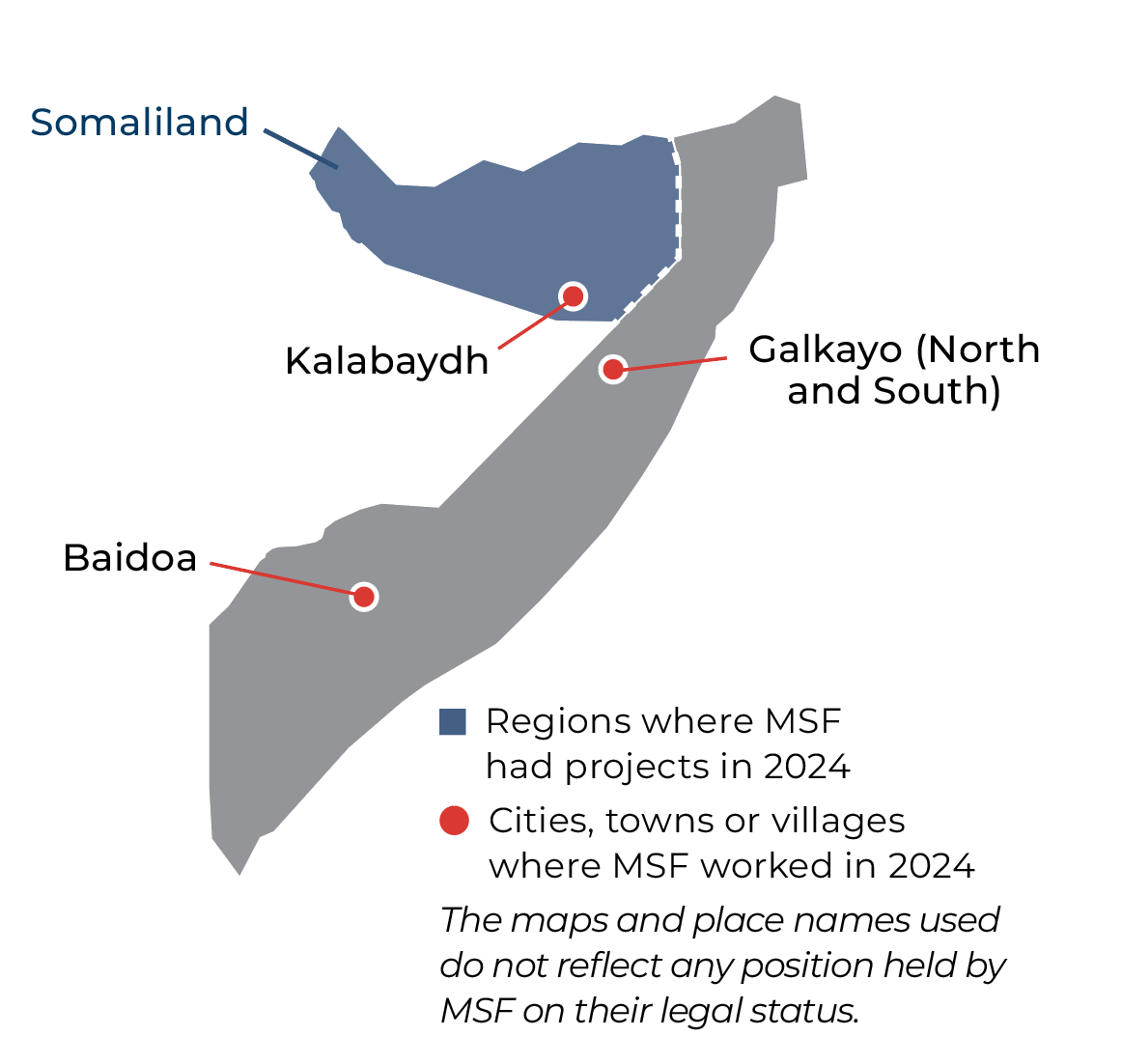
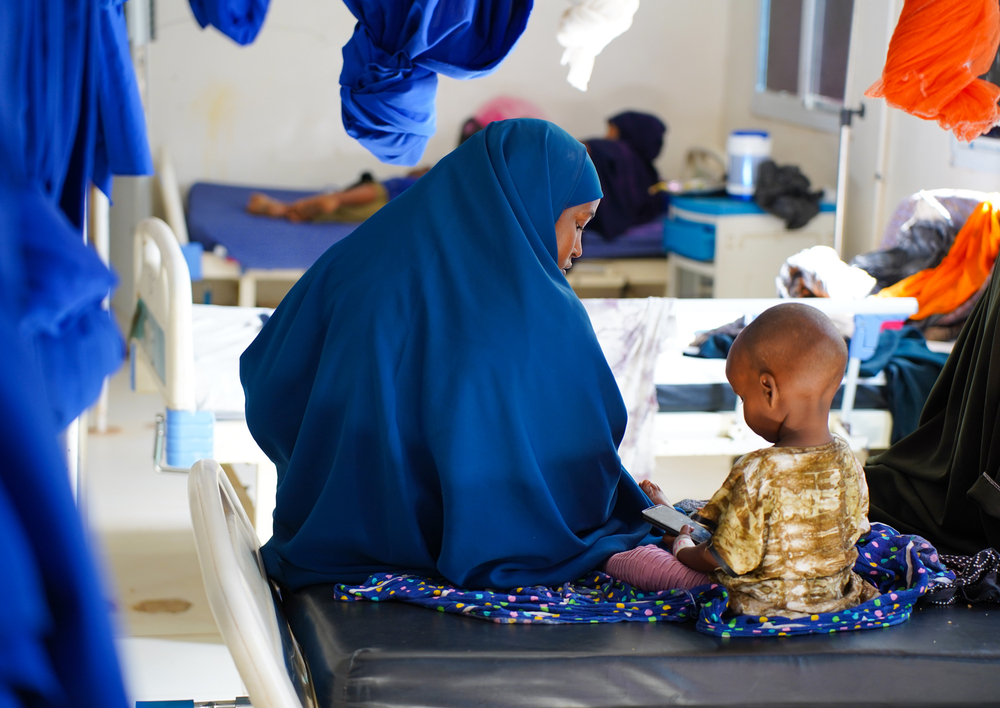
In Baidoa, the capital of South West state, which currently hosts more than 1.1 million displaced people, our teams are responding to the ongoing humanitarian crisis, which has been exacerbated by conflict and a lack of healthcare and other essential services. At Bay Regional hospital, we deliver emergency obstetric care, neonatal services, and inpatient care for children with malnutrition. In 2024, our outreach teams also worked in seven locations to ensure early detection and treatment of complications among expectant mothers and newborns, and refer them for specialist care.
In Puntland’s Galkayo North, our services include supporting the emergency room, maternity, and paediatric units at Mudug regional hospital, treating malnutrition and tuberculosis, and running mobile clinics to address the needs of displaced communities. In Galkayo South, Galmudug state, we work with a local hospital to provide emergency care, maternal and child healthcare, including vaccinations, and respond to emergencies in camps. In addition, we send mobile teams to remote areas where healthcare facilities have ceased to function.
Until April, we supported basic and specialist care in Kalabaydh, Sool region, and later in the year donated medical supplies to healthcare facilities in the region.
As part of our regular outreach work, MSF has helped improve healthcare facilities by upgrading water and sanitation systems, and training local healthcare workers in Somalia to support the Ministry of Health’s efforts to strengthen services.
IN 2024

57,400
57,4
6,990
6,99
1,810
1,81
270
27


One year later: How US policies are reshaping global health and humanitarian aid

MSF and West African artists sound the alarm on the health impacts of the climate crisis

How Funding Gaps and Barriers Undermine Healthcare for Women and Children

MSF’s Green Initiative Brings Sustainable Healthcare and Climate Resilience to Somalia