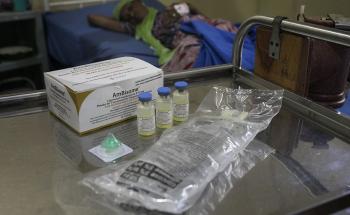
A range of antibiotics can treat the infection, including penicillin, ampicillin, chloramphenicol and ceftriaxone. Under epidemic conditions in African in areas with limited health infrastructure and resources, ceftriaxone is the drug of choice
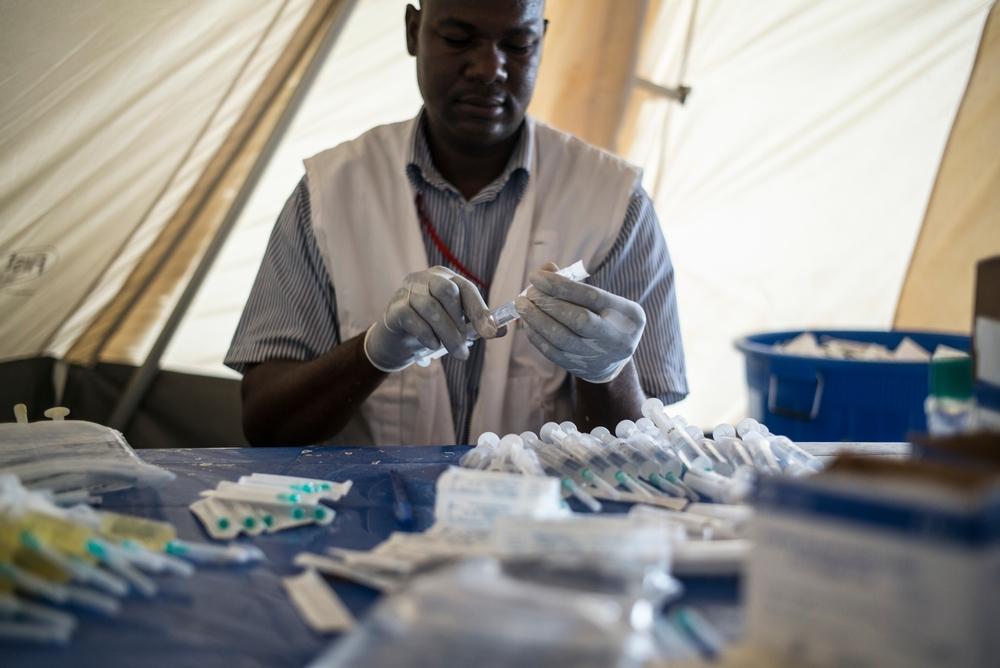
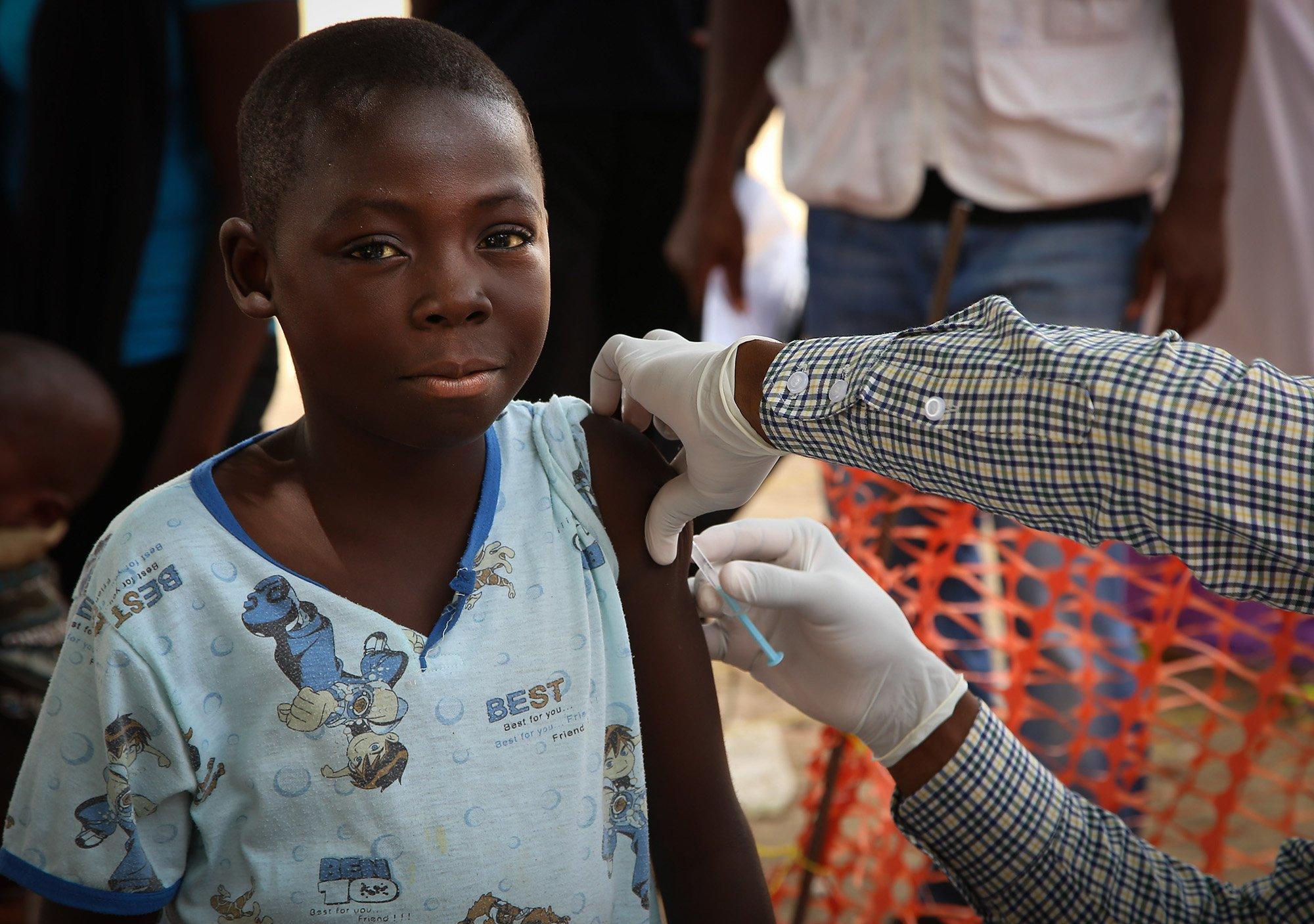
However, timely mass vaccinations are the most effective means of limiting the spread of epidemics.In 2010, a new meningococcal A conjugate vaccine was introduced in Africa and, as of November 2017, more than 280 million people had been vaccinated.
According to the WHO, this has led to a 58 percent drop in cases and reduced the risk of epidemics by 60 percent. Maintaining high immunisation coverage is expected to eliminate meningococcal A epidemics from the meningitis belt completely.
However, other strains are still causing epidemics. Conjugate vaccines against multiple meningococcal strains (ACWY) are very expensive and in short supply, and are, therefore, impossible to use for wide-scale preventive campaigns.
A new meningococcal conjugate vaccine against the ACWYX strains is currently being developed and expected to be available at an affordable price in 2021 or 2022.