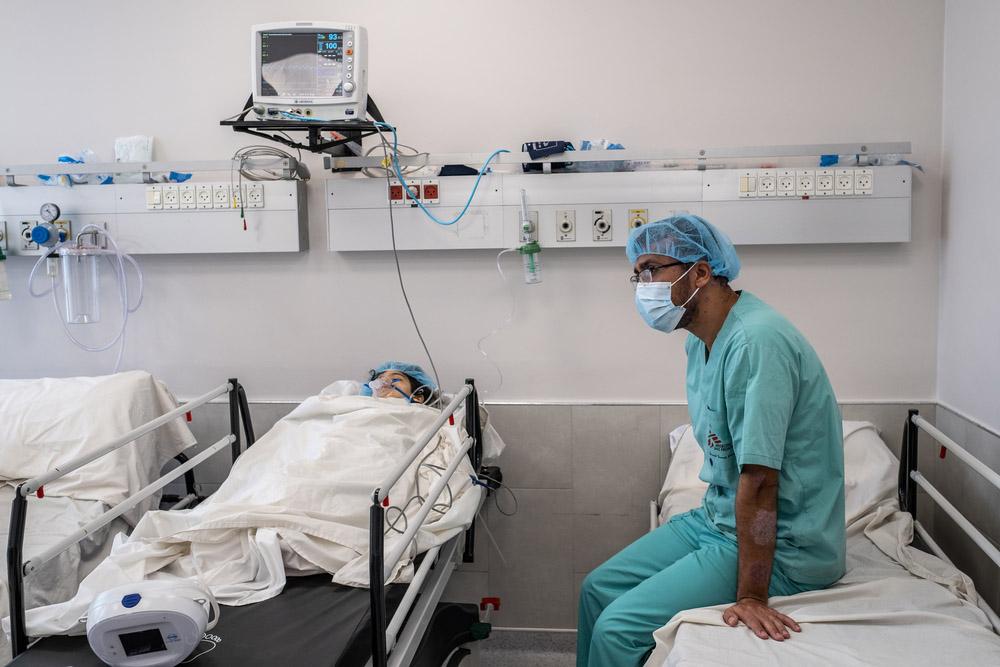
In a training room in Gaza City, a group of healthcare workers from across the Gaza Strip gather, introducing themselves as doctors, nurses, administrators, technicians, and other medical professionals. Mahmoud and Hana, Doctors Without Borders (MSF) psychologists, hand out materials and explain the agenda for the day: It’s a session of the “Helping Helpers” programme, a training on mental health topics for healthcare professionals in the Gaza Strip, organized by MSF with the Ministry of Health.
The last three years have been extremely taxing for this group of professionals – not least because of the COVID-19 pandemic. They have also been on the frontlines of two escalations of violence, in May 2021 and August 2022, treating patients impacted by the Israeli bombings and the trauma of war.

The “Helping Helpers” training that this group has gathered for aims to open up the conversation, in a safe space, about the importance of mental health for healthcare workers. Capacity-building sessions during the day include anger management, managing stressful situations, self-care, and breaking bad news to patients.
According to Antonella Pozzi, MSF Mental Health Activity Manager in Gaza, “MSF decided to develop this activity since in Gaza, medical and non-medical staff deal with a population that has suffered and continues to suffer ongoing traumatic circumstances. These personnel deal with challenging situations and indirect exposure to potential trauma, that if not properly channelled, can create a build-up leading to severe psychological consequences, such as burn out.”
Nessma, a doctor in a Gaza City hospital, says, “Every day, we deal with physically ill people who are tired and sick, who want someone to stand with them and care for them and deal with their problems.” She says patients need doctors who are aware of the mental impact of these crises and who themselves are in tune with and resilient to their own stressors.

Patients need doctors who are aware of the mental impact of these crises and who themselves are in tune with and resilient to their own stressors.Nessma, Medical Doctor in Gaza City Hospital
Today, Nessma and 11 others are gathering for a full, one-day session run by MSF psychologists Mahmoud and Hana to discuss about the difficulties and challenges they face as healthcare providers in Gaza and to learn about skills to cope.
During the COVID-19 pandemic, the everyday pressure experienced by healthcare workers around the world was amplified, and global awareness about the need to support those carers was raised. Yet not included in these conversations has been the triple burden that healthcare workers in settings like Gaza have shouldered in addition to the pandemic – low resource settings with an impoverished population and operations in conflict zones where they often see influxes of trauma patients.
In Gaza, healthcare professionals are working in an extremely challenging environment. The 15-year blockade on Gaza and the recurring outbreaks of violence continue to cripple the healthcare system. This combination of factors has led to a decrease in operational hospital beds and affected the availability of human resources such as nurses and doctors. In addition, the restrictions imposed on imports by the Israeli authorities, which are reinforced during periods of violence, often result in medical shortages in Gaza hospitals. In August 2022, the closure of the border crossings for several days compromised the entrance of essential medicines and medical supplies and led to a severe fuel shortage, which affected the functioning of Gaza’s healthcare infrastructure.

For one of the participants in the session, a radiologist in Gaza City, the uncertainty of war adds to her anxiety and impacts her own mental health. She notices it in her patients too. “Patients experience psychological pressure due to an unstable political and security situation that fluctuates every day. In Gaza, we’re always waiting to know if there is going to be a war today or not, waiting for a bomb and waiting for a missile to hit and these things. Dealing in our daily lives with fires and ambulances on the streets.”
In order to best serve her patients, she says, “We need to learn to deal with all of these things.”

Of course, hospital staff in Gaza also experience many of the same issues confronted by their peers around the world, even in peaceful contexts. Mahmoud, one of the session’s facilitators, says long working hours, staff shortages, and pressure from superiors and patients’ families weigh heavily on the participants he meets in his “Helping Helpers” sessions.
The sessions he runs on self-care aim to alleviate those pressures by teaching staff to identify symptoms of burnout and mental distress within themselves and strategies to put up personal boundaries and ask for help. With these sessions running twice per week, MSF aims to target hundreds of healthcare workers.
We have learned new concepts, documented concepts and solutions to some of the problems that we face like any other human being, whether at home, at work, with colleagues, or with patients.
Mahmoud emphasizes that the program is just the start of a discussion about mental health that should continue. The participants commit to contribute to it and to share the new skills they’ve learned today with their colleagues.
The Head of a physiotherapy department at a pediatric hospital in Gaza says, “These sessions really moved us from a psychological gap, fatigue, exhaustion and routine to something else, and we have learned new concepts, documented concepts and solutions to some of the problems that we face like any other human being, whether at home, at work, with colleagues, or with patients.”