It’s normally quite hard to catch up with Zani Prinsloo, a nurse and midwife working as an MSF sexual and reproductive health (SRH) trainer. Before the COVID-19 outbreak, she would travel to MSF projects in different countries and teach colleagues about women’s health issues, sexual violence and safe abortion care. Since South Africa went into lockdown, however, she’s been supporting MSF teams around the country to deal with the outbreak and its knock-on effects.
The level 5 lockdown in April found her in rural Eshowe and Mbongolwane, KwaZulu-Natal, where MSF runs an extensive HIV and TB project in the community. “I was completely out of my comfort zone compared to the projects I’ve worked on before, but I loved it,” Zani says, laughing.
Given the added vulnerability of patients with pre-existing conditions like HIV and TB during the COVID-19 outbreak, the team quickly focused on decongesting busy clinics so that patients needing chronic medication could collect it from sites nearer to home, reducing the risk of coming into contact with coronavirus.
Over the years, MSF has set up 12 “Luyanda” sites to screen and monitor TB patients. These community sites offer testing, monitoring and linking to treatment for HIV and TB, as well as other chronic conditions, like high blood pressure or diabetes.
In March, after the first COVID-19 case was confirmed in a KwaZulu-Natal community, the Luyanda sites became key collection points for patients as the team rolled out their TIC-TOG strategy: treatment in the community and treatment on the go. The strategy identified 35 medicine pick up points, including the already functioning Luyanda sites.
“This process involved so many people,” explains Zani. “Our data team starts with tracing people on antiretroviral (ARV) and TB treatment, as well as people with non-communicable diseases, who are at the highest risk if they get COVID-19. After retrieving the list we had about 20,000 patients in the Eshowe and Mbongolwane area.”

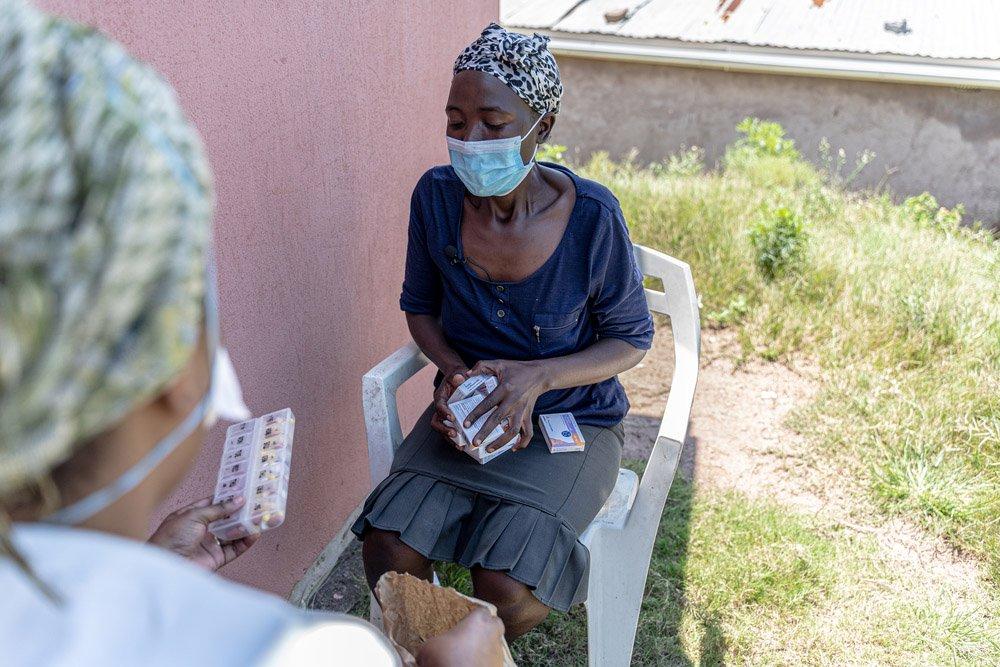
From there another team started calling these patients one by one to confirm addresses, allocate a pickup point and arrange for collection of their medication on certain days. MSF health workers would pre-package the medication needed and then distribute to three or four pickup points every day. “We brought the treatment to the community,” says Zani. “It’s a big job, but if we don’t ensure that people stay on their chronic medication, they could experience a lot of health problems in a few months from now.”
While pre-packing medicine the team also reviewed patients’ charts to see if they were due for viral load testing, which is essential to monitor on an annual basis to determine whether an HIV patient’s medication is working and if it’s necessary to change their treatment or provide additional support as required.
If patients were due for this check-up the team made sure to conduct the test at the same time that the patient collected their medication. MSF community health workers also offered family planning, collection of sputum for TB testing and even some immunisations to anyone coming to pick up medicine.
“In the first month of lockdown, we saw that a lot of patients didn’t come for treatment at the bigger clinics. Women didn’t access family planning because people were really afraid of COVID-19 infection,” Zani tells us. It was, therefore, a huge relief for the team that they could offer patients a “two-in-one” consultation at a Luyanda site.
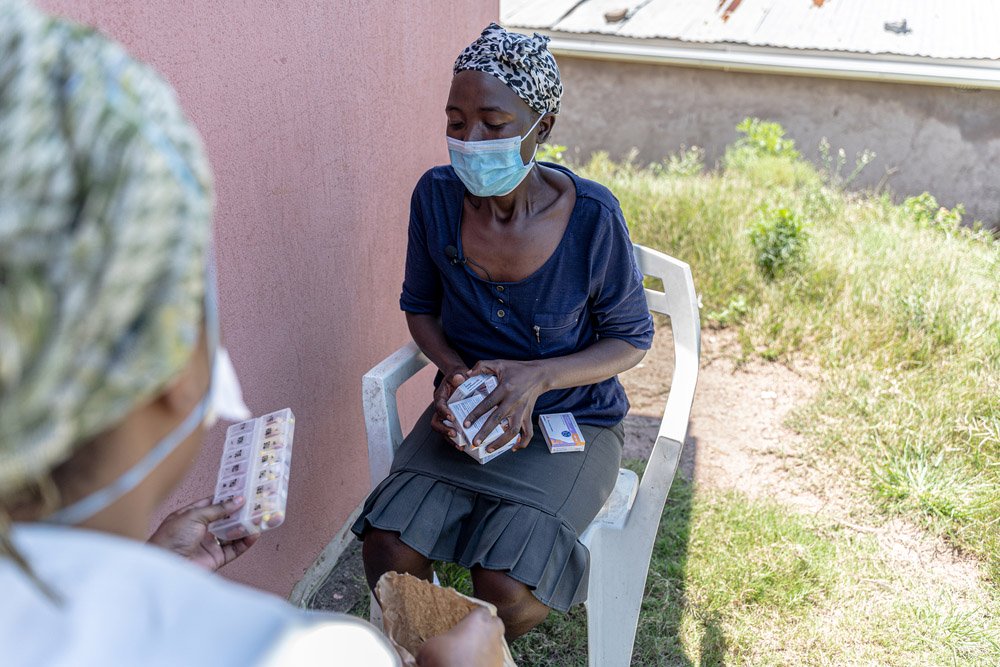
But what about the patients who don’t come and collect their medication? “We do our best to follow up and reschedule times for our patients,” says Zani. “What is really great about the Luyanda sites is that the community health workers have gained a lot of trust over the years within the community. So, at the end of the day, if someone didn’t come for treatment they know where they live, and they’ll go deliver the medication to their home.”
To avoid any stigma about medication, packages are sealed and the teams delivering them don’t know what medication they are delivering. “We maintain strict confidentiality,” says Zani. “Our community health workers don’t know who is getting medicine for blood pressure or who is getting for HIV.”
After working mainly in SRH and maternity hospitals for many years with MSF, Zani says it was wonderful to experience working in a community-based project. “I learnt a lot from the team. The work they do really impacts the community,” she says. “It was also great to show people that in the time of COVID-19 we are still prioritising HIV and TB; we will never neglect it.”
MSF has been working in Eshowe since 2011 in partnership with the provincial Department of Health. Our HIV and TB project seeks to implement multiple strategies to reduce the high incidence of HIV and TB in the area. The project supports several clinics and hospitals in the Eshowe urban and Mbongolwane rural health services areas and MSF runs 12 remote ‘Luyanda’ clinics to service the community closer to their homes.