

Bangladesh
MSF provided emergency care and sexual and reproductive health services, as well as mental health support and treatment for victims of sexual and gender-based violence.
We also treated patients for a range of non-communicable diseases, acute watery diarrhoea, respiratory infections, dengue fever, and measles.
Featured
Our activities in 2024 in Bangladesh
Data and information from the International Activity Report 2024.
1,924
1,924
€28.8 M
28.8M
1985
1985
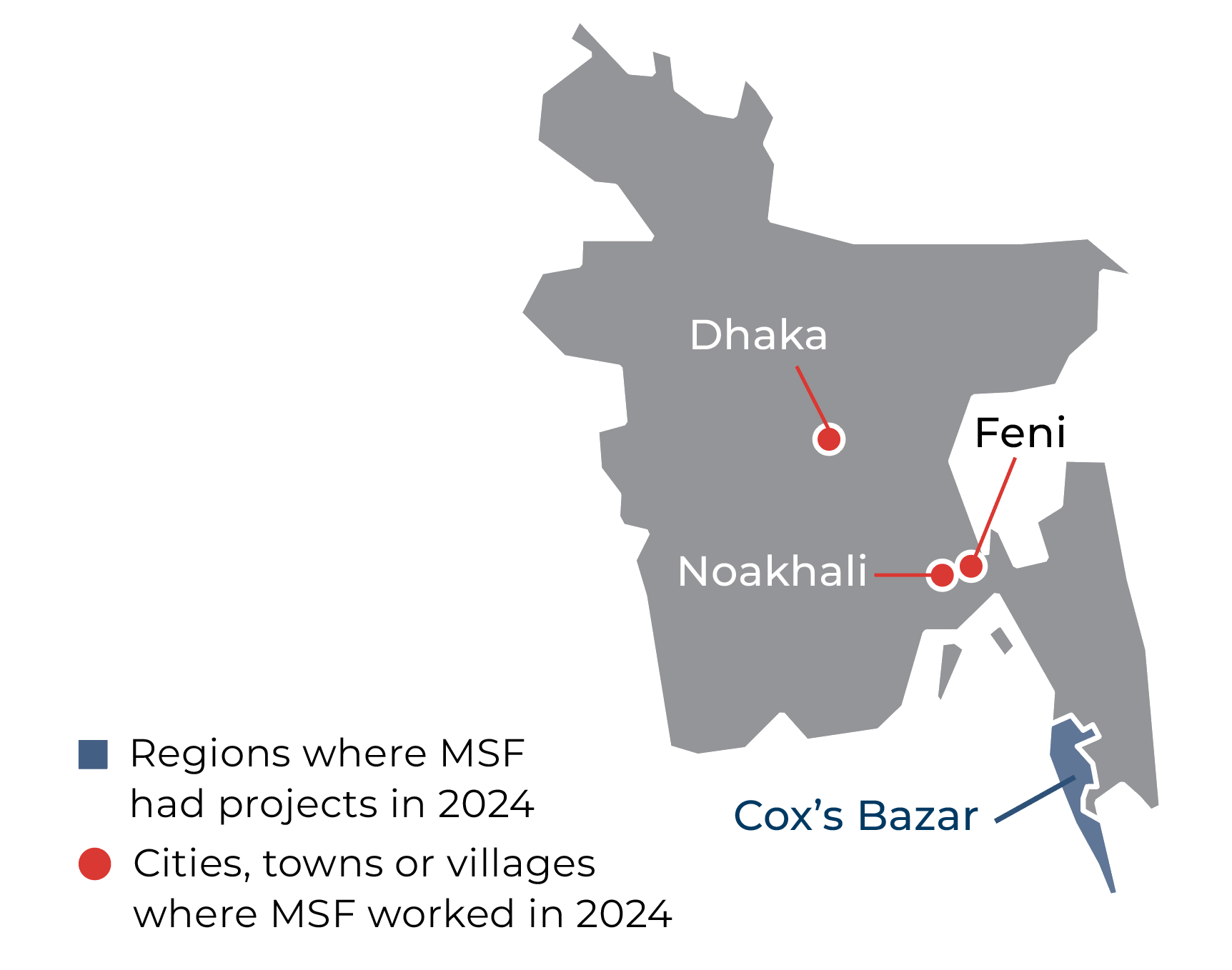
Since mid-2022, there has been a significant increase in violence inside the Cox’s Bazar refugee camps, due to conflict over the border in Myanmar.
In September 2024, the fighting between armed groups reached such a level that we had to temporarily suspend activities in some of the camps for a number of days. MSF teams treated some of the injured. Earlier in the year, we also witnessed Rohingya boys and young men being threatened and pressured into returning to Myanmar to fight.
Scabies remained a major health issue in Cox’s Bazar. In the last quarter of 2024, we saw a sharp increase in cases compared to 2023, when numbers had reduced following a mass drug administration. An MSF-led assessment found reduced chlorination and poor water distribution across all camps, likely contributing to a rise in water-borne diseases.
A study carried out by Epicentre, MSF’s epidemiological centre, published in June, reported a high prevalence of hepatitis C infection in adults living in the camps. By December, MSF and other organisations had committed about 60 per cent of the needed resources to tackle the virus.
In the capital, Dhaka, MSF ran two clinics in Kamrangirchar district, offering sexual and reproductive healthcare, medical and psychological treatment for victims and survivors of sexual and gender-based violence, and occupational health services for factory workers.
IN 2024

624,100
624,1
3,930
3,93
3,330
3,33
220
22

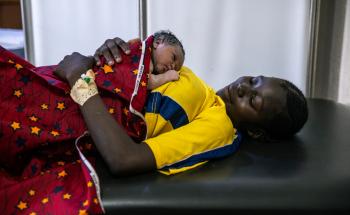
Challenges in accessing lifesaving maternal care

The Taro leaf Statement

“We are still here”: The taro leaf as a metaphor for the Rohingya experience

MSF concludes emergency response supporting over 1,900 flood-affected patients in Bangladesh

