

Central African Republic
We have implemented new approaches to care in Bangassou and Batangafo, by expanding community-based services through training for traditional birth attendants on family planning, and for community health workers on malaria, diarrhoea, and respiratory infections.
In addition, our teams respond to disease outbreaks and provide mental health support, basic healthcare, and specialist referrals. Malaria is one of the most common diseases we treat, and the deadliest, particularly for children under five. The general lack of prevention measures and treatment lead to high infection rates, particularly during the rainy season.
Featured
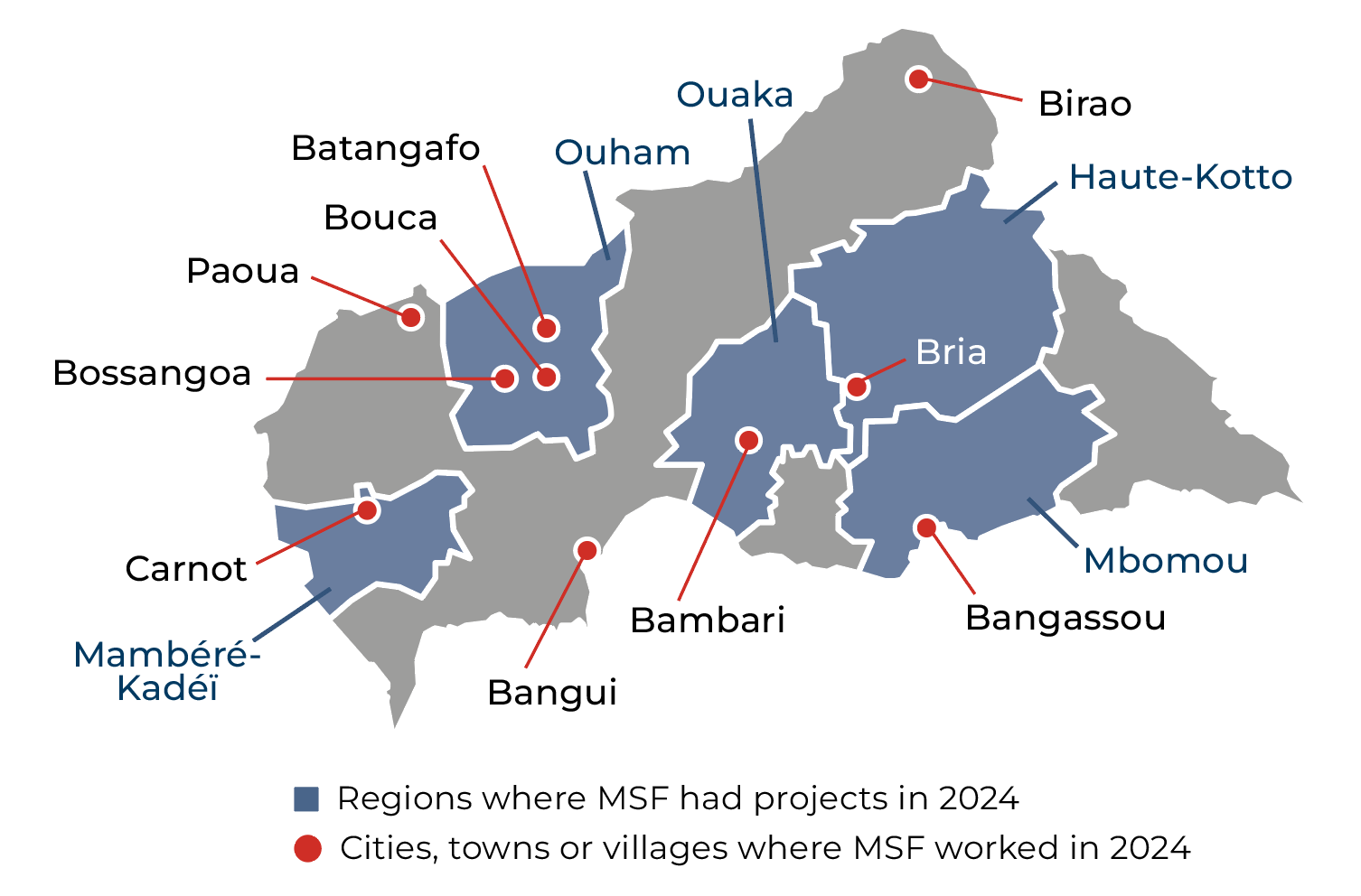
Our activities in 2024 in Central African Republic
Data and information from the International Activity Report 2024.
2,379
2,379
€68.1 M
68.1M
1997
1997
Addressing gaps in care
The healthcare system in CAR remains critically weak due to shortages of trained personnel and medical supplies, and an overall lack of health facilities. Even where healthcare is available, many people die from preventable diseases because they are unable to afford treatment. In rural areas, the healthcare facilities where MSF teams work are often the only places offering free medical care.
In 2024, we scaled up malaria treatment activities in several districts where outbreaks were severe. This included chemoprevention in Batangafo and Bossangoa as a method for protecting infants under one year old.
CAR also has one of the highest HIV prevalence rates in the central African region. Antiretroviral coverage is low, and the disease is a leading cause of death among adults. MSF continues to expand access to treatment – including for patients with advanced HIV – and improve patient follow-up to ensure adherence to treatment by supporting Ministry of Health staff.
Emergency and specialised medical services
During 2024, MSF teams launched emergency responses to assist refugees from neighbouring Sudan and Chad. These included general healthcare services, and vaccination campaigns to contain measles and whooping cough outbreaks. In areas with high maternal death rates, MSF strengthened maternal healthcare services, ensuring that pregnant women received essential antenatal care.
While most of our projects are in rural areas, we continue to work in the capital, Bangui, supporting trauma surgery, obstetric and neonatal care, advanced HIV and TB treatment, and comprehensive medical and psychological care for victims and survivors of sexual violence.
IN 2024

543,600
543,6
324,800
324,8
10,300
10,3
4,820
4,82

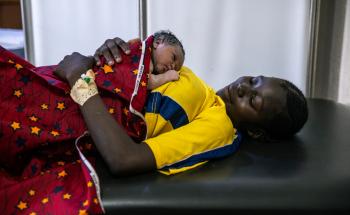
Challenges in accessing lifesaving maternal care

MSF Warns of Consequences as Funding Cuts Threaten Fight Against AIDS, TB and Malaria

Difficult Access to Healthcare for People Around Bambari

Central African Republic - A silent health crisis

