‘2030 is too late for the nearly one million people with HIV who died in 2017’
Today, in the era of Test-and-Treat, an estimated one million people still die of AIDS each year. This is simply unacceptable. It is a failure and an indictment of the HIV response.
Mortality among young HIV positive adolescents is a scandal. We are not getting ahead of the epidemic affecting adolescent girls and young women, and for all other key population groups at highest risk of HIV infection.
At AIDS2018, many continue to emphasize 2030; we are here to talk about today.
2030 is too late for the nearly one million people with HIV who died in 2017.
We need a course correction from the Global Fund, the US and European governments and other donors so that we can get ahead of the crisis.
By intensifying the pace of scale-up while expanding management of advanced HIV disease, including access to testing and treatment for Opportunistic Infections (OIS) in PLHIV who present for the first time and those who fail on antiretroviral therapy (ART), and or drop out and come back into care.
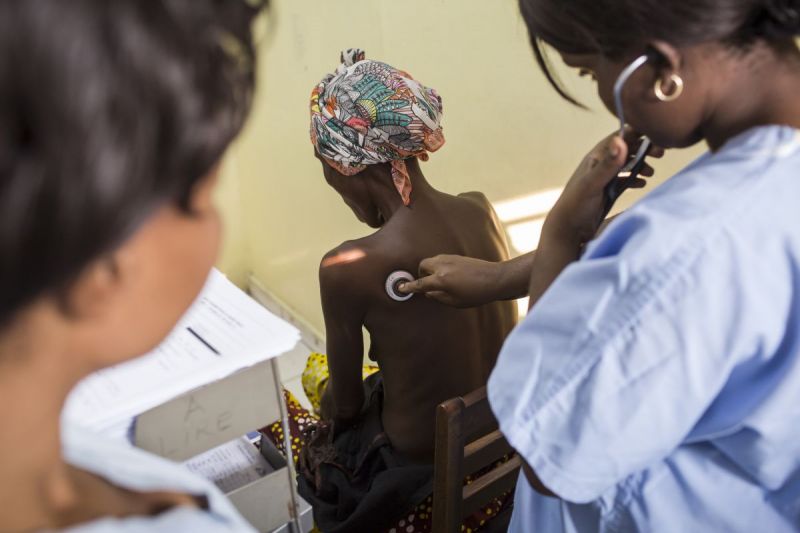
A substantial portion of AIDS-related deaths occur in individuals who have already started treatment. We must stop turning our backs on these PLHIV.
Today, only 21.7 million of the 36.9 million people infected with HIV have access to life-saving antiretroviral treatment. Nearly half of those starting treatment present with advanced disease, meaning increased risk of death and increased need for more than just ART.
PLHIV with advanced disease need [i] access to diagnostics (urinary lipoarabinomannan (LAM), cryptococcal antigen lateral flow assays (CrAg LFAs)) and initial treatment for OIs including tuberculosis, cryptococcal meningitis, and bacterial sepsis before the start of ART.
We cannot expand and accelerate the HIV response without more funding. In prevention alone, we see the effects of reduced financing. DREAMS cannot expand to all the geographic regions where it is urgently needed because programs are starved for funding. In Zimbabwe, DREAMS is only reaching 50% of adolescent girls and young women in six districts with a minimum package of interventions.
The tools and WHO policy exist to make a major reduction in the impact of advanced HIV disease, but they are not being funded, they are not being implemented, and they are hardly being spoken about. WHO has issued recent guidance on both advanced disease and cryptococcal meningitis in particular, and advocates packages of tests and treatments for PLHIV with advanced disease.
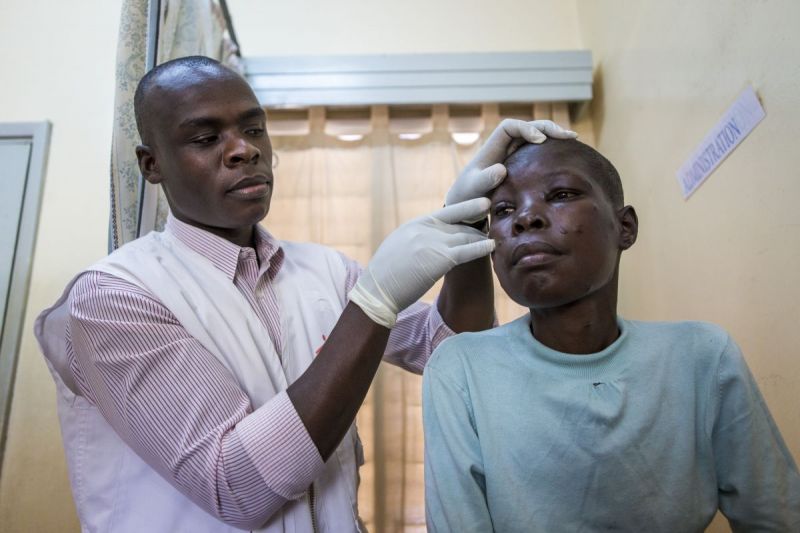
However, these diagnostic tests and treatments for OIs are currently unavailable in most low- and middle-income country (LMIC) settings, despite 30-50% PLHIV presenting or representing to care with advanced disease. Recent data is showing that about three-quarters of HIV-infected in-patients hospitalised in LMICs are ART-experienced.
This is why we see:
- An estimated 280,000 AIDS deaths in West and Central Africa in 2017
- 150,000 AIDS deaths in Nigeria in 2017
- 70,000 AIDS deaths in Mozambique in 2017
- 110,000 AIDS deaths in South Africa in 2017
- 135,000 deaths (15-20% HIV-related deaths) from cryptococcal meningitis alone annually
In fact, a recent study evaluating official mortality statistics in Zambia suggests that these estimates of deaths may be vastly underestimated. Latest trial data and WHO guidance on cryptococcal disease, a leading cause of death for PLHIV with advanced disease, could cut cryptococcal meningitis mortality from rates of 70% by over half.
However, in routine care settings, the most basic diagnostic tests and treatments, including the key off patent, 50-year-old antifungal flucytosine, are completely unavailable in resource-limited settings where disease burden is highest.
Despite making up just 7% of the world population, the West and Central African region alone accounts for 28% of total AIDS-related deaths.
We cannot turn a blind eye to these deaths.
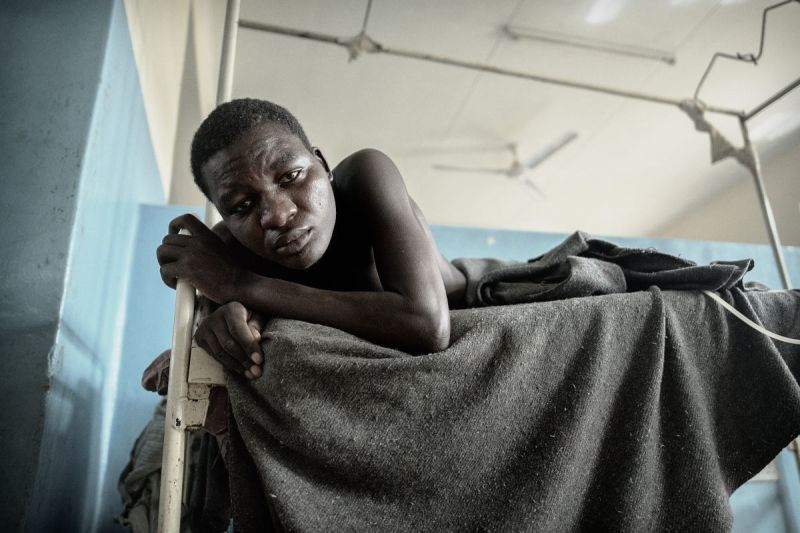
You, Mr. Sands and Ambassador Birx, cannot look away.
We demand:
- The Global Fund must announce a bold replenishment target of 18 billion, including a commitment to address the treatment emergency in West and Central Africa that has been exacerbated by the Global Fund’s decision to slash funding allocations in that region.
- The US government must stop flat funding PEPFAR, building on the $50 million increase that will come FY2019.
- UNAIDS, a concrete global plan to realise the targeted mortality reduction below 500,000 by 2020, including supports to test and start and roll out of tools we need to address the leading causes of AIDS deaths.
Global Fund and PEPFAR must require its implementers and fund recipients to measure and report on deaths directly so they are held accountable.
All donors need to step in and support urgent efforts to supply diagnostic tests (urinary LAM and CrAg LFA) and treatments for opportunistic infections (flucytosine, amphotericin B (AmB) and work on in-country demand including education programs for Health Care Workers on integrated packages of tests and treatments for advanced disease as per latest WHO guidance.
Organizations: Coalition PLUS, Doctors Without Borders/Médecins Sans Frontières (MSF)
Sources:
[i] UNAIDS. Miles to Go, July 2018.
