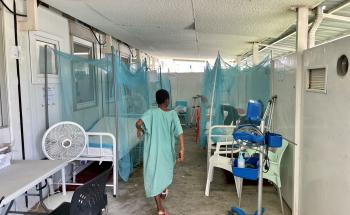
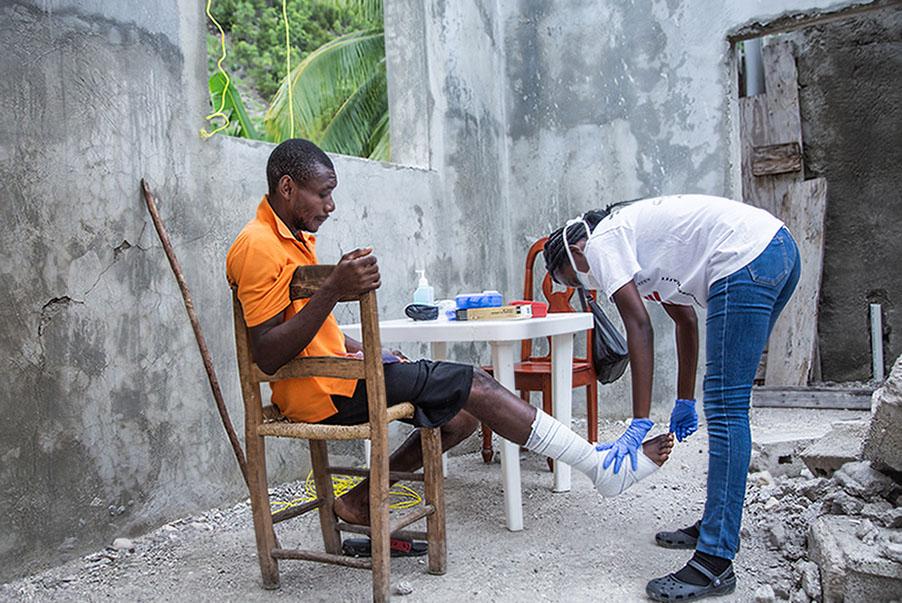The first quarter of 2024 was the deadliest since the UN began tracking armed group violence in Haiti. Between February and April, the number of patients arriving with gunshot wounds at MSF’s Tabarre trauma hospital surged from 60 to 100 per month, and we had to expand from 50 to 75 beds to meet the growing demand for surgery. Several major hospitals in Port-au-Prince closed due to mounting insecurity. In 2024, Haiti recorded 5,600 deaths and 2,200 injuries related to violence, a 17 per cent increase compared to the previous year.
Mass displacement is deepening the humanitarian crisis in Haiti, with over one million people driven from their homes in the span of a single year. Many live in informal sites with limited access to water and sanitation facilities, which increases the risk of water-borne diseases. In August, MSF provided treated water in 15 sites, trained site managers on water chlorination and hygiene, built or renovated latrines and emergency showers, and distributed hygiene kits. MSF’s mobile clinics treated people for a wide variety of conditions, including water-borne diseases such as acute watery diarrhoea, and scabies.
In this volatile situation, MSF teams faced severe security threats and incidents that disrupted operations. On 11 November, during an attack on an MSF ambulance, two patients were executed, and accompanying staff members assaulted. In the following days, MSF ambulances were repeatedly stopped by police, who threatened staff with death and sexual violence. As risks grew, we temporarily suspended most of our activities in Port-au-Prince on 20 November, further reducing access to critical healthcare. We partially resumed activities on 11 December.
Treatment for trauma and burns
In March, in response to the significant increase in emergency medical needs, MSF opened the Sant MSF pou Blese trauma centre in Carrefour, Port-au-Prince, to treat victims of gunshot wounds, stabbings, burns, and road accidents. The Turgeau emergency centre, which had closed in December 2023 after a patient was forcibly taken from an ambulance and killed, reopened in March to strengthen emergency care.
On 14 September, a fuel truck explosion in Miragoâne, Nippes department, injured many people. MSF responded by providing critical care to 16 burns victims at Tabarre trauma hospital, the only facility with a specialist burns unit in the country, and six others at Carrefour trauma hospital. As well as treatment for wounds, MSF offers physiotherapy and mental health support to burns patients.
Sexual and gender-based violence
The ongoing gang war in Port-au-Prince has led to a steep increase in sexual and gender-based violence (SGBV), leaving victims and survivors in urgent need of shelter, mental health support, and medical care. Since 2015, MSF has offered comprehensive medical and psychological support for victims and survivors of SGBV through Pran Men’m clinic. In 2024, we also provided these services at Carrefour maternity hospital, and at a new programme in Cité Soleil. Meanwhile, we concluded a five-year project that we had been running in Gonaïves, Artibonite department, focused on adolescent sexual health and supporting victims and survivors of SGBV.
Maternal health
The maternal death rate in Haiti remains alarmingly high, rising from 154.9 deaths per 100,000 births in 2022 to 201.2 in 2023. South department, still reeling from the 2021 earthquake, has one of the highest rates, at 343.9 deaths per 100,000 births.[5]
Many healthcare facilities have still not been repaired, while in Port-au-Prince, the brutal fighting in the streets prevents women from seeking care. In response, MSF, in partnership with the Ministry of Public Health and Population, continues to offer emergency obstetric and neonatal services in Port-à-Piment, where teams assist with deliveries, including those requiring specialist care.
To further improve maternal healthcare, MSF started to rehabilitate Isaïe Jeanty maternity hospital in the Chancerelles district of the capital in November 2024. Once completed, the facility will deliver free, high-quality maternal care, family planning, support for victims and survivors of SGBV, and referrals.