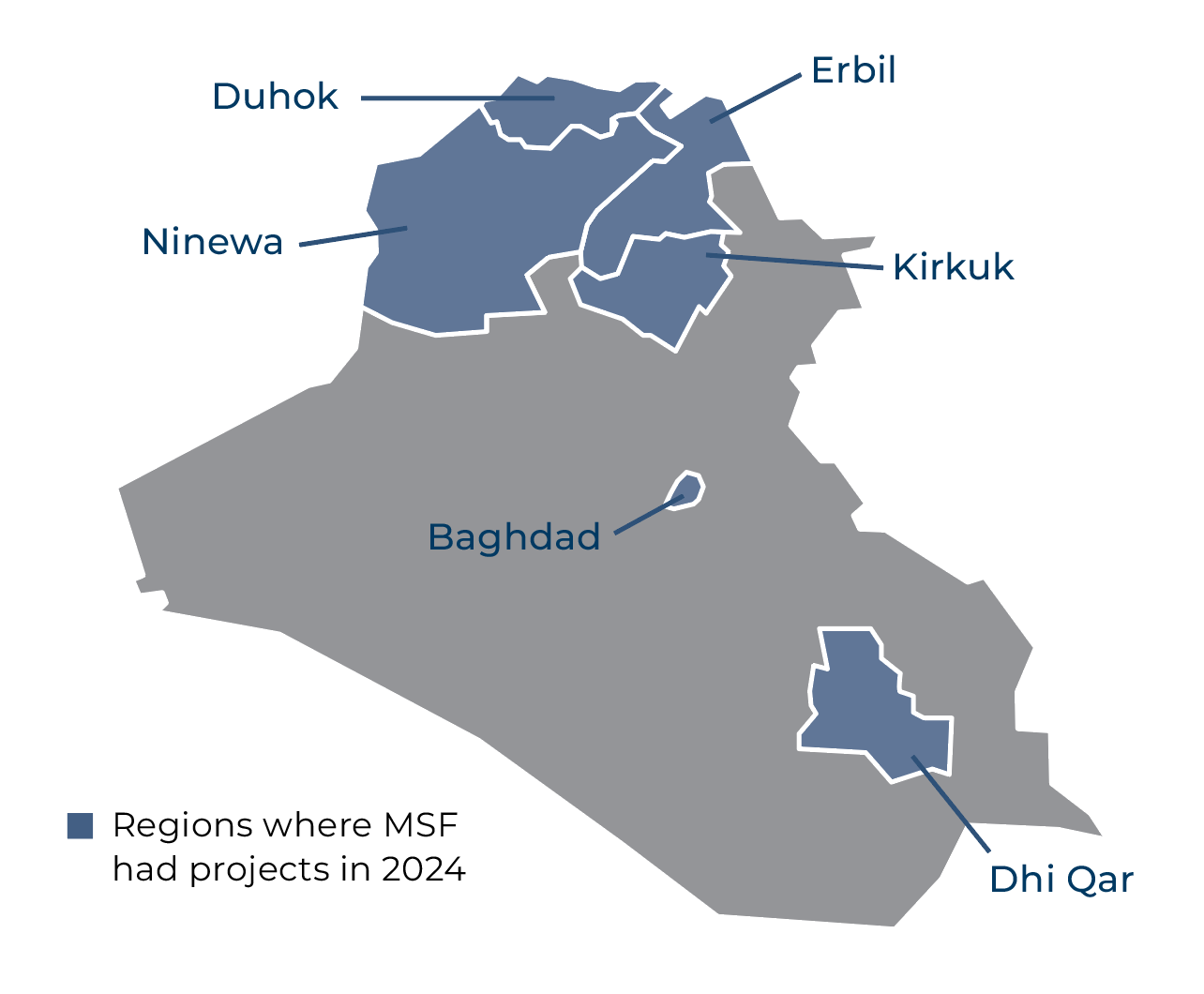
Maternal healthcare was the focus of our activities in Ninewa and Dhi Qar governorates. Our teams provided ante- and postnatal care, assistance with deliveries and family planning, as well as offer mental health support and health promotion activities, at two clinics in Mosul – Al-Ubur, on the western outskirts, and Al-Ama, in the Al-Nahrawan neighbourhood – in Ninewa. We provided the same services in Garmat Bani Saeed, in Dhi Qar, until the end of the year.
Meanwhile, at our field hospital in Mosul’s Nablus neighbourhood, we offered basic maternity services, as well as deliveries by caesarean section, neonatal healthcare, and emergency paediatric care.
We also continued to support the national tuberculosis programme with new treatment protocols and training, while ensuring a continuous supply of medications and conducting screening campaigns in places of detention.
In addition to our regular projects in Iraq, we collaborated with directorates of health in various governorates and the ministries of health in both federal Iraq and the Kurdistan region, by training healthcare staff and enhancing infection prevention and control measures in health facilities.