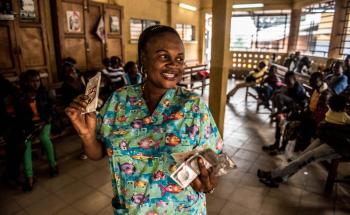In July 2023, Doctors Without Borders (MSF) closed the chapter on one of its longest-standing projects in Malawi, launched 25 years ago in response to the HIV/AIDS epidemic.
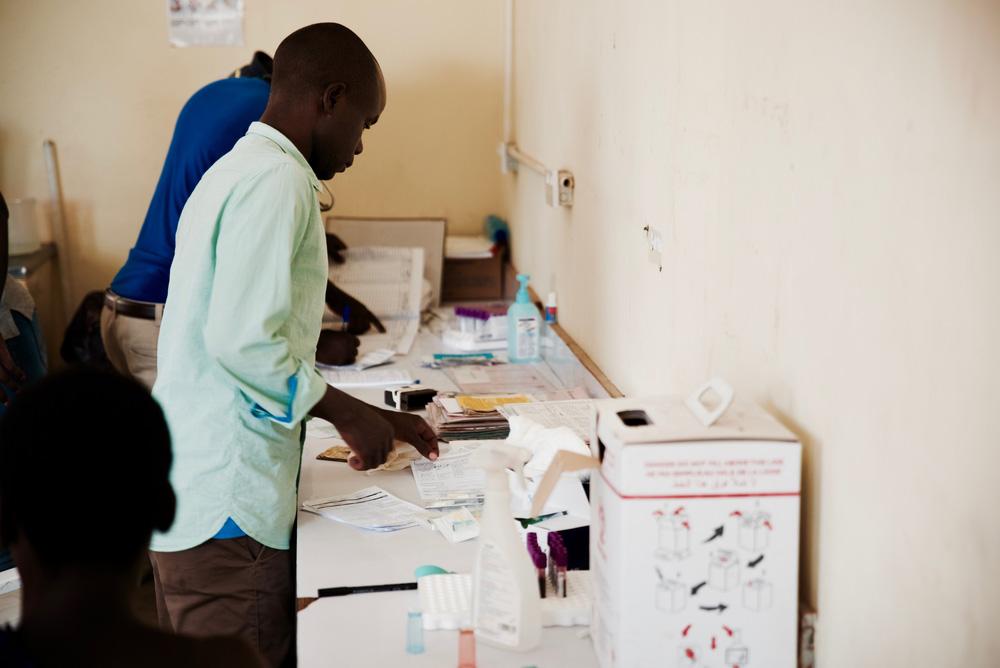
MSF first began HIV/AIDS prevention and control activities in Malawi in 1994 in the district of Mwanza before expanding to Chiradzulu in 1997, where 20 per cent of the district’s adult population was estimated to be HIV-positive. In August 2001, MSF started a programme to provide free access to Anti-Retroviral Therapy (ART) at Chiradzulu’s district hospital. Before this date, no HIV treatment was available in the country, and medical action regarding people suffering from AIDS was limited to preventing and treating opportunistic infections. According to UNAIDS, some 86,000 people died of AIDS-related causes in Malawi in 2001.
Fred Minandi, a retired farmer, proudly recalls that he was the fourth patient to receive ART in the Chiradzulu project on 16 August 2001 at the age of 41.

MSF HIV in Malawi, Video Testimony of Fred Minandi
“In those days (1990s-2000s) it was very bad, people were dying. I lost my brother and my sister to AIDS. When I was sick, I had no hope. At that time no one was receiving ART until MSF began providing it,” Fred explains. “In 1999, I went for an HIV test at Chiradzulu district hospital. I was not working anymore because I was too sick and had been suffering from opportunistic infections since 1997. I tested positive to the virus. Later, I met with MSF counsellors who told me they were going to begin dispensing ART. I was lucky to be one of the first patients to receive treatment. After a month, I was able to start work again.” - Fred Minandi
The story of the project in Chiradzulu is not just about providing drugs to patients. It proved it was possible to tackle HIV in poor rural settings and that patients would comply with the strict HIV treatment routine, an idea met with significant cynicism at the time. The project set a precedent and helped pave the way to advocate for cheaper drug prices and ensure access to ART in low-income countries.

In July 2002, Fred was invited to speak at the 14th International Conference on HIV/AIDS in Barcelona, where MSF’s presentation on “Access to ART in MSF programmes” included the Chiradzulu experience.
“I am one of the first patients to benefit from free treatment in Malawi and if I am here to talk to you about it today, it’s because I am receiving treatment. Some of you will say that Africans cannot take medicine properly because we don’t know how to tell time. I don’t have a watch, but I can tell you that since I began my triple therapy, I have never forgotten to take a single dose,” Fred told the conference.
By the end of 2003, more than 2,000 patients were on ART in the Chiradzulu programme, at an average rate of 200 new patients per month, showing clinical results comparable to those found in high-income countries.
As the years went by, scaling up the number of patients receiving ART was made possible by simplifying treatment approaches, decentralizing care to peripheral healthcare facilities and task-shifting certain tasks from medical to para-medical – and even non-medical – staff. Advances in treatment strategies also allowed patients in stable condition who had been on treatment for at least a year to have their medical consultations once every six months instead of every two to three months. This six-month appointment (SMA) system helped reduce the burden on patients and medical staff.
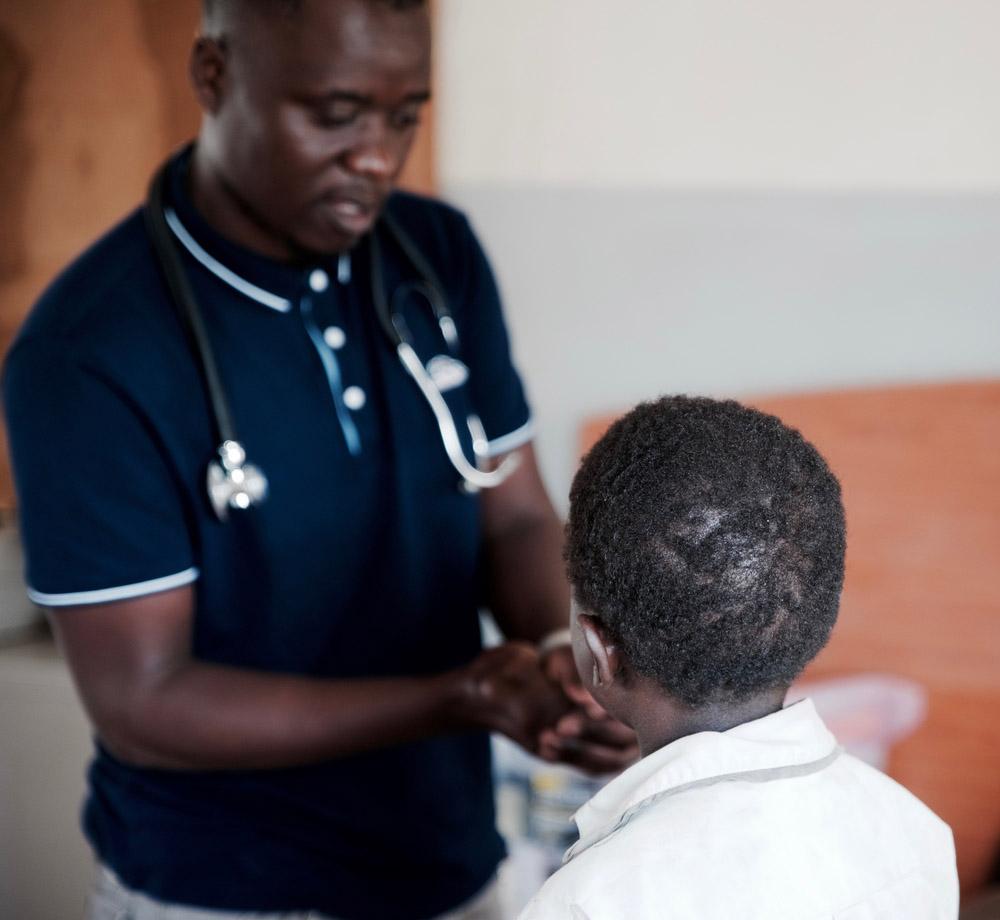
The collaboration between MSF and the Ministry of Health, along with this model of decentralization and task-shifting, contributed to shaping policies and guidelines in Malawi on the care and treatment of people living with HIV.
By 2009, every health structure in the Chiradzulu district could provide a range of services for HIV/AIDS patients, from testing to prevention of mother-to-child transmission (PMTCT) and treatment of Tuberculosis (TB) co-infected patients.
In 2013, an MSF study in the district showed that 65.8 per cent of people needing ART were receiving the appropriate medicines, and a population-based survey revealed that there was also a very low level of new infections (0.4 per cent), suggesting that the large provision of HIV treatment had played a role in reducing transmission.
Such progress was made possible by the partnership between MSF and local health authorities and by the patients themselves. Patients such as Fred formed support groups and were employed by MSF as peer care counsellors to encourage people to get tested and help patients comply with their treatment.

“This approach of having care-givers team up with peer counsellors empowered patients to take charge of their care and support others in their treatment journey,” Fred recalls of his days as a peer counsellor at Mauwa health centre in Chiradzulu district.
While people living with HIV face many of the same issues regardless of their age and circumstances, over time, it became clear that children and teenagers face specific challenges of their own, needing extra attention and dedicated care. With patients sometimes under ten years old, even the simple explanation of what HIV-positivity is and what it means for one’s life can be complicated; other patients might just be approaching sexual maturity and struggle to come to terms with the fact that they live with a sexually transmittable disease.
MSF started dedicated Saturday "Teen clubs" in 2017 and continued to run them until the end of 2022, offering HIV care, follow-up, sexual and reproductive health services, and psychological and social support to teenagers living with HIV. Attendance at these clubs, which provided a safe, friendly space where teenagers could also benefit from peer support, showed enhanced adherence to treatment and contributed to a patient’s overall well-being.
For many of these adolescents, attending "Teen clubs" helped them transition from being overwhelmed by a condition they struggle to make sense of to be better prepared to tackle it. In 2019, as many as 9,200 adolescents attended the clubs in Chiradzulu district.

After over 20 years of collaboration with MSF, Chiradzulu district health authorities and their partners fully took over all patients and activities between 2022 and 2023, ensuring the continuity of HIV treatment and care.
Malawi has one of the highest HIV prevalence rates in the world, with 990,000 people (UNAIDS, 2021) living with the virus out of a population of nearly 20 million. Projects such as the one in Chiradzulu set a benchmark in Malawi for HIV care. In collaboration with MSF and other partners, the country scaled up HIV prevention and treatment programmes resulting in great strides. Of 990,000 people living with HIV, 93 per cent know their status, 91 per cent are on ART, and 85 per cent have suppressed viral loads (UNAIDS 2021).

When I go for viral load testing nowadays, the virus is undetectable.Fred Minandi, HIV Patient
“When I go for viral load testing nowadays, the virus is undetectable. In 2001, when the counsellor said ART could prolong my life, I thought it would be two to three years but here I am, 22 years later,” 63-year-old Fred says with a cheerful grin.
Overall, 55,000 people who tested positive for HIV were enrolled in the Chiradzulu cohort between 2001 and the closure of the project in 2023.