“This project was the toughest thing I ever did!” says Zimbabwean nursing director Gilberta Jairos, who arrived in Kenema, Sierra Leone, for her sixth international assignment just a few months after MSF’s paediatric hospital had opened. Given how new the hospital and its staff were, a huge training task lay ahead of Gilberta, and her job was made even more challenging with the outbreak of COVID-19.
Sierra Leone has one of the world’s highest maternal and child mortality rates. Each year over 1,300 women die during or after childbirth. A fragile health system and lack of health workers, caused in part by the 2014 Ebola outbreak, are among the factors that cause a high number of deaths of children under five. The Kenema hospital, which opened in March 2019, is now a crucial lifeline for many seriously ill children and mothers.

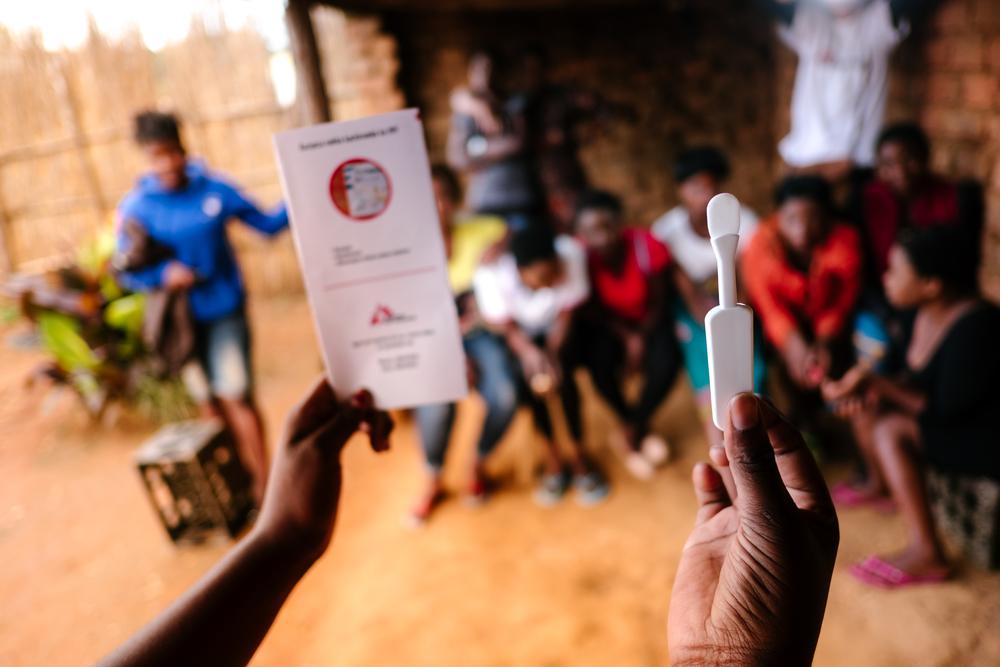
Gilberta explains that since the Ebola outbreak of 2014 and the arrival of COVID-19 in March, there is a general mistrust in hospitals among the community. “Because of the high mortality rate and the fact that Ebola patients would often arrive too late to the hospitals, many people believed that it was the hospital that led to the person’s demise.” This, together with a strong reliance on traditional medicine, makes health education and promotion a priority in the local communities.
“We tell people that malaria can be treated and urge them to bring their children to the hospital to be monitored, but they’re afraid. Those Ebola times really affected them, and now there’s the fear of COVID-19. I think it will take some time for attitudes to change.”
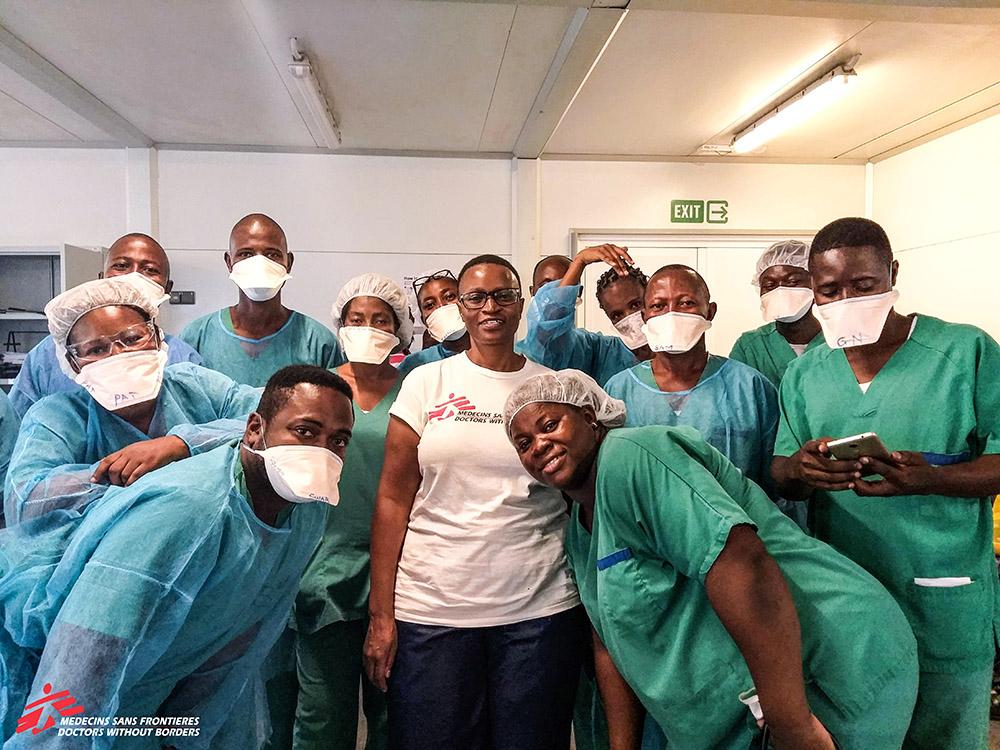
As an MSF nursing director, Gilberta was responsible for the nursing team and making sure that the nursing care across all departments was running well. “I tried to make sure that the nurses were well-trained and that the supervisors could run their departments,” she says. “Most of the international staff had been working on the opening of the hospital, so many were preparing to leave and new supervisors were coming in. I had to quickly understand the ins and outs of the project so that I could train the new staff.”
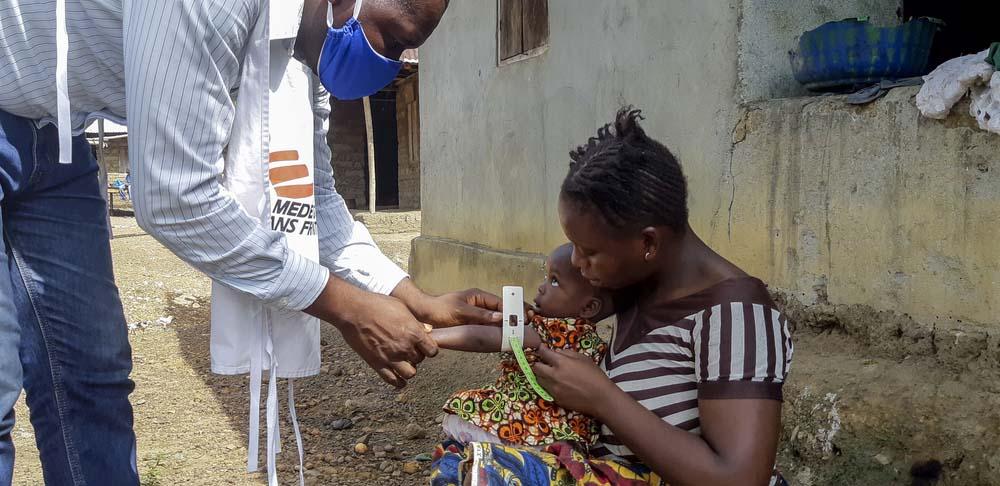
While Gilberta’s role was managerial, she regularly met patients on her rounds, with the most common illnesses among the young children and babies being malaria, pneumonia, diarrhoea or malnutrition. “Most of the malaria patients were complicated cases who came in very late. Babies are often kept at home and only brought in when critical. Unfortunately, some children are intoxicated from traditional medicine when they come to the hospital or they have organ failure.

“There was one child who came in and we didn’t know if she would make it. She had *sepsis. She arrived unconscious and we thought it was meningitis, but she was actually septic from malaria. When we did a **lumbar puncture, the fluid that came out was puss. That spinal fluid circulates in the brain, so we had little hope for the child. But she ended up going home after making a full recovery. And this is not the only case.
There were so many children you would see fighting for their lives… When you get a very bad case you think: I hope this one will fight, but many of these children die.”
*Sepsis is a very serious and potentially life-threatening immune response that occurs when the body's reaction to infection causes injury to its tissues and organs.
**A Lumbar puncture is a medical procedure in which a needle is inserted into the spine to collect cerebrospinal fluid for testing to diagnose certain diseases such as meningitis.
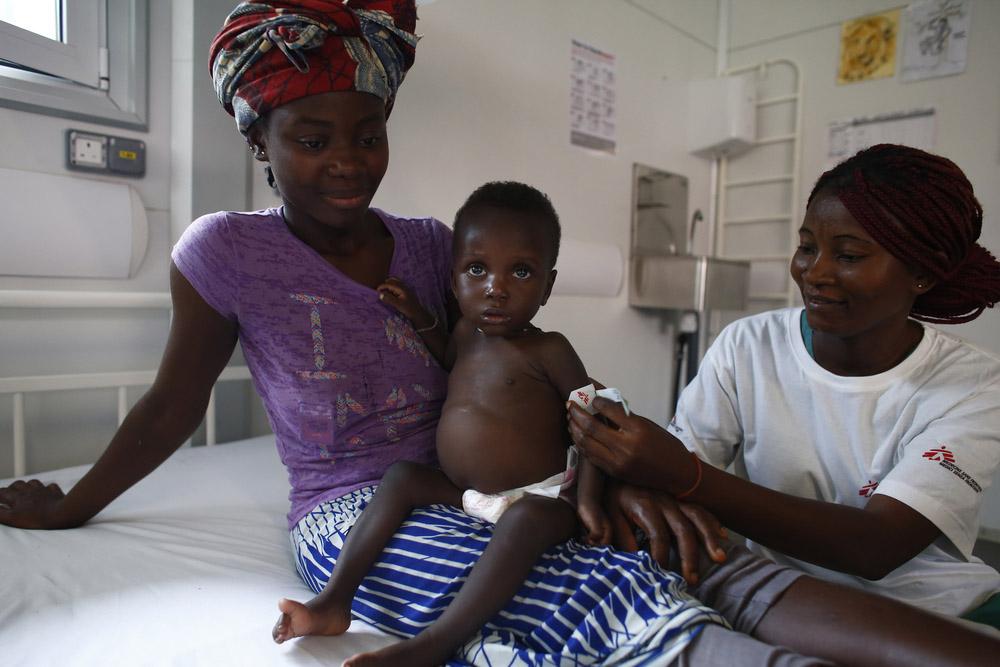
The MSF hospital is a 10-year project that will be completed in phases. Currently, it provides a lab and blood bank, alongside paediatric services that include an emergency room, a paediatric intensive care unit, an inpatient therapeutic feeding centre, two general paediatric wards and an isolation ward for suspected Lassa fever cases. Construction has now begun on a maternity and neonatal unit, which will bring the total hospital capacity to 149 beds.
“By year four or five of the project we hope to have fewer international fieldworkers being sent to Kenema, so we need to make sure we empower the locally-hired staff who will be running the hospital,” Gilberta says.
“At first there was a lot of work to do with the nurses. I pushed the supervisors to delegate and become managers. Being a manager means watching and managing everything that is going on administratively and clinically.
As we trained the supervisors, you could see their confidence growing. This confidence trickles down to the nurses. I was confident in them, but sometimes you need someone to tell you that you can do it.”

Despite her mammoth training task, Gilberta is incredibly proud of the upskilled team she left behind. “My vision was to create confident managers, and this is what happened,” she says. “When COVID-19 emerged for some time we were unable to bring new staff into the country but we managed because we had built such a strong team.
“I said to myself that I would not go back home, even though there were times I wanted to. I could not leave my team as they became like my family, and you can’t let the family down.”
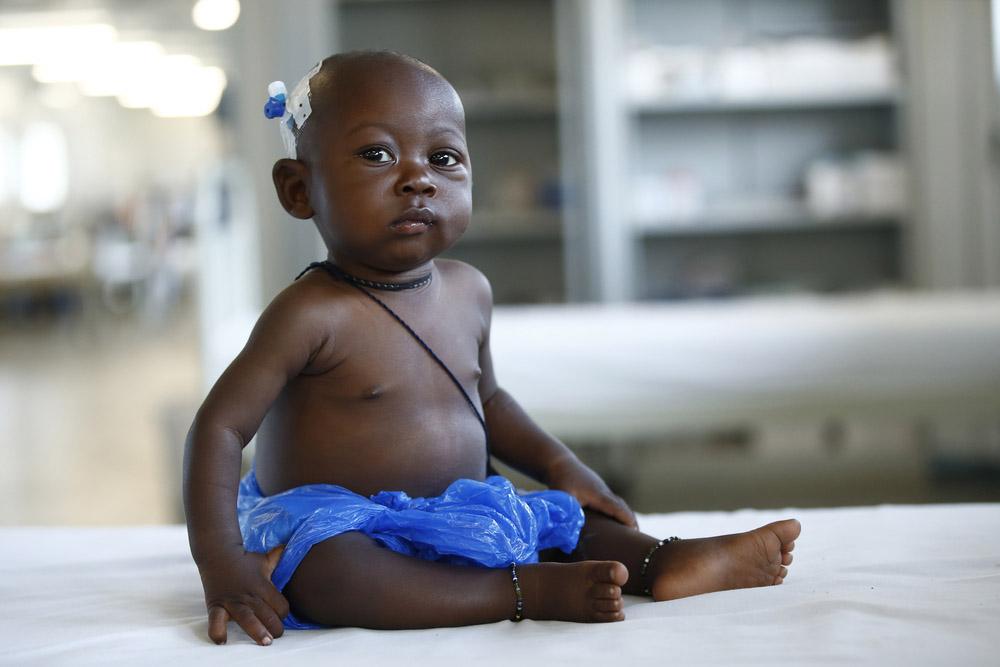
MSF has worked in Sierra Leone since 1986. In 1995, MSF sent teams to provide assistance to displaced Sierra Leoneans during and immediately after the decade-long civil war. MSF also launched a large-scale response during the Ebola outbreak of 2014-16. MSF currently works in three districts – Kenema, Tonkolili and Bombali – providing medical care and supporting initiatives to strengthen the country’s health system.