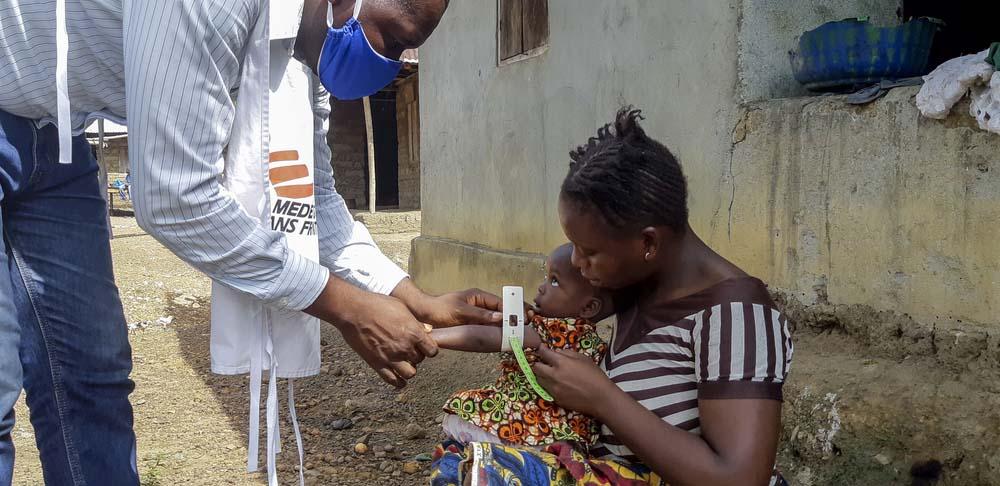
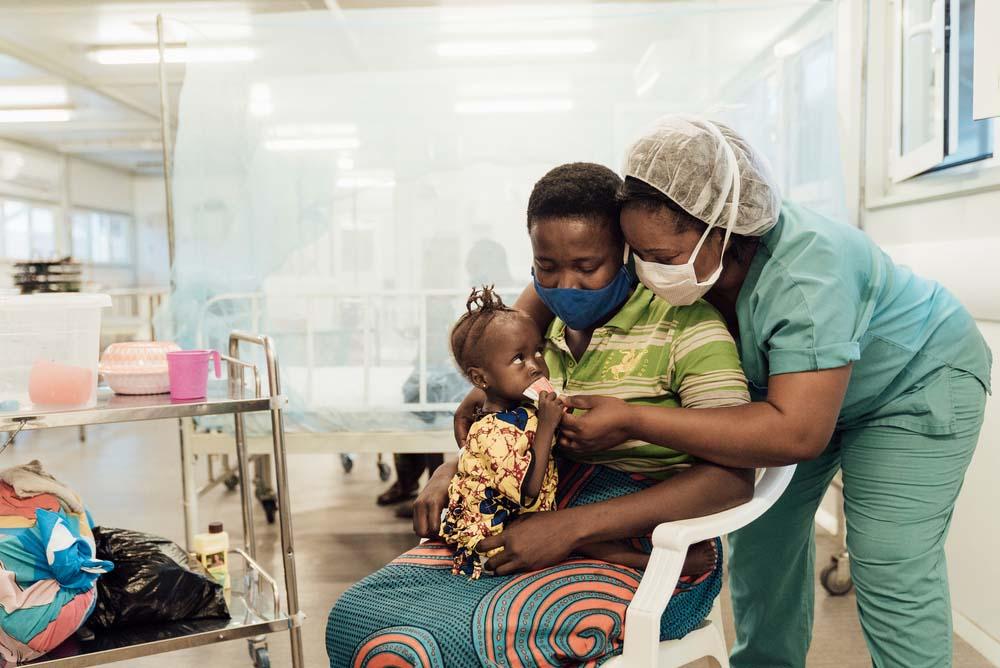
Gift Farau, a nursing supervisor from Zimbabwe, spent a year at the MSF Hangha hospital in Kenema, Sierra Leone from August 2019. In this article he sheds some light on what an Inpatient Therapeutic Feeding Centre (ITFC) is all about and the impact the hospital’s ITFC is making on the historically high infant mortality rates linked to severe acute malnutrition.
The inpatient therapeutic feeding centre
The main objective of the feeding centre is to try and get a child to regain their health. When they are at home, they might not be feeding well because they don’t have the appropriate food, or they’re sick and unable to eat. At the ITFC we provide comprehensive management: including therapeutic food with the correct nutrients, and we also address acute and chronic medical conditions that may be a cause of severe malnutrition.

We have a three-hourly feeding programme for the children. Before feeding them you have to stimulate them. To do this, we try to create a patient-friendly environment, but because there are quite a few infants in the centre, you have to create an individual relationship with the patient and caretaker. If the children have a good relationship with the person who is feeding them, they will be encouraged to eat properly. While the nurses initially do the feeding, the main objective for us is to train, support and assist the mothers to feed the children themselves.
Quality of eating
Sometimes the parents look more at the quantity of food the child is eating and not how they are eating. For example, a child may take in the quantity that we would expect, but if they vomit soon after then their tiny bodies are not getting the nutrients the need. Ideally, we want the children to eat 100% of the meal but if they can’t, it’s better to get them to eat gradually and have a gradual recovery. When it comes to feeding, it’s often quality over quantity.
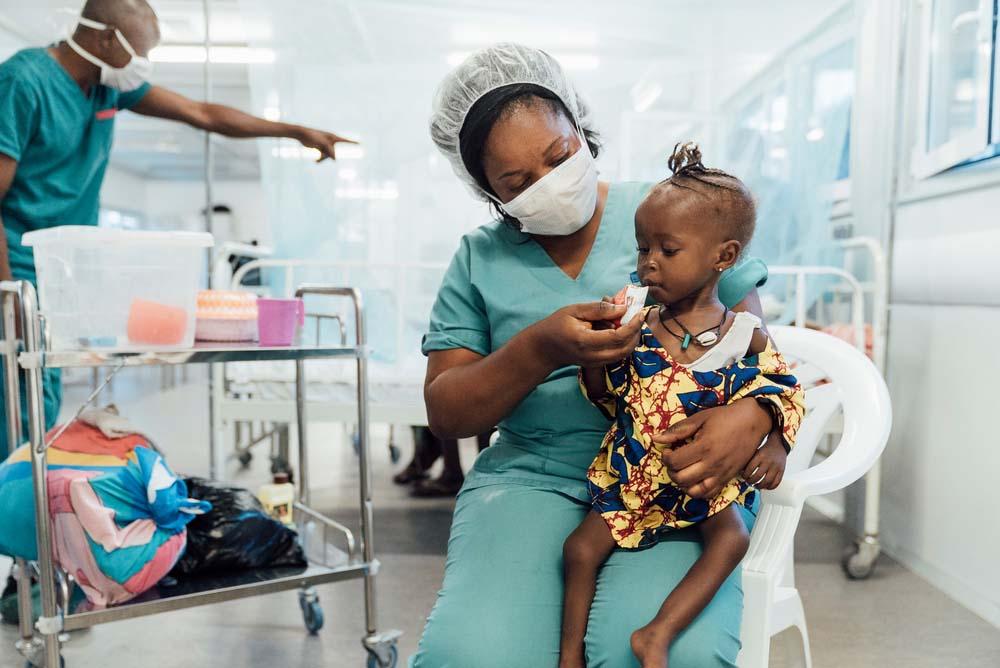
Difficult cases
I am proud of how we managed some very complicated cases at the ITFC that the nurses had struggled to cope with before. Some nurses were so afraid of these cases because in the past many of these young patients would die. But we managed; we attended to them and many recovered. Difficult cases included kwashiorkor, one of the most severe forms of malnutrition, which can result in complicated skin lesions. Kwashiorkor is characterised by a child having oedema, or a swelling of every part of the body, which makes the skin very fragile. If the skin tears then it can cause wounds, and the healing of these wounds is complicated by the fact that the child is already suffering from malnutrition. A child’s body needs to be properly nourished for the wounds to heal.
Malnourished children are also at a high risk of acute respiratory infections, which was another complicated condition treated in the hospital. And, of course, there is malaria which is the main cause of death for children under 5 years in the country.
Sharing valuable knowledge with communities
Health education plays a crucial role in the success of a hospital like ours and the recovery of our patients. Many parents are not aware about how to feed correctly their children. They might just follow the same feeding pattern that they received or saw growing up; they might not understand that while it’s okay for an adult to eat rice, the nutritional value for a child is not sufficient and can contribute to malnutrition. From the experience that I had in the year that I was in Kenema, I can honestly say that most of the problems we saw came from a lack of knowledge around childcare.
To address this, we ran a health promotion programme for mothers and caregivers twice a day in the hospital. In the morning and afternoon, health promoters sit with the parents and share with them all the factors that could contribute to child malnutrition. They would teach them about nutrition and discuss what food is appropriate for children. The health promoters would find out what the mothers have in their homes and give advice on what and how much the children should eat. They encourage the mothers to also share what they have learnt with the rest of their community when they return home.
It is important that the community in Kenema district first understood why malnutrition is a problem and what we were trying to do. If people don’t have the knowledge about what you are doing they won’t use your services.
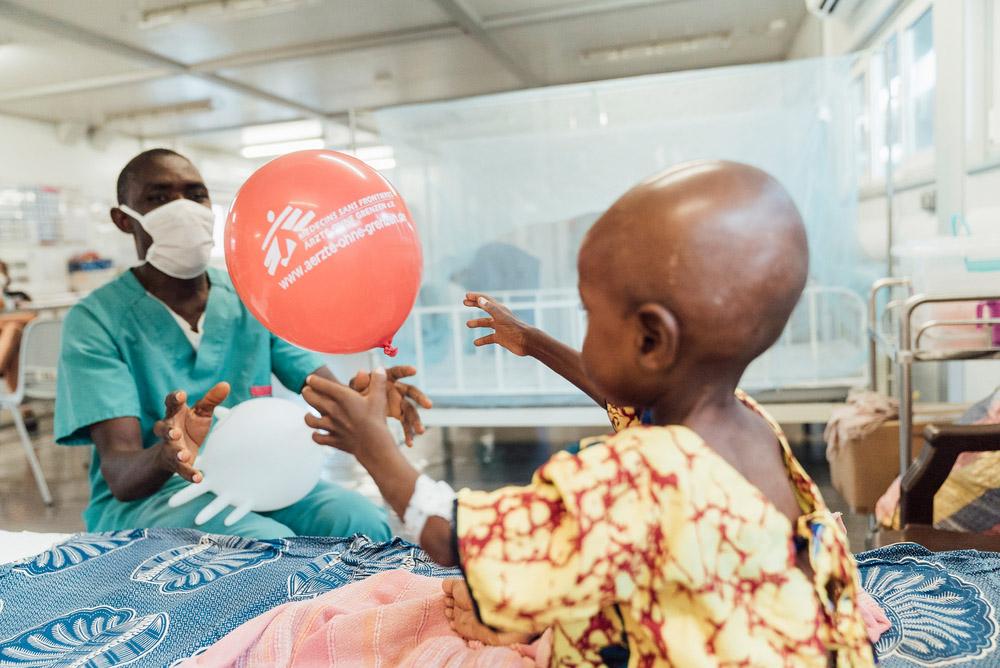
Making an impact
What I enjoyed most is seeing the impact that MSF is having in the community. In Sierra Leone, the consequences of civil war, Ebola, cholera and Lassa fever left communities disabled and it was hard for the government to cope. MSF is able to work alongside the government health facilities to help meet the demand for quality medical care and ensure access to primary and secondary care
MSF has worked in Sierra Leone since 1986. In 1995, MSF sent teams to provide assistance to displaced Sierra Leoneans during and immediately after the decade-long civil war and also launched a large-scale response during the West African Ebola outbreak of 2014-16. MSF currently works in three districts – Kenema, Tonkolili and Bombali and runs its own medical projects while supporting the Ministry of Health and Sanitation (MoHS) in providing primary and secondary healthcare. MSF’s current activities focus on children, pregnant and lactating mothers, TB patients and survivors of gender-based violence.