

Pakistan
In Balochistan, a region with alarmingly high maternal death rates, we supported reproductive health and neonatal services in Kuchlak, Chaman, and east Balochistan.
We also offered nutrition care for children, lactating women, and pregnant women.
Our activities in 2024 in Pakistan
Data and information from the International Activity Report 2024.
964
964
€12.3 M
12.3M
1986
1986
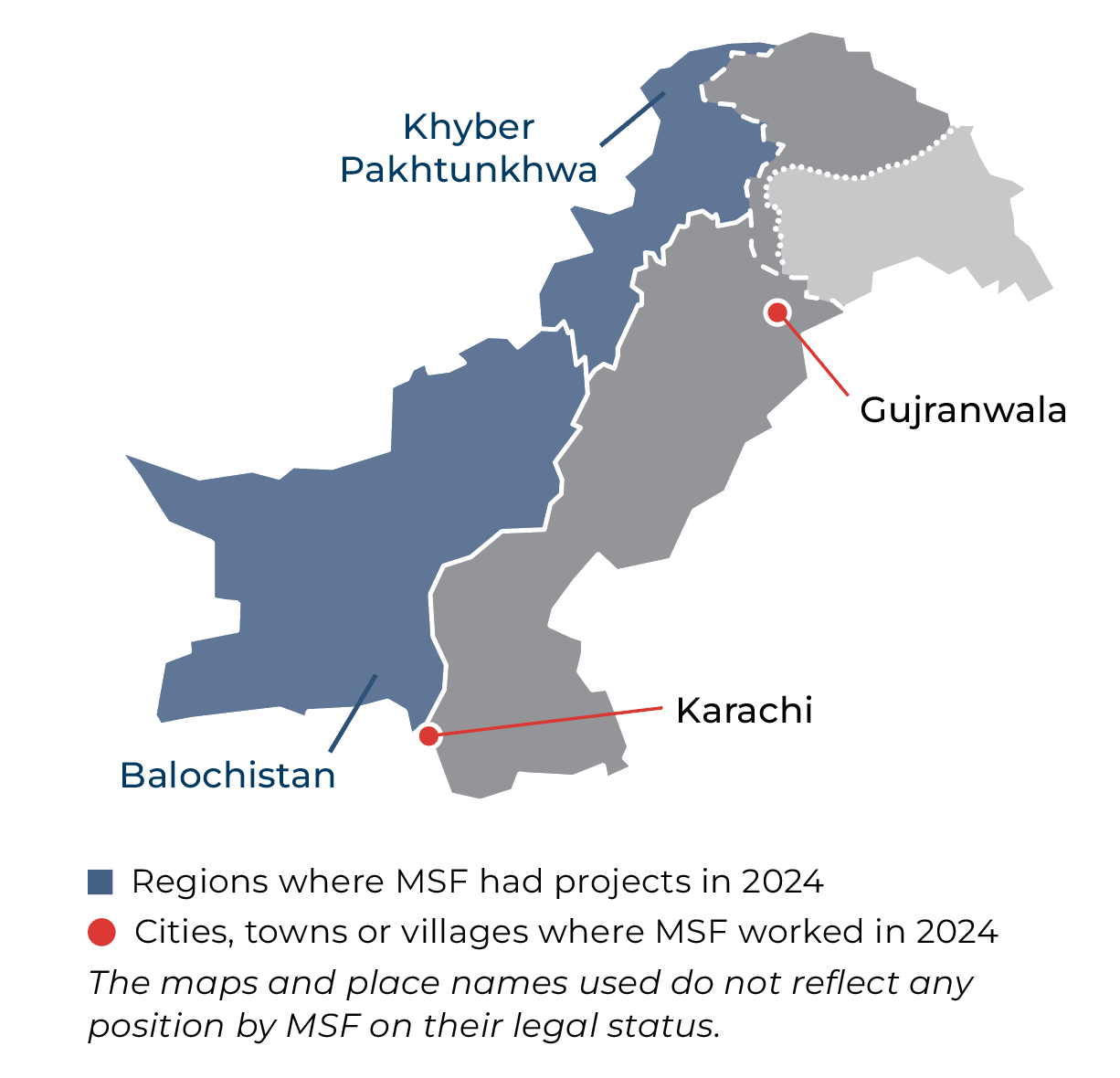
In 2024, we continued our programme, which focused on treating cutaneous leishmaniasis, a neglected tropical disease that causes skin lesions, across Balochistan and Khyber Pakhtunkhwa. During the year, our clinics treated nearly 10,000 patients. In addition to diagnosis and care, we offered mental health support, and conduct research into improved treatment options.
In Khyber Pakhtunkhwa's Tirah valley, where communities are rebuilding their lives after being displaced by conflict, we provided basic healthcare, and in 2024 responded to a significant malaria outbreak. Our presence ensured access to vital medical services in a fragile environment.
Our drug-resistant tuberculosis (TB) programme in Gujranwala, Punjab, implemented a patient-centred approach, offering injection-free, shorter, and more effective treatment regimens, and comprehensive and tailored psychological and social support. In addition, we conducted systematic household contact screening, targeting children under 15 years of age, to improve diagnosis and treatment of paediatric TB.
In 2024, we concluded our nine-year hepatitis C project in Karachi’s Machar Colony. This programme delivered free, lifesaving treatment, and demonstrated how a major health crisis can be effectively addressed through sustained efforts within an urban community.
IN 2024

14,900
14,9
11,200
11,2
6,770
6,77
490
49


Pakistan floods: “So many people needed help”
Innovative TB trial starts in Sindh province, Pakistan

Working to turn the tide of hepatitis C infection in Karachi’s Machar Colony

Fezile Kanju: "What we consider work is actually life-changing to the people we treat”
