MSF has been working with the key populations since 2014 and is developing several approaches to improve their access to healthcare.
“My life changed a lot with MSF. Before, I didn’t even believe HIV existed. I used to attend the traditions [alternative traditional medicine]. After joining MSF, I started reducing my exposure [to sex] without a condom and teaching others to do the same. When I manage to help one person, it means a lot to me. It feels like a victory, because I’m helping save lives.”
This sex worker, who wishes to remain anonymous, works for Doctor Without Borders (MSF) as a peer educator in Beira, providing health promotion information in the community to other sex workers. Since 2014, the international medical organisation has worked alongside the Ministry of Health and other partners to increase access to healthcare for sex workers and men who have sex with men. They are considered ‘key populations’ as they often face difficulties accessing healthcare. To help bridge the gap, MSF is working with peer educators – themselves sex workers and men who have sex with men who have been recruited from their local communities and trained to raise awareness about HIV among their peers.

The programme was established along the main transport corridor between Mozambique, Malawi and Zimbabwe, with the aim of adapting health services to reach groups identified as being the most vulnerable to HIV. Previously known as the ‘Corridor project’, with 4 sites in Malawi and 2 in Mozambique, it initially focused on long-distance truck drivers and sex workers but over time has expanded to provide support to others at risk of HIV and with equally high needs, namely adolescents and young women engaged in transactional sex, and men who have sex with men.
At over 13 per cent, Mozambique has one of the world’s highest rates of HIV according to the last Ministry of Health survey (IMASIDA 2015). Many of the ‘key populations’ who are most at risk of contracting HIV, as well as sexually transmitted infections (STIs) and unwanted pregnancies, also experience significantly reduced access to preventive sexual healthcare, including HIV testing and treatment, mainly due to stigma and discrimination.
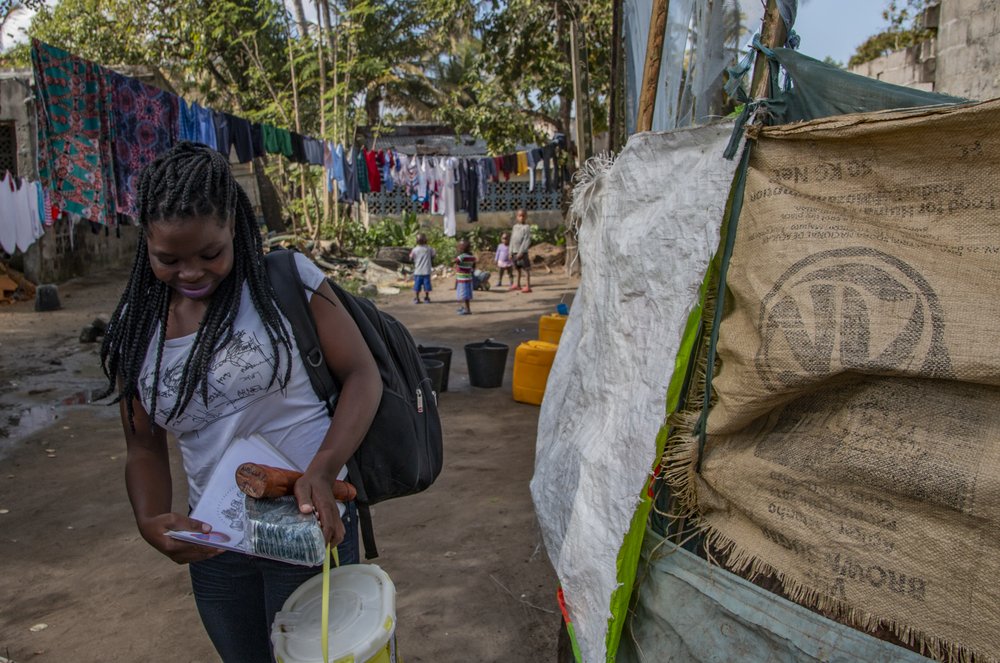
Working with peer educators and assigning them the task of HIV testing in the community has proved effective in raising awareness about HIV among their peers and increasing acceptance of testing. MSF peer educators in Beira visit hotspots to communicate with known sex workers and men who have sex with men, and identify people who are new to the area. Initially, fewer than 30 per cent of the sex workers who enrolled in the MSF programme were aware of their HIV status. Thanks to our peer-led approach, we have now reached over 90 per cent.
“My strategy is to open up that I am a sex worker too,” explains one peer educator, who wishes to remain anonymous. “They first need to trust me so I can start offering the services. It won’t work if you offer HIV testing straight away. I tell them we are enrolling those ladies who have two boyfriends or more. I also have my own network, so when a new sex worker arrives to the area, they call me and ask me to come.”
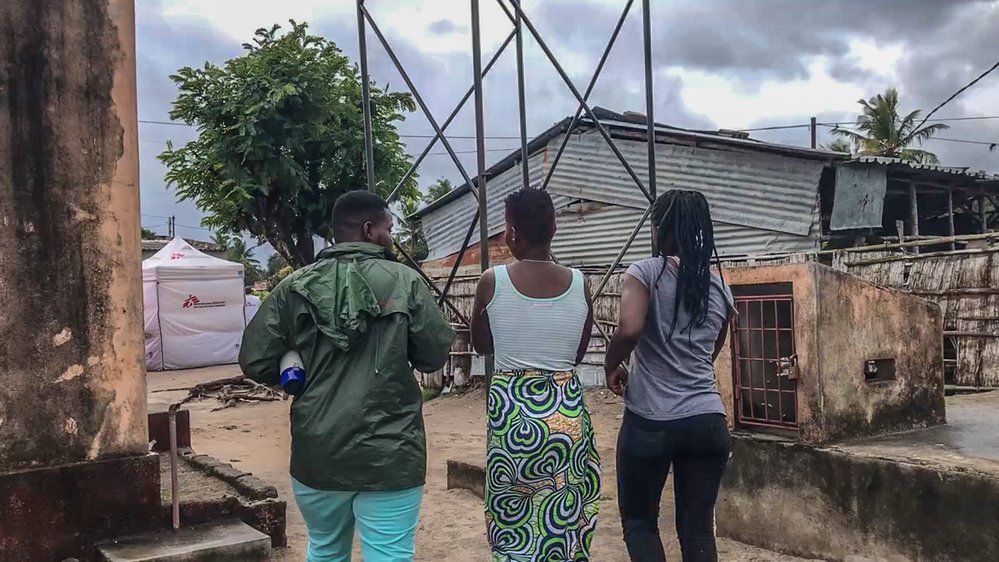
Additional strategies have been developed alongside the peer-led approach to increase key populations’ access to HIV prevention and care and sexual and reproductive healthcare. A basic package of care is offered at community level, bridging barriers such as discrimination at health centres, with referrals for more comprehensive medical treatment. The basic package comprises of health promotion and education on topics such as HIV, sexual and reproductive health, and sexual and gender-based violence, but also the distribution of condoms and lubricants, HIV testing and counselling, post-exposure prophylaxis, and referrals to the Ministry of Health for antiretroviral (ARV) services.
Between 2014 and 2018, over 6,000 people have accessed care in Tete’s (which was handed over in 2018) and Beira’s MSF projects.
