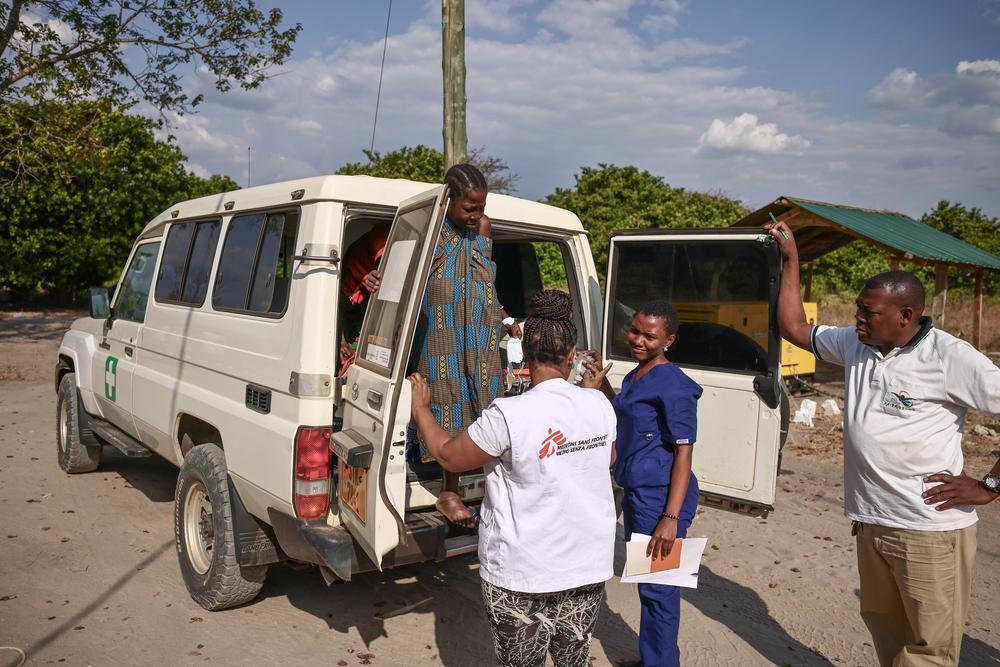In the high-stakes world of humanitarian medicine, there is a silence every midwife fears. It is the stillness of a delivery room where a newborn does not cry, or the heavy stillness of a mother whose body is failing her. My life’s work has been about breaking that silence, replacing it with the sound of a first breath, a baby’s cry, or a mother’s exhausted sigh of relief.
I have spent my career pursuing those moments across borders, from the vast Somali refugee camps of Dagahaley in Kenya to emergency settings shaped by conflict. Today, I lead a midwifery team in rural southern Tanzania, where the challenges are immense, but the goal remains simple: no woman should lose her life while giving life.
My journey into humanitarian midwifery began in Dagahaley refugee camp. There, I witnessed how displacement strips women of safety, stability, and access to care at the very moment they need it most. I quickly learned that maternal healthcare in crises is not just a medical service; it is an act of humanity.
Those years shaped my understanding that saving lives requires more than clinical skill. It requires trust. You must listen, understand cultural beliefs, and respect the fears women carry. Whether in a refugee camp or a district hospital, the principle remains the same: stay adaptable, stay respectful, and never lose sight of the individual woman before you.

In Liwale, the setting is rural, but the emergencies are acute. I was drawn to this project by its fierce commitment to reducing maternal mortality. Here, the landscape itself is an adversary. Women live in remote areas, separated from the hospital by difficult terrain and a lack of transport. By the time a mother reaches us, she is often in a state of crisis, presenting with complications that could have been managed if caught early: haemorrhages, obstructed labour, and convulsions from eclampsia.
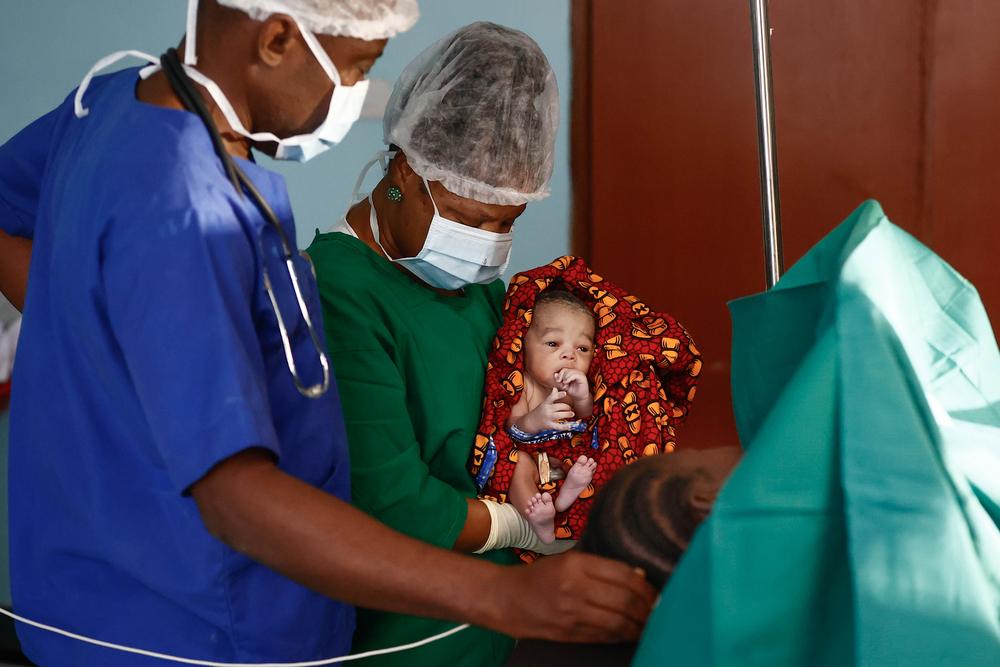
As Midwife Activity Manager, my role goes far beyond administration. I believe deeply in hands-on leadership. You will find me in the maternity ward, working alongside midwives during emergency obstetric and neonatal care situations. I see my responsibility as strengthening both systems and people. The lessons I learned in earlier humanitarian settings guide how I mentor junior staff here. We emphasise strict adherence to Doctors Without Borders MSF and World Health Organisation protocols because in resource-limited environments, protocols save lives.

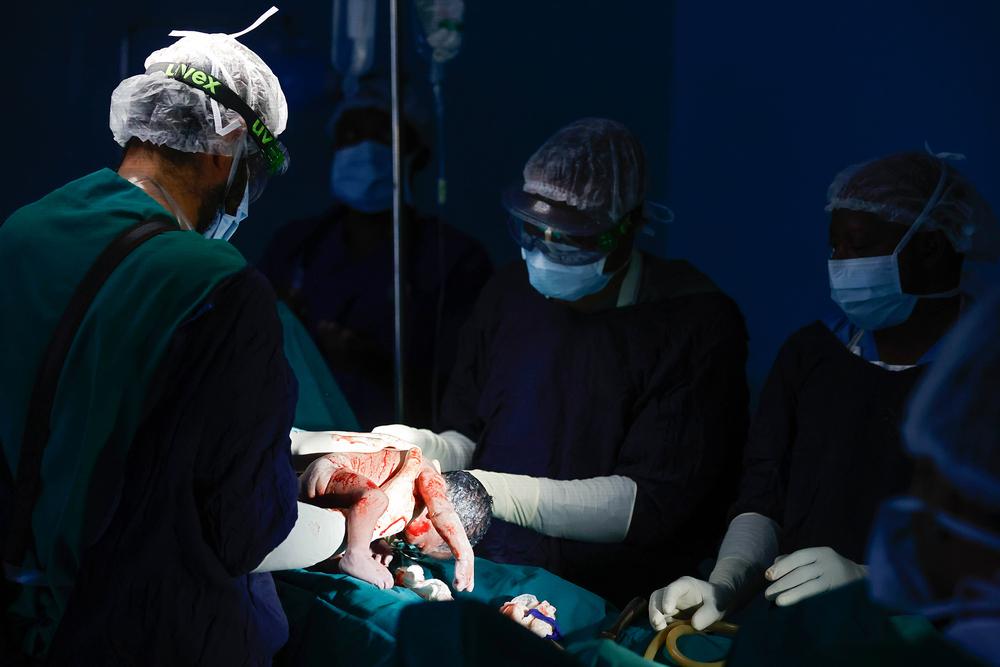
One afternoon tested everything we had built. Within a short period, four women arrived at our facility, all with severe obstetric complications. Each required an emergency cesarean section. In a rural district hospital, this is not just a busy day; it is a crisis. The tension was intense. Decisions had to be made quickly. Because we had invested heavily in capacity building, teamwork, and surgical preparedness, the response was precise. The team stabilised, prioritised, and operated efficiently. All four women survived. All four babies survived. Walking into the ward the next morning and seeing healthy mothers holding their newborns was a powerful reminder of why preparation matters. Those moments sustain us.

One of our deepest challenges isn't medical, but cultural. In Liwale, practices like child marriage lead to teenage pregnancies, putting young girls at high risk for complications because their bodies are not physically ready for the toll of childbirth. Navigating this requires more than medicine; it requires engagement. We work with local leaders and conduct community outreach to promote facility-based deliveries. We want families to understand that the hospital is a place of safety, not fear. Success here is not measured only in numbers, but in changing attitudes. Each time a family chooses to seek care early, we know progress is being made.

Resource limitations remain a constant reality. Shortages of essential medications and equipment challenge us, but delays in seeking care remain the greatest threat. Too often, women arrive only after traditional methods have failed or after hours of travel on motorbikes. Strengthening referral pathways and ambulance services has been critical in reducing these delays and improving outcomes.
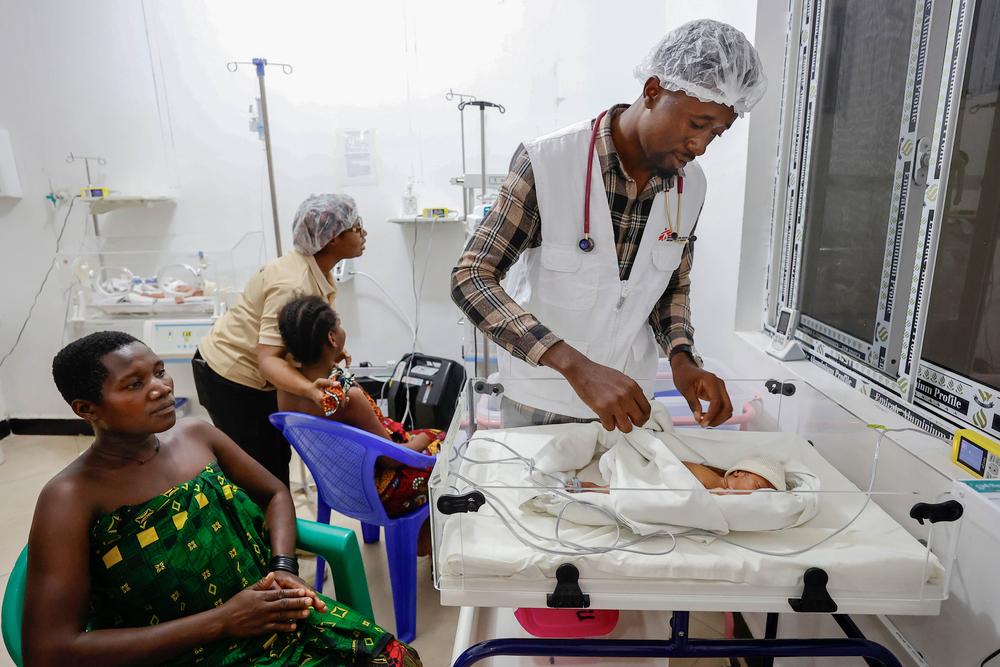
We drill for postpartum haemorrhage until the team moves like a single, synchronised machine. Capacity building is the heartbeat of our project, focusing on the "Big Four" life-savers: managing haemorrhage, treating eclampsia, neonatal resuscitation, and infection prevention. I facilitate case reviews and debriefings after critical incidents, not to find blame, but to find lessons. When a junior midwife gains the confidence to manage a complication independently is one of the most meaningful indicators of impact.
One case remains vivid in my mind. A woman arrived after experiencing convulsions at home. She was critically ill, and both her life and her baby’s were at risk. Without a functioning referral system, she might not have survived. But because the system worked, we intervened in time. Today, she is back in her community, raising her child. That outcome represents everything we strive for.
To young midwives aspiring to humanitarian work, I offer this: this path demands more than technical training. It requires resilience, cultural humility, and the ability to remain calm in crisis. You must believe deeply that every life is worth fighting for. Looking ahead, our priorities remain clear: improving emergency access, strengthening referrals, and addressing adolescent pregnancies. The future of midwifery in rural Tanzania lies in community integration, stronger health systems, and continued investment in people.

Working in Liwale has reinforced a truth I carry with me every day: healthcare is not just about treatment, but about belonging. I am proud of the significant reduction in maternal deaths we have achieved. Every life saved keeps a family whole. Each time a mother leaves the hospital, her baby wrapped in her arms, stepping into the Tanzanian sun, I am reminded why this work matters.
We are not just providing medical services; we are protecting the future of this community. As long as there is a mother in Liwale who needs a safe place to give birth, we will be here. There is no greater honour than being the bridge that brings a mother safely home.